10 Autoimmune Conditions That Are Frequently Misdiagnosed
Autoimmune diseases represent one of the most challenging frontiers in modern medicine, affecting approximately 50 million Americans and creating a diagnostic maze that often leaves patients wandering through years of uncertainty, misdiagnosis, and inappropriate treatments. These complex conditions occur when the body's immune system mistakenly attacks healthy tissues, creating a cascade of symptoms that can mimic dozens of other diseases. The average patient with an autoimmune condition waits nearly five years for an accurate diagnosis, visiting multiple specialists and enduring countless tests before receiving proper care. This diagnostic odyssey is particularly troubling because early intervention is crucial for preventing irreversible organ damage and maintaining quality of life. The overlapping symptoms, lack of definitive diagnostic tests for many conditions, and the subtle onset of many autoimmune diseases contribute to this epidemic of misdiagnosis. Healthcare providers often struggle to piece together seemingly unrelated symptoms, while patients may be dismissed as having stress-related conditions or told their symptoms are "all in their head." Understanding the most commonly misdiagnosed autoimmune conditions is essential for both patients and healthcare providers to recognize red flags, advocate for appropriate testing, and ultimately achieve faster, more accurate diagnoses that can transform lives and prevent long-term complications.
1. Lupus - The Great Imitator's Many Faces
Systemic lupus erythematosus (SLE) has earned the notorious title of "the great imitator" due to its ability to masquerade as numerous other conditions, making it one of the most frequently misdiagnosed autoimmune diseases. This multisystem disorder can affect virtually every organ in the body, presenting with symptoms that range from joint pain and fatigue to kidney dysfunction and neurological complications. The hallmark butterfly rash across the cheeks and nose bridge appears in only about 30% of patients, leaving many without this classic visual clue. Patients are often initially misdiagnosed with fibromyalgia, chronic fatigue syndrome, rheumatoid arthritis, or even psychiatric conditions when neurological symptoms predominate. The diagnostic challenge is compounded by the fact that lupus symptoms tend to wax and wane, with patients experiencing periods of remission followed by unpredictable flares. Laboratory