12 Daily Habits Linked to Lower Cardiovascular Risk
Cardiovascular disease remains the leading cause of death globally, claiming approximately 17.9 million lives annually according to the World Health Organization. However, emerging research consistently demonstrates that simple, daily lifestyle modifications can dramatically reduce cardiovascular risk by up to 80%. The concept of preventive cardiology has evolved beyond traditional medical interventions to embrace a holistic approach that emphasizes sustainable daily habits. These evidence-based practices work synergistically to improve endothelial function, reduce systemic inflammation, optimize lipid profiles, and enhance overall cardiovascular resilience. From the moment we wake up to our evening routines, each choice we make either contributes to or detracts from our heart health. This comprehensive exploration examines twelve scientifically-validated daily habits that have been consistently linked to lower cardiovascular risk, providing practical strategies that can be seamlessly integrated into modern lifestyles. Understanding these habits and their underlying mechanisms empowers individuals to take proactive control of their cardiovascular destiny, transforming everyday activities into powerful tools for heart disease prevention.
1. Morning Hydration - Kickstarting Cardiovascular Function

The simple act of consuming adequate water upon waking serves as a fundamental catalyst for optimal cardiovascular function throughout the day. Research published in the American Journal of Epidemiology reveals that individuals who drink five or more glasses of water daily have a 41% lower risk of fatal coronary heart disease compared to those consuming two glasses or less. Morning hydration specifically addresses the natural dehydration that occurs during sleep, when the body continues metabolic processes without fluid intake for 6-8 hours. This dehydration state increases blood viscosity, forcing the heart to work harder to pump thicker blood through the circulatory system. By consuming 16-20 ounces of water within the first hour of waking, individuals can rapidly restore optimal blood viscosity, reduce cardiac workload, and improve oxygen delivery to tissues. Additionally, proper hydration supports healthy blood pressure regulation by maintaining adequate plasma volume and supporting kidney function in sodium excretion. The temperature of morning water intake also matters; room temperature or slightly warm water is absorbed more efficiently than ice-cold water, which can temporarily constrict blood vessels. Establishing this simple morning ritual creates a foundation for sustained cardiovascular health while supporting the body's natural circadian rhythms and metabolic processes.
2. Regular Physical Activity - The Ultimate Cardiovascular Medicine
Daily physical activity stands as perhaps the most potent non-pharmacological intervention for cardiovascular disease prevention, with effects comparable to many prescription medications. The landmark Framingham Heart Study, spanning over seven decades, consistently demonstrates that individuals engaging in regular moderate exercise reduce their cardiovascular disease risk by 30-35%. The mechanisms underlying these protective effects are multifaceted and profound. Exercise stimulates the production of nitric oxide, a powerful vasodilator that improves endothelial function and reduces arterial stiffness. Regular physical activity also promotes the development of collateral circulation, creating alternative pathways for blood flow that can compensate for potential arterial blockages. Furthermore, exercise enhances insulin sensitivity, reduces systemic inflammation markers like C-reactive protein, and optimizes lipid profiles by increasing HDL cholesterol while reducing triglycerides and small, dense LDL particles. The beauty of this habit lies in its accessibility; even 150 minutes of moderate-intensity activity per week, as recommended by the American Heart Association, can be achieved through brisk walking, gardening, dancing, or household activities. High-intensity interval training (HIIT) has emerged as particularly effective, with studies showing that just 15 minutes of HIIT three times per week can produce cardiovascular benefits equivalent to 45 minutes of moderate continuous exercise. The key is consistency rather than intensity, making daily movement a non-negotiable component of cardiovascular health maintenance.
3. Mindful Eating Practices - Nourishing the Heart Through Conscious Consumption

The practice of mindful eating extends far beyond simple dietary choices, encompassing how, when, and why we consume food, with profound implications for cardiovascular health. Research from Harvard Medical School indicates that individuals who eat slowly and mindfully have a 23% lower risk of developing metabolic syndrome, a cluster of conditions that significantly increase cardiovascular disease risk. Mindful eating practices activate the parasympathetic nervous system, promoting optimal digestion and nutrient absorption while reducing stress-induced cortisol production that can contribute to inflammation and arterial damage. This approach naturally leads to better portion control, as it takes approximately 20 minutes for satiety signals to reach the brain, allowing mindful eaters to recognize fullness before overconsumption occurs. The practice also enhances appreciation for nutrient-dense foods, naturally steering individuals toward