10 Early Warning Signs of Type 2 Diabetes to Know
Type 2 diabetes has emerged as one of the most pressing health challenges of our time, affecting over 422 million people worldwide and earning its reputation as a "silent epidemic." Unlike Type 1 diabetes, which typically manifests dramatically in childhood or young adulthood, Type 2 diabetes often develops gradually over years, with subtle warning signs that can easily be dismissed or attributed to other factors such as aging, stress, or lifestyle changes. This insidious nature makes early detection crucial, as the condition can cause significant damage to blood vessels, nerves, and organs long before a formal diagnosis is made. The prediabetic phase, where blood sugar levels are elevated but not yet in the diabetic range, can last for years, presenting a critical window of opportunity for intervention. Understanding and recognizing the early warning signs of Type 2 diabetes can be the difference between preventing the disease entirely or managing its progression effectively. Research consistently shows that early intervention through lifestyle modifications can delay or even prevent the onset of Type 2 diabetes in up to 58% of high-risk individuals, making awareness of these warning signs not just beneficial but potentially life-saving.
1. Excessive Thirst and Frequent Urination

One of the most common and earliest warning signs of Type 2 diabetes is the development of excessive thirst (polydipsia) accompanied by frequent urination (polyuria), creating a frustrating cycle that many people initially attribute to drinking more fluids or aging. When blood glucose levels begin to rise above normal ranges, the kidneys work overtime to filter and remove the excess sugar from the bloodstream. However, when blood sugar levels exceed the kidney's ability to reabsorb glucose efficiently, the excess sugar spills into the urine, taking water with it through a process called osmotic diuresis. This leads to increased urine production, causing more frequent trips to the bathroom, particularly noticeable during nighttime hours. The body's natural response to this fluid loss is to trigger intense thirst as it attempts to replace the lost fluids and maintain proper hydration levels. Many individuals notice they're drinking significantly more water than usual yet still feeling thirsty, or they find themselves waking multiple times during the night to urinate. This symptom often develops gradually, making it easy to overlook initially, but it tends to become more pronounced as blood sugar levels continue to rise. Healthcare providers often use this classic symptom combination as one of the first indicators to investigate potential diabetes, as it reflects the body's struggle to maintain glucose homeostasis.
2. Unexplained Weight Loss Despite Normal Appetite

Paradoxical weight loss, where individuals lose weight despite maintaining or even increasing their food intake, represents another significant early warning sign of Type 2 diabetes that often confuses both patients and healthcare providers. This phenomenon occurs because the body's cells become increasingly resistant to insulin, the hormone responsible for allowing glucose to enter cells for energy production. When cells cannot effectively utilize glucose for fuel due to insulin resistance, the body begins to break down muscle tissue and fat stores to meet its energy requirements, leading to unintentional weight loss. This process, known as catabolism, can result in the loss of 10-20 pounds or more over several months, even when dietary habits remain unchanged or food consumption increases. The weight loss is particularly noticeable in individuals who have previously struggled with weight management or have been overweight, making the sudden drop even more concerning. Additionally, because the cells are essentially "starving" at the cellular level despite adequate food intake, many people experience persistent hunger and may actually increase their caloric consumption, yet continue to lose weight. This metabolic dysfunction creates a concerning cycle where the body cannot properly process nutrients, leading to muscle wasting and fatigue. Healthcare providers often investigate unexplained weight loss as a potential indicator of diabetes, especially when it occurs alongside other symptoms, as it suggests significant metabolic disruption that requires immediate attention and intervention.