tests, while helpful, can be misleading – antinuclear antibody (ANA) tests can be positive in healthy individuals, while some lupus patients may initially test negative for specific markers. Women of childbearing age, particularly those of African American, Hispanic, or Asian descent, are disproportionately affected, yet the condition is often overlooked in favor of more common diagnoses. The average time to diagnosis ranges from four to six years, during which patients may suffer irreversible organ damage, particularly to the kidneys and cardiovascular system, highlighting the critical importance of early recognition and treatment.
2. Hashimoto's Thyroiditis - The Silent Saboteur of Metabolism
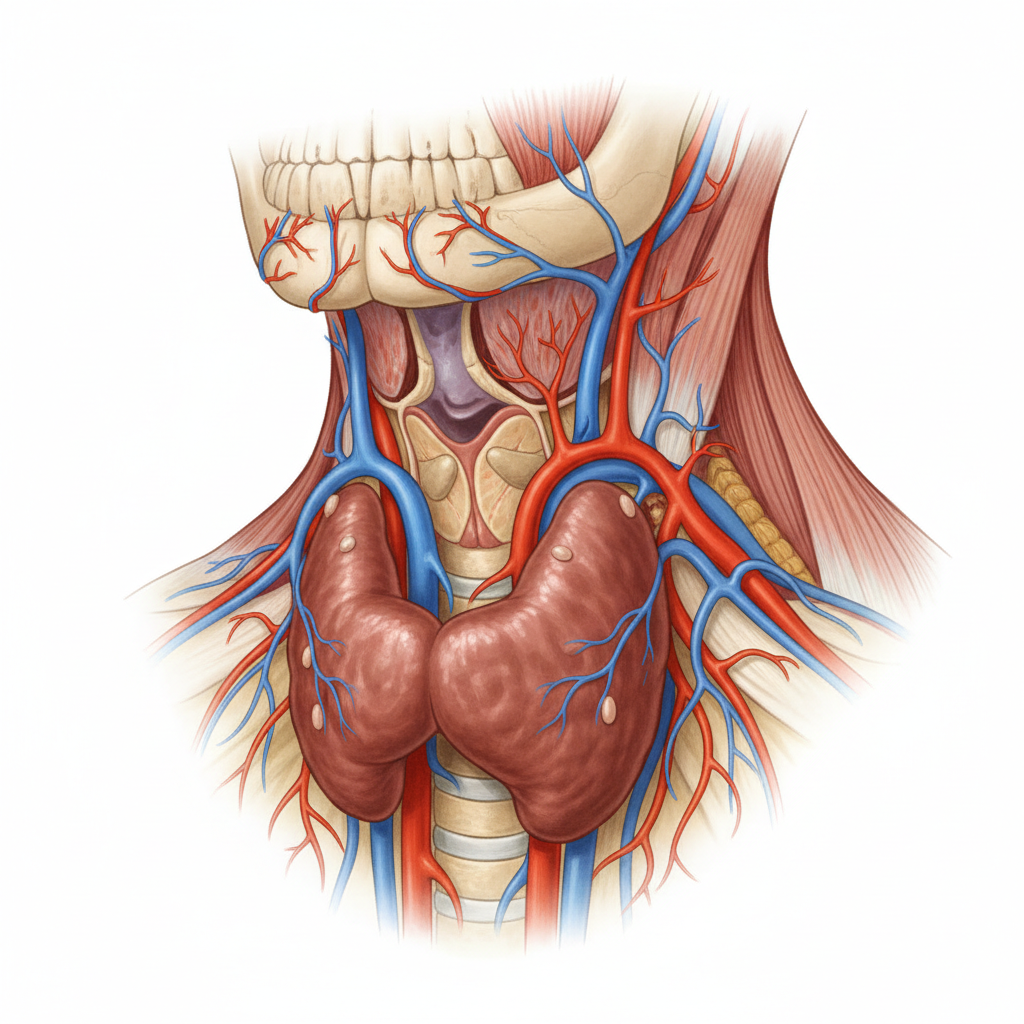
Hashimoto's thyroiditis, the most common cause of hypothyroidism in developed countries, exemplifies how autoimmune conditions can lurk beneath the surface for years before being properly identified. This condition occurs when the immune system gradually destroys thyroid tissue, leading to a progressive decline in thyroid hormone production that can profoundly impact every system in the body. The insidious nature of Hashimoto's makes it particularly prone to misdiagnosis, as symptoms develop slowly and are often attributed to aging, stress, depression, or lifestyle factors. Patients frequently present with complaints of unexplained weight gain, persistent fatigue, brain fog, hair loss, and cold intolerance – symptoms that are easily dismissed or attributed to other causes. Many healthcare providers rely solely on thyroid-stimulating hormone (TSH) levels for diagnosis, potentially missing cases where TSH remains normal despite significant thyroid antibody elevation and tissue destruction. The condition is often misdiagnosed as depression, chronic fatigue syndrome, or menopause-related changes, particularly in women over 40. Subclinical hypothyroidism, where TSH is mildly elevated but thyroid hormones remain within normal ranges, represents a diagnostic gray area where patients experience symptoms but may not receive treatment. The presence of thyroid peroxidase (TPO) and thyroglobulin antibodies confirms the autoimmune nature of the condition, yet these tests are not always ordered during initial evaluations. Early detection and treatment with thyroid hormone replacement can prevent progression to overt hypothyroidism and associated complications including cardiovascular disease, cognitive decline, and reproductive issues.
