10 Cancer Screening Timelines by Type That Catch Problems Early
Early cancer detection represents one of the most powerful weapons in modern medicine's arsenal against this devastating disease. When cancer is caught in its earliest stages, before it has spread to other parts of the body, treatment options are typically more effective, less invasive, and associated with significantly better survival rates. The difference between Stage I and Stage IV cancer can literally mean the difference between life and death, with five-year survival rates often dropping from over 90% to less than 30% as the disease progresses. This stark reality underscores why understanding and adhering to recommended cancer screening timelines is absolutely crucial for everyone. Different types of cancer require different screening approaches, frequencies, and starting ages based on extensive research into how these diseases develop and spread. From the well-established mammography guidelines for breast cancer to the newer recommendations for lung cancer screening in high-risk populations, each screening protocol has been carefully developed through decades of clinical trials and population studies. The following comprehensive guide explores ten of the most important cancer screening timelines, providing you with the knowledge needed to take proactive steps in protecting your health and potentially catching cancer at its most treatable stage.
1. Breast Cancer Screening - Mammography and Beyond

Breast cancer screening represents one of the most well-established and successful cancer prevention programs in modern medicine, with mammography serving as the cornerstone of early detection efforts. The American Cancer Society recommends that women with average risk begin annual mammograms at age 45, with the option to start at age 40 if they choose, and transition to biennial screening at age 55 or continue annually based on personal preference and life expectancy. However, these guidelines become more complex for women with elevated risk factors, including those with BRCA1 or BRCA2 genetic mutations, strong family histories, or previous chest radiation therapy. High-risk women may need to begin screening as early as age 25-30 with magnetic resonance imaging (MRI) in addition to mammography, creating a more intensive surveillance protocol. The evolution of breast cancer screening has also incorporated newer technologies such as 3D mammography (tomosynthesis), which can detect 20-65% more invasive cancers than traditional 2D mammography, particularly in women with dense breast tissue. Clinical breast examinations, while no longer recommended as standalone screening tools, remain valuable components of routine healthcare visits. The screening timeline must also account for the fact that breast cancer risk increases significantly with age, with the median age at diagnosis being 62 years, making consistent screening throughout a woman's lifetime essential for optimal outcomes.
2. Cervical Cancer Screening - Pap Smears and HPV Testing

Cervical cancer screening has undergone revolutionary changes over the past several decades, evolving from annual Pap smears for all women to a more nuanced, risk-based approach that incorporates both cytology and human papillomavirus (HPV) testing. Current guidelines recommend that cervical cancer screening begin at age 21, regardless of sexual activity onset, with Pap tests every three years for women aged 21-29. For women aged 30-65, the preferred approach is co-testing with both Pap smears and HPV testing every five years, though Pap testing alone every three years remains acceptable. This extended interval is possible because cervical cancer typically develops slowly over many years, and the combination of tests provides excellent sensitivity for detecting precancerous changes. The integration of HPV testing has been particularly significant because persistent infection with high-risk HPV types is responsible for virtually all cervical cancers, making HPV status a crucial predictor of cancer risk. Women who have received the HPV vaccine still require regular screening, as the vaccines don't protect against all cancer-causing HPV types. The screening timeline also includes important stopping points: women over 65 who have had adequate prior screening with normal results can discontinue screening, and women who have had hysterectomies with removal of the cervix for non-cancerous reasons typically don't need continued cervical cancer screening. This sophisticated approach has contributed to a dramatic decline in cervical cancer incidence and mortality in countries with organized screening programs.
3. Colorectal Cancer Screening - Multiple Effective Options
Colorectal cancer screening offers perhaps the most diverse array of effective screening options, each with distinct timelines and protocols designed to detect both cancer and precancerous polyps before they become malignant. The standard recommendation calls for screening to begin at age 45 for average-risk individuals, recently lowered from age 50 due to increasing incidence in younger populations. Colonoscopy, considered the gold standard, is typically performed every 10 years and allows for both detection and removal of polyps during the same procedure. However, several other effective options exist, including flexible sigmoidoscopy every five years, CT colonography (virtual colonoscopy) every five years, and various stool-based tests with different frequencies. The fecal immunochemical test (FIT) requires annual testing, while the multi-target stool DNA test (Cologuard) is performed every three years. High-risk individuals, including those with inflammatory bowel disease, strong family histories, or genetic syndromes like Lynch syndrome, may need to begin screening as early as age 20-25 and require more frequent surveillance. The screening timeline extends until age 75 for most individuals, with decisions about continued screening between ages 76-85 based on individual health status, life expectancy, and prior screening history. The effectiveness of colorectal cancer screening is particularly notable because it can actually prevent cancer by detecting and removing precancerous polyps, making adherence to recommended timelines crucial for optimal protection.