3. Persistent Fatigue and Weakness

Chronic fatigue and weakness represent pervasive early symptoms of Type 2 diabetes that significantly impact quality of life and daily functioning, often developing so gradually that individuals adapt to feeling constantly tired without recognizing it as a medical concern. This overwhelming exhaustion stems from the body's inability to efficiently convert glucose into usable energy at the cellular level due to insulin resistance. When cells cannot properly absorb glucose from the bloodstream, they lack the primary fuel source needed for optimal function, leading to a persistent state of cellular energy deficit. Unlike normal tiredness that improves with rest, diabetes-related fatigue is characterized by a deep, bone-weary exhaustion that persists regardless of sleep quality or duration. Many individuals describe feeling as though they're "running on empty" throughout the day, struggling to complete routine tasks that were previously manageable. This fatigue often worsens after meals, particularly those high in carbohydrates, as blood sugar spikes further exacerbate the body's inability to process glucose effectively. The weakness component manifests as reduced physical strength, difficulty with previously easy activities like climbing stairs or carrying groceries, and a general sense of physical depletion. Additionally, the fluctuating blood sugar levels associated with developing diabetes can cause energy crashes and mood swings, creating a rollercoaster effect that leaves individuals feeling drained and emotionally exhausted. This symptom often prompts people to seek medical attention, as the persistent nature of the fatigue interferes with work performance, relationships, and overall life satisfaction.
4. Blurred Vision and Eye Problems

Visual disturbances, particularly blurred vision, serve as critical early warning signs of Type 2 diabetes that should never be ignored, as they indicate that elevated blood sugar levels are already beginning to affect delicate body systems. High glucose levels cause the lens of the eye to swell by drawing fluid into it, changing its shape and affecting its ability to focus properly. This results in blurred vision that may fluctuate throughout the day, often correlating with blood sugar levels – vision may be clearer in the morning after fasting overnight and become progressively blurrier after meals when blood glucose rises. Many individuals initially attribute these visual changes to eye strain from computer work, aging, or needing new glasses, delaying important medical evaluation. However, diabetes-related vision changes are distinctly different from typical refractive errors, as they tend to