3. Rheumatoid Arthritis - Beyond Joint Pain

Rheumatoid arthritis (RA) represents far more than simple joint pain, yet this reductive understanding contributes significantly to its frequent misdiagnosis and delayed treatment. This systemic autoimmune condition primarily targets the synovial lining of joints but can affect multiple organ systems, including the heart, lungs, eyes, and blood vessels. The classic presentation of symmetric joint swelling and morning stiffness may not be present in early disease, leading to misdiagnosis as osteoarthritis, fibromyalgia, or viral arthritis. Seronegative RA, affecting approximately 20% of patients, presents additional diagnostic challenges as traditional markers like rheumatoid factor and anti-cyclic citrullinated peptide antibodies are absent. Early RA symptoms can be subtle and intermittent, with patients experiencing joint stiffness that improves throughout the day, fatigue, and low-grade fever that may be attributed to other causes. The condition disproportionately affects women, particularly those between ages 30-50, yet it can occur at any age and in any gender. Palindromic rheumatism, characterized by episodic joint attacks that completely resolve between episodes, often precedes the development of persistent RA but may be misdiagnosed as gout or other crystalline arthropathies. The window of opportunity for preventing joint damage is narrow – ideally within the first three to six months of symptom onset – making early diagnosis crucial. Advanced imaging techniques like musculoskeletal ultrasound and MRI can detect synovitis before it becomes clinically apparent, yet these tools are not always utilized in primary care settings. Delayed diagnosis and treatment initiation can result in irreversible joint destruction, disability, and increased cardiovascular mortality, emphasizing the critical importance of maintaining high clinical suspicion for RA in patients presenting with unexplained joint symptoms.
4. Multiple Sclerosis - The Neurological Chameleon
Multiple sclerosis (MS) stands as one of the most diagnostically challenging autoimmune conditions, with its protean neurological manifestations often leading to years of misdiagnosis and delayed treatment. This demyelinating disease of the central nervous system can present with an bewildering array of symptoms that may appear unrelated and can affect any part of the brain, spinal cord, or optic nerves. Early symptoms such as numbness, tingling, visual disturbances, balance problems, and cognitive difficulties are frequently attributed to stress, vitamin deficiencies, anxiety, or other neurological conditions. The relapsing-remitting nature of MS in its early stages means that symptoms may completely resolve between attacks, leading patients and healthcare providers to dismiss them as temporary or insignificant. Optic neuritis, often the first manifestation of MS, may be misdiagnosed as migraine, eye strain, or other ophthalmologic conditions, particularly when it occurs without obvious visual field defects. The McDonald criteria for MS diagnosis require evidence of lesions disseminated in space and time, but early disease may not meet these stringent requirements, leaving patients in diagnostic limbo. Clinically isolated syndrome (CIS), representing a first neurological episode suggestive of demyelination, poses particular diagnostic challenges as not all patients will progress to definite MS. Primary progressive MS, characterized by gradual neurological decline without distinct relapses, is often misdiagnosed as other neurodegenerative conditions or attributed to normal aging. Advanced MRI techniques and cerebrospinal fluid analysis have improved diagnostic accuracy, yet access to these specialized tests may be limited. The average time from first symptom to diagnosis ranges from two to five years, during which patients may experience disease progression and accumulate disability that could potentially be prevented with early disease-modifying therapy.
5. Celiac Disease - The Hidden Intestinal Autoimmune Response
Celiac disease represents a unique autoimmune condition triggered by gluten consumption in genetically susceptible individuals, yet its diverse clinical presentations often lead to misdiagnosis as irritable bowel syndrome, inflammatory bowel disease, or other gastrointestinal disorders. This condition affects approximately 1% of the global population, but studies suggest that up to 80% of cases remain undiagnosed due to the wide spectrum of symptoms and lack of awareness among healthcare providers. The classic presentation of severe diarrhea, weight loss, and malabsorption represents only the tip of the iceberg, as many patients present with subtle or atypical symptoms including constipation, bloating, fatigue, anemia, or neurological manifestations. Non-gastrointestinal presentations are increasingly recognized and include dermatitis herpetiformis, unexplained infertility, recurrent miscarriages, dental enamel defects, and neurological symptoms such as peripheral neuropathy or ataxia. The condition can manifest at any age, from infancy through elderly years, with adult-onset celiac disease becoming increasingly common and often presenting with milder symptoms that may be overlooked. Silent celiac disease, where patients have positive serology and intestinal damage but minimal symptoms, represents a significant diagnostic challenge as these individuals may not seek medical attention despite ongoing intestinal inflammation. The gold standard for diagnosis requires both positive serology (tissue transglutaminase antibodies, endomysial antibodies) and confirmatory intestinal biopsy showing villous atrophy, yet many patients are placed on gluten-free diets before proper testing, potentially masking the diagnosis. Refractory celiac disease, where symptoms persist despite strict gluten avoidance, may be misdiagnosed as treatment failure when it actually represents a distinct condition requiring specialized management. The consequences of delayed diagnosis extend beyond gastrointestinal symptoms to include increased risks of osteoporosis, lymphoma, and other autoimmune conditions, making early recognition and treatment essential for long-term health outcomes.