4. Lung Cancer Screening - Targeting High-Risk Smokers
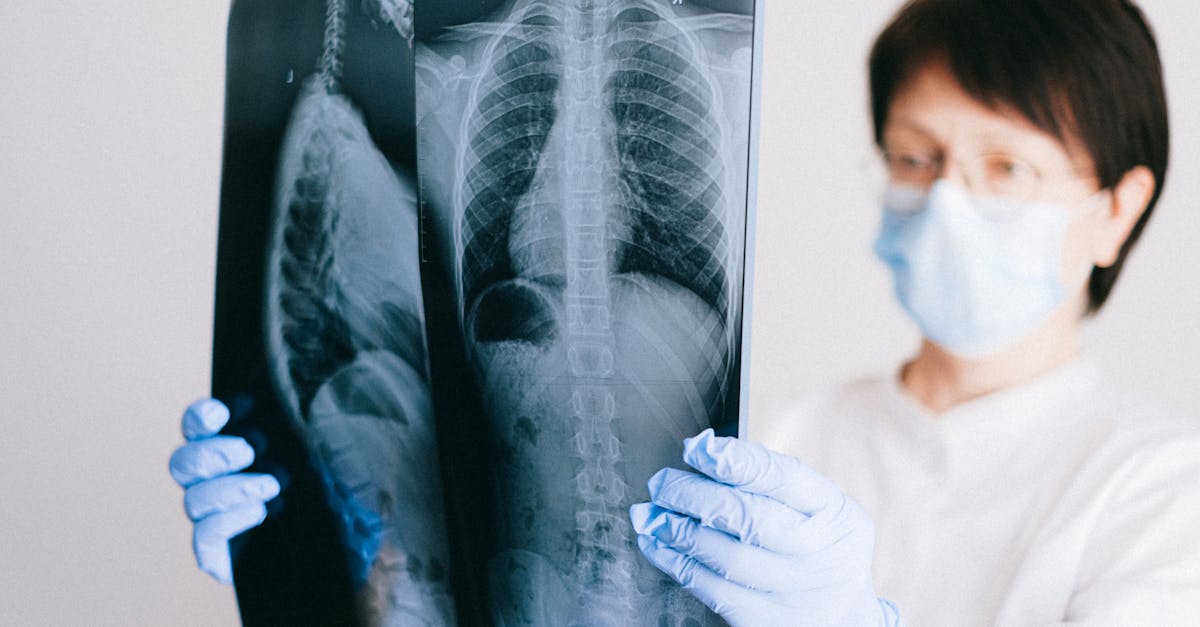
Lung cancer screening represents one of the newest additions to routine cancer screening recommendations, specifically targeting individuals at highest risk due to significant smoking histories. The current guidelines recommend annual low-dose computed tomography (LDCT) screening for adults aged 50-80 who have a 20 pack-year smoking history and currently smoke or have quit within the past 15 years. A pack-year is calculated by multiplying the number of packs smoked per day by the number of years smoked, so someone who smoked one pack per day for 20 years or two packs per day for 10 years would have a 20 pack-year history. This targeted approach is necessary because lung cancer screening involves radiation exposure and has a relatively high rate of false-positive results, making it inappropriate for low-risk populations. The screening timeline requires annual LDCT scans as long as the individual remains in good health and is a candidate for curative treatment, with screening typically discontinued when a person has not smoked for 15 years or develops health problems that substantially limit life expectancy. The implementation of lung cancer screening programs has shown promising results, with the National Lung Screening Trial demonstrating a 20% reduction in lung cancer mortality among high-risk individuals. However, the success of lung cancer screening depends heavily on proper patient selection, high-quality imaging, and comprehensive follow-up protocols for managing the inevitable false-positive results that occur in this population.
5. Prostate Cancer Screening - Navigating Controversy and Individual Choice
Prostate cancer screening remains one of the most controversial topics in cancer prevention, with guidelines emphasizing shared decision-making between patients and healthcare providers rather than universal recommendations. The current approach suggests that men aged 55-69 should engage in informed discussions with their doctors about the potential benefits and harms of prostate-specific antigen (PSA) testing, with screening decisions based on individual values and preferences. For men at higher risk, including African American men and those with strong family histories, these discussions may begin at age 40-45. The controversy surrounding prostate cancer screening stems from the fact that many prostate cancers grow slowly and may never cause symptoms or threaten life, leading to concerns about overdiagnosis and overtreatment. However, PSA screening can also detect aggressive cancers early when they are most treatable, creating a complex risk-benefit calculation. The screening timeline typically involves annual PSA testing for men who choose to be screened, though some experts suggest that men with very low PSA levels might extend the interval to every two years. Digital rectal examinations, once a standard component of prostate cancer screening, are now considered optional and of uncertain benefit. The decision about when to stop prostate cancer screening depends on age, overall health, and life expectancy, with most guidelines suggesting that men with less than 10-15 years of life expectancy are unlikely to benefit from continued screening.