fluctuate rather than remain constant, and new prescription glasses often fail to provide lasting improvement. Beyond blurred vision, early diabetic eye problems may include difficulty focusing when switching between near and far objects, increased sensitivity to light, and seeing halos around lights, particularly at night. The retina, the light-sensitive tissue at the back of the eye, is particularly vulnerable to damage from high blood sugar levels, as elevated glucose can damage the tiny blood vessels that supply this crucial structure. Even in the early stages of diabetes, these microvascular changes can begin, making regular eye examinations essential for anyone experiencing unexplained vision changes. Prompt recognition and treatment of diabetes can often reverse these early visual symptoms, but delayed intervention may lead to permanent vision problems or even blindness.
5. Slow-Healing Wounds and Frequent Infections
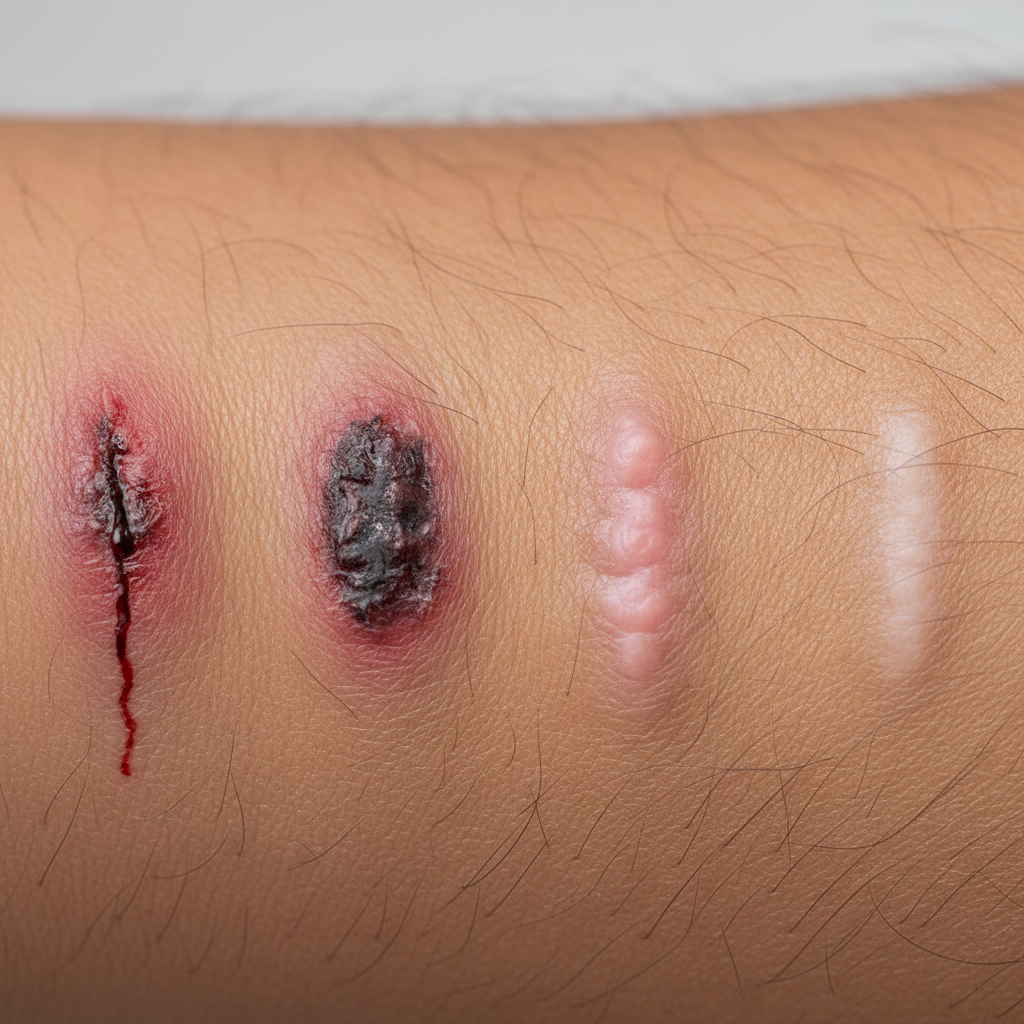
Impaired wound healing and increased susceptibility to infections represent significant early indicators of Type 2 diabetes that reflect the condition's impact on the immune system and circulatory function. Elevated blood glucose levels create an environment that promotes bacterial and fungal growth while simultaneously compromising the body's natural defense mechanisms. High sugar levels in the blood and tissues provide an ideal breeding ground for pathogens, while also impairing white blood cell function, reducing the body's ability to fight off infections effectively. Individuals may notice that minor cuts, scrapes, or bruises take significantly longer to heal than usual, sometimes remaining open or infected for weeks rather than the typical few days. This delayed healing occurs because high glucose levels damage blood vessels, reducing circulation and limiting the delivery of oxygen and nutrients essential for tissue repair. Common areas affected include the feet, legs, and gums, where even small injuries may become problematic. Frequent infections, particularly urinary tract infections, yeast infections, and skin infections, may occur with unusual frequency or severity. Women may experience recurrent vaginal yeast infections, while both men and women might notice persistent skin infections, especially in warm, moist areas like under the arms, between toes, or in skin folds. Gum disease and dental infections may also become more common and severe, as the mouth's bacterial balance shifts in response to elevated glucose levels in saliva. These symptoms often prompt individuals to seek medical attention, providing an opportunity for diabetes screening and early intervention before more serious complications develop.