6. Sjögren's Syndrome - The Overlooked Moisture Thief

Sjögren's syndrome, characterized by autoimmune destruction of exocrine glands leading to debilitating dryness, remains one of the most underdiagnosed autoimmune conditions despite affecting millions worldwide. This systemic disorder primarily targets the salivary and lacrimal glands, causing severe dry mouth and dry eyes, but its effects extend far beyond these classic symptoms to include fatigue, joint pain, and potentially life-threatening organ involvement. The insidious onset and gradual progression of symptoms often lead to misdiagnosis as age-related changes, medication side effects, or other conditions such as fibromyalgia or chronic fatigue syndrome. Patients frequently endure years of dental problems, recurrent oral infections, and vision difficulties before receiving an accurate diagnosis, with studies showing an average diagnostic delay of nearly seven years. The condition predominantly affects women, particularly those over 40, leading to frequent misattribution of symptoms to menopause or hormonal changes. Sicca symptoms can result from numerous medications, environmental factors, or other medical conditions, creating diagnostic confusion and often leading to symptomatic treatment without recognition of the underlying autoimmune process. Extraglandular manifestations, occurring in up to 70% of patients, include arthritis, Raynaud's phenomenon, pulmonary involvement, kidney disease, and peripheral neuropathy, which may be misdiagnosed as separate conditions rather than recognized as part of a systemic autoimmune disorder. The development of lymphoma, particularly mucosa-associated lymphoid tissue (MALT) lymphoma, represents a serious complication that occurs in 5-10% of patients, emphasizing the importance of early diagnosis and monitoring. Diagnostic criteria require both objective evidence of glandular dysfunction and positive autoantibodies (anti-Ro/SSA, anti-La/SSB), yet these tests may not be routinely ordered in patients presenting with dry symptoms. Specialized tests such as salivary gland biopsy, Schirmer's test for tear production, and sialometry for saliva measurement are essential for definitive diagnosis but may not be readily available in all healthcare settings.
7. Inflammatory Bowel Disease - The Chronic Intestinal Battleground
Inflammatory bowel disease (IBD), encompassing both Crohn's disease and ulcerative colitis, represents a group of chronic autoimmune conditions that frequently face diagnostic delays due to symptom overlap with functional gastrointestinal disorders and other inflammatory conditions. These diseases involve chronic inflammation of the gastrointestinal tract, yet their presentations can be highly variable, leading to misdiagnosis as irritable bowel syndrome, infectious gastroenteritis, or other gastrointestinal conditions. Crohn's disease, which can affect any part of the digestive tract from mouth to anus, often presents with abdominal pain, diarrhea, and weight loss, but may also manifest with extraintestinal symptoms including arthritis, skin lesions, and eye inflammation that can overshadow gastrointestinal complaints. Ulcerative colitis, limited to the colon and rectum, typically presents with bloody diarrhea and urgency, but mild cases may be mistaken for hemorrhoids or infectious colitis. The intermittent nature of symptoms, with periods of remission alternating with active disease flares, can lead to delayed recognition and inappropriate reassurance that symptoms are not serious. Pediatric IBD presents unique diagnostic challenges, as symptoms may be subtle and include failure to thrive, delayed puberty, or isolated extraintestinal manifestations without obvious gastrointestinal symptoms. The overlap between IBD and other inflammatory conditions such as celiac disease, microscopic colitis, or infectious causes requires careful differentiation through appropriate testing including colonoscopy with biopsy, imaging studies, and laboratory markers. Indeterminate colitis, representing cases where features of both Crohn's disease and ulcerative colitis are present, poses additional diagnostic challenges and may require long-term follow-up for definitive classification. The consequences of delayed diagnosis include progression to complications such as strictures, fistulas, perforation, and increased colorectal cancer risk, while early diagnosis and treatment can prevent these serious outcomes and preserve intestinal function. Emerging biomarkers and advanced imaging techniques are improving diagnostic accuracy, but access to specialized gastroenterology care and endoscopic procedures remains a barrier in many healthcare systems.
8. Psoriatic Arthritis - The Hidden Joint Disease Behind Skin Symptoms

Psoriatic arthritis (PsA) represents a complex autoimmune condition that affects both skin and joints, yet it remains significantly underdiagnosed due to its variable presentations and the common misconception that psoriasis is merely a cosmetic skin condition. This inflammatory arthritis affects up to 30% of individuals with psoriasis, but the joint symptoms may precede, coincide with, or follow the development of skin lesions, creating diagnostic challenges when the typical temporal relationship is absent. The heterogeneous nature of PsA, with five distinct clinical patterns including symmetric polyarthritis, asymmetric oligoarthritis, distal interphalangeal joint involvement, arthritis mutilans, and axial disease, means that no single presentation is pathognomonic for the condition. Many patients are initially misdiagnosed with rheumatoid arthritis, osteoarthritis, or fibromyalgia, particularly when psoriatic skin lesions are minimal, hidden, or mistaken for other dermatologic conditions such as eczema or seborrheic dermatitis. The condition can affect the spine, peripheral joints, entheses (tendon and ligament insertion points), and cause dactylitis (sausage-like swelling of entire digits), yet these diverse manifestations may be attributed to separate conditions rather than recognized as part of a unified disease process. Nail involvement, occurring in up to 80% of PsA patients, includes pitting, onycholysis, and oil drop discoloration, but these changes are often overlooked or attributed to fungal infections or trauma. The absence of rheumatoid factor in most PsA patients can lead to diagnostic confusion, as healthcare providers may not consider inflammatory arthritis in seronegative cases. Enthesitis, inflammation at tendon and ligament insertion sites, is a hallmark feature of PsA but may be misdiagnosed as tendinitis, bursitis, or overuse injuries, particularly in physically active individuals. Early recognition is crucial as PsA can cause rapid joint destruction and functional disability, yet studies show diagnostic delays averaging 2-5 years from symptom onset. The development of classification criteria such as CASPAR (Classification criteria for Psoriatic Arthritis) has improved diagnostic accuracy, but these tools require familiarity with the diverse manifestations of the disease and may not be routinely applied in primary care settings.
9. Antiphospholipid Syndrome - The Clotting Disorder in Disguise
Antiphospholipid syndrome (APS) represents a unique autoimmune condition characterized by the production of antibodies against phospholipid-binding proteins, leading to increased thrombotic risk and pregnancy complications, yet it remains frequently undiagnosed due to its diverse clinical presentations and the need for specialized laboratory testing. This condition can manifest as recurrent venous or arterial thrombosis, pregnancy morbidity including recurrent miscarriages, or non-thrombotic manifestations such as thrombocytopenia, hemolytic anemia, and neurological symptoms. The protean nature of APS means that patients may present to various specialists including hematologists, obstetricians, neurologists, or cardiologists, each potentially focusing on isolated manifestations without recognizing the underlying autoimmune process. Primary APS occurs in isolation, while secondary APS develops in association with other autoimmune conditions, particularly systemic lupus erythematosus, creating additional diagnostic complexity when multiple conditions coexist. Catastrophic antiphospholipid syndrome (CAPS), a rare but life-threatening variant