6. Skin Cancer Screening - Self-Examination and Professional Assessment
Skin cancer screening encompasses both regular self-examinations and periodic professional skin assessments, with timelines varying based on individual risk factors and the type of skin cancer being targeted. For the general population, monthly self-examinations using the ABCDE criteria (Asymmetry, Border irregularity, Color variation, Diameter greater than 6mm, and Evolving characteristics) can help identify suspicious moles or lesions that warrant professional evaluation. Annual skin examinations by dermatologists or trained healthcare providers are recommended for individuals at high risk, including those with personal or family histories of melanoma, numerous atypical moles, fair skin that burns easily, or significant sun exposure. However, there is no universal consensus on routine skin cancer screening for average-risk individuals, as evidence for population-wide screening programs remains limited. High-risk individuals may require more frequent professional examinations, sometimes every 3-6 months, particularly those with dysplastic nevus syndrome or genetic predispositions to melanoma. The screening timeline for skin cancer is unique because it can begin at any age, as melanoma, though rare in children, can occur in young adults, and the incidence increases with age. Total body photography and dermoscopy (dermatoscopy) are increasingly used in high-risk patients to document and monitor moles over time, allowing for more precise detection of changes that might indicate malignant transformation. The effectiveness of skin cancer screening depends heavily on both patient education for self-examination and access to experienced dermatologists who can distinguish between benign and potentially malignant lesions.
7. Ovarian Cancer Screening - Limited Options and High-Risk Focus
Ovarian cancer screening presents unique challenges because effective screening methods for the general population remain elusive, leading to focused efforts on high-risk women who may benefit from intensive surveillance protocols. Unlike many other cancers, there are currently no recommended routine screening tests for ovarian cancer in average-risk women, as neither CA-125 blood tests nor transvaginal ultrasounds have proven effective at reducing mortality in this population. The primary screening timeline focuses on women at high risk due to BRCA1 or BRCA2 mutations, Lynch syndrome, or strong family histories of ovarian or breast cancer. For these high-risk women, screening typically begins between ages 30-35 and may include transvaginal ultrasounds and CA-125 measurements every 6-12 months, though the effectiveness of this approach remains uncertain. Many high-risk women ultimately choose prophylactic bilateral salpingo-oophorectomy (removal of ovaries and fallopian tubes) after completing childbearing, typically recommended between ages 35-40 for BRCA1 carriers and 40-45 for BRCA2 carriers. Recent research has shifted focus toward the fallopian tubes as the likely origin of many "ovarian" cancers, leading to investigations of salpingectomy (removal of fallopian tubes while preserving ovaries) as a risk-reduction strategy. The lack of effective screening options underscores the importance of recognizing symptoms such as bloating, pelvic pain, difficulty eating, and urinary urgency, particularly when they are persistent and represent a change from normal. Genetic counseling and testing play crucial roles in identifying high-risk women who might benefit from enhanced surveillance or prophylactic surgery.
8. Liver Cancer Screening - Targeting Chronic Disease Populations
Liver cancer screening focuses primarily on individuals with chronic liver disease, particularly those with cirrhosis, as this population faces dramatically elevated cancer risk compared to the general population. The recommended screening timeline involves ultrasound examinations every six months for patients with cirrhosis, regardless of the underlying cause, whether it be hepatitis B or C infection, alcohol-related liver disease, or non-alcoholic fatty liver disease. Alpha-fetoprotein (AFP) blood testing may be used in conjunction with ultrasound, though its value remains controversial due to limited sensitivity and specificity. For patients with chronic hepatitis B infection without cirrhosis, screening recommendations vary based on additional risk factors such as family history, age, gender, and viral load, with some guidelines suggesting screening for Asian men over 40, Asian women over 50, and African individuals over 20. The screening timeline for hepatitis C patients typically begins once cirrhosis is established, as the cancer risk in non-cirrhotic hepatitis C patients is relatively low. However, successful treatment of hepatitis C with direct-acting antivirals may reduce but not eliminate cancer risk, so continued surveillance is often recommended even after viral cure. The effectiveness of liver cancer screening depends heavily on the quality of ultrasound examination and the experience of the interpreting radiologist, as early liver cancers can be difficult to detect. Patients with detected lesions often require additional imaging with CT or MRI for further characterization, and the rapid growth potential of liver cancer makes adherence to the six-month screening interval crucial for optimal outcomes.