6. Increased Hunger and Food Cravings

Persistent hunger and intense food cravings, particularly for carbohydrate-rich foods, represent a paradoxical early warning sign of Type 2 diabetes that occurs despite adequate or even excessive caloric intake. This phenomenon, known as polyphagia, develops because cells throughout the body are unable to effectively utilize glucose for energy due to insulin resistance, sending constant hunger signals to the brain despite normal or elevated blood sugar levels. The body essentially experiences starvation at the cellular level while glucose accumulates in the bloodstream, creating a frustrating cycle where eating provides only temporary satisfaction before hunger returns with renewed intensity. These cravings often focus specifically on sugary or starchy foods, as the body instinctively seeks quick sources of glucose in an attempt to satisfy its perceived energy deficit. However, consuming these foods only exacerbates the problem by further elevating blood sugar levels without addressing the underlying insulin resistance. Many individuals describe feeling as though they can never quite feel satisfied or full, regardless of how much they eat, leading to gradual weight gain in some cases or unexplained weight loss in others, depending on how their metabolism responds to the insulin resistance. The timing of these cravings often correlates with blood sugar fluctuations, becoming more intense during periods of relative hypoglycemia that occur as blood sugar levels drop from their elevated peaks. This symptom can be particularly distressing for individuals who have previously maintained good portion control or healthy eating habits, as they may feel they've lost control over their appetite. Understanding this symptom as a potential sign of diabetes rather than a lack of willpower can help individuals seek appropriate medical evaluation and treatment.
7. Tingling and Numbness in Extremities
Peripheral neuropathy, manifesting as tingling, numbness, or burning sensations in the hands and feet, represents one of the more concerning early warning signs of Type 2 diabetes as it indicates that elevated blood sugar levels are beginning to damage the nervous system. This condition, known as diabetic peripheral neuropathy, typically begins in the longest nerves first, which is why symptoms usually appear in the toes and feet before progressing to the hands and fingers in a characteristic "stocking and glove" distribution. The high glucose levels in the bloodstream damage nerve fibers through multiple mechanisms, including the formation of advanced glycation end products (AGEs) that accumulate in nerve tissue, reduced blood flow to nerves due to microvascular damage, and metabolic disruptions that affect nerve function. Early symptoms often include a tingling or "pins and needles" sensation, particularly noticeable at night or when resting, that many people initially attribute to poor circulation, sleeping in an awkward position, or wearing tight shoes. As the condition progresses, individuals may experience numbness that makes it difficult to feel temperature changes, pain, or pressure in affected areas, creating a dangerous situation where injuries may go unnoticed. Some people describe the sensation as feeling like they're wearing thick socks or gloves even when their skin is bare, while others experience sharp, shooting pains or a constant burning sensation. The feet are particularly vulnerable because they bear the body's weight and are furthest from the heart, making them more susceptible to circulation problems and nerve damage. Early recognition and treatment of diabetes can slow or even halt the progression of neuropathy, but delayed intervention may result in permanent nerve damage and increased risk of serious complications such as foot ulcers or infections.
8. Dark Skin Patches (Acanthosis Nigricans)

Acanthosis nigricans, characterized by dark, velvety patches of skin that typically appear in body folds and creases, serves as a visible early warning sign of insulin resistance and potential Type 2 diabetes development. These distinctive skin changes most commonly occur in areas where skin rubs against skin, such as the neck, armpits, groin, elbows, and knuckles, appearing as thick, darkened patches that may feel slightly raised or have a velvety texture. The condition develops as a direct result of elevated insulin levels in the bloodstream, which stimulate the growth of skin cells and increase melanin production, leading to the characteristic hyperpigmentation. While acanthosis nigricans can occur in individuals without diabetes, its presence, particularly in adults, strongly suggests underlying insulin resistance and significantly increases the risk of developing Type 2 diabetes. Many people initially mistake these patches for poor hygiene or assume they can be scrubbed away, but the discoloration persists despite thorough cleaning and may actually worsen with aggressive scrubbing. The patches typically develop gradually over months or years, often going unnoticed until they become quite pronounced. In some cases, the affected skin may also develop small, skin-colored growths called skin tags, which further indicate metabolic dysfunction. Healthcare providers often use the presence of acanthosis nigricans as a clinical marker to screen for diabetes and metabolic syndrome, particularly in overweight individuals or those with a family history of diabetes. The good news is that these skin changes can improve significantly with proper diabetes management and weight loss, as reducing insulin levels allows the skin to gradually return toward its normal appearance, making early recognition and intervention particularly valuable.
9. Recurring Skin and Gum Infections
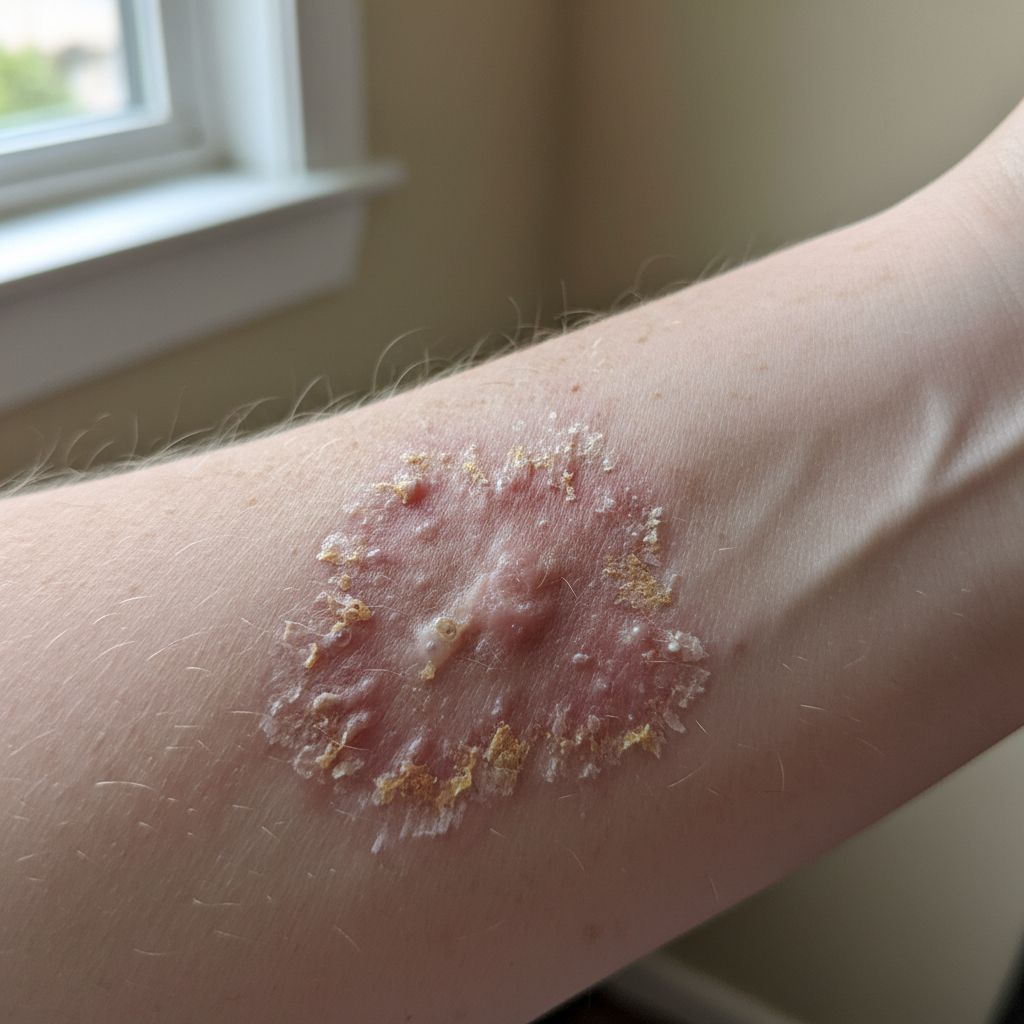
Frequent skin infections, dental problems, and gum disease represent important early indicators of Type 2 diabetes that reflect the condition's impact on immune function and tissue health. Elevated blood glucose levels create an environment that promotes bacterial and fungal growth while simultaneously weakening the body's natural defense mechanisms, making infections more likely to occur and more difficult to resolve. The skin, being the body's largest organ and first line of defense against pathogens, becomes particularly vulnerable when blood sugar levels are consistently elevated. Common skin infections include bacterial infections such as cellulitis, boils, and folliculitis, as well as fungal infections like athlete's foot, jock itch, and yeast infections in skin folds. These infections often occur in areas where moisture and warmth create ideal conditions for microbial growth, such as between toes, under breasts, in the groin area, or around the waistline where clothing creates friction. Dental and gum problems also become more prevalent and severe in individuals with developing diabetes, as elevated glucose levels in saliva provide nutrients for harmful bacteria in the mouth. Gingivitis and periodontitis may develop more rapidly and be more difficult to treat, with symptoms including bleeding gums, persistent bad breath, loose teeth, and recurrent dental abscesses. The relationship between diabetes and oral health is bidirectional, as severe gum disease can also worsen blood sugar control, creating a dangerous cycle. Many individuals notice that infections that would typically resolve quickly with basic treatment become persistent or recurrent, requiring multiple rounds of antibiotics or antifungal medications. This pattern of recurring infections often prompts healthcare providers to screen for diabetes, as it suggests underlying immune system compromise that may be related to metabolic dysfunction.
10. Mood Changes and Irritability

Significant mood changes, increased irritability, and emotional instability represent often-overlooked early warning signs of Type 2 diabetes that can profoundly impact relationships, work performance, and overall quality of life. The connection between blood sugar fluctuations and mood is well-established, as the brain relies heavily on glucose for optimal function, and any disruption in glucose availability or utilization can affect neurotransmitter production and neural activity. When blood sugar levels spike and crash throughout the day due to insulin resistance, individuals may experience corresponding emotional highs and lows that seem disproportionate to their circumstances. During periods of elevated blood glucose, people may feel anxious, restless, or agitated, while blood sugar drops can trigger irritability, mood swings, difficulty concentrating, and even symptoms resembling depression. Many individuals describe feeling "on edge" or having a shorter fuse than usual, finding themselves snapping at family members or colleagues over minor issues that wouldn't normally bother them. The cognitive effects of unstable blood sugar can include brain fog, difficulty making decisions, memory problems, and reduced ability to handle stress effectively. Sleep disturbances caused by frequent urination and blood sugar fluctuations can further exacerbate mood problems, creating a cycle where poor sleep worsens blood sugar control, which in turn affects mood and sleep quality. Family members and close friends often notice these personality changes before the individual does, observing increased moodiness, withdrawal from social activities, or uncharacteristic emotional responses. These psychological symptoms are frequently attributed to stress, aging, or life circumstances, delaying recognition of their potential connection to diabetes. Understanding the relationship between blood sugar and mood can help individuals seek appropriate medical evaluation and treatment, as stabilizing glucose levels often leads to significant improvements in emotional well-being and cognitive function.
11. Taking Action on Early Warning Signs

Recognizing the early warning signs of Type 2 diabetes represents a crucial step toward preventing or effectively managing this increasingly common condition that affects millions of people worldwide. The ten warning signs discussed – excessive thirst and urination, unexplained weight loss, persistent fatigue, blurred vision, slow-healing wounds, increased hunger, tingling in extremities, dark skin patches, recurring infections, and mood changes – often develop gradually and may be easily dismissed as normal aging or stress-related symptoms. However, their presence, particularly in combination, should prompt immediate medical evaluation and blood sugar testing. The importance of early detection cannot be overstated, as research consistently demonstrates that intervention during the prediabetic phase can prevent or significantly delay the onset of Type 2 diabetes through lifestyle modifications including dietary changes, regular physical activity, weight management, and stress reduction. Even when diabetes has already developed, early diagnosis and treatment can prevent or minimize serious complications such as heart disease, stroke, kidney damage, nerve damage, and vision loss. Healthcare providers can perform simple blood tests, including fasting glucose, hemoglobin A1C, or oral glucose tolerance tests, to accurately diagnose diabetes or prediabetes. For individuals at higher risk due to family history, obesity, sedentary lifestyle, or other risk factors, regular screening becomes even more critical. The key message is that Type 2 diabetes is largely preventable and highly manageable when detected early, but the window of opportunity for optimal intervention