9. Stomach Cancer Screening - Geographic and Risk-Based Variations

Stomach cancer screening practices vary dramatically worldwide, with organized screening programs primarily implemented in countries with high gastric cancer incidence, such as Japan and South Korea, while most Western countries focus on targeted screening for high-risk individuals. In high-incidence countries, population-based screening typically begins at age 40-50 using upper endoscopy or upper gastrointestinal series, performed every 1-2 years depending on the specific protocol and individual risk factors. The screening timeline in these countries has proven effective, with significant reductions in gastric cancer mortality attributed to early detection programs. In lower-incidence countries like the United States, screening recommendations focus on individuals with specific risk factors, including those with hereditary diffuse gastric cancer syndrome, pernicious anemia, gastric adenomatous polyps, or chronic atrophic gastritis. Helicobacter pylori infection, a major risk factor for gastric cancer, has led to screening and treatment programs in some populations, though the optimal timing and target populations remain subjects of ongoing research. Family history plays a crucial role in determining screening timelines, with individuals having first-degree relatives with gastric cancer potentially benefiting from earlier and more frequent screening. The emergence of genetic testing for CDH1 mutations associated with hereditary diffuse gastric cancer has created new screening paradigms, often involving annual endoscopy beginning in the twenties or thirties, and many affected individuals ultimately choose prophylactic total gastrectomy. The effectiveness of gastric cancer screening depends heavily on the expertise of endoscopists and the use of advanced techniques such as chromoendoscopy or narrow-band imaging to detect subtle mucosal abnormalities.
10. Pancreatic Cancer Screening - Emerging Protocols for Ultra-High-Risk Groups

Pancreatic cancer screening remains largely experimental and is currently recommended only for individuals at extremely high risk, as effective screening methods for the general population do not exist and the disease's aggressive nature makes early detection challenging. The screening timeline for high-risk individuals typically begins around age 50 or 10 years younger than the youngest affected family member, whichever comes first, and involves annual imaging with magnetic resonance imaging (MRI) or endoscopic ultrasound (EUS). Candidates for pancreatic cancer screening include individuals with hereditary pancreatitis, Peutz-Jeghers syndrome, familial atypical multiple mole melanoma (FAMMM) syndrome, or strong family histories suggesting hereditary pancreatic cancer. Genetic testing for mutations in genes such as BRCA1, BRCA2, PALB2, ATM, and others associated with increased pancreatic cancer risk helps identify appropriate screening candidates. The screening protocol often involves alternating MRI and EUS every six months to maximize detection sensitivity, as each modality has distinct advantages in visualizing different aspects of pancreatic anatomy and pathology. Research into blood-based biomarkers and advanced imaging techniques continues to evolve, with promising developments in areas such as circulating tumor DNA and artificial intelligence-enhanced image analysis. The psychological impact of pancreatic cancer screening cannot be understated, as participants face the knowledge that they carry significantly elevated risk for a disease with poor prognosis, making counseling and support services integral components of screening programs. Most screening programs are conducted within research protocols at specialized centers, reflecting the experimental nature of current approaches and the need for continued investigation into optimal screening strategies.
11. Integrating Screening Timelines into Comprehensive Healthcare

The landscape of cancer screening represents a complex interplay of scientific evidence, individual risk factors, and healthcare resources, requiring personalized approaches that balance the benefits of early detection against the potential harms of overdiagnosis and unnecessary procedures. Understanding the diverse screening timelines for different cancer types empowers individuals to work collaboratively with their healthcare providers in developing comprehensive prevention strategies tailored to their unique circumstances. The evolution of screening guidelines reflects our growing understanding of cancer biology, with newer approaches increasingly incorporating genetic risk factors, family history, and individual preferences into screening decisions. Technology continues to advance screening capabilities, from improved imaging techniques that can detect smaller lesions to blood-based tests that may revolutionize early detection across multiple cancer types. However, the success of any screening program ultimately depends on consistent participation and adherence to recommended timelines, making patient education and healthcare system support crucial components of effective cancer prevention. As we look toward the future, emerging technologies such as artificial intelligence, liquid biopsies, and multi-cancer early detection tests promise to further refine our ability to catch cancers at their most treatable stages. The integration of these various screening timelines into routine healthcare requires coordination between primary care providers, specialists, and patients, emphasizing the importance of maintaining detailed health records and open communication about risk factors and screening preferences. Ultimately, the goal of cancer screening is not just to detect disease early, but to prevent cancer-related suffering and death while minimizing the burden of screening itself, making informed participation in age-appropriate screening programs one of the most important health decisions individuals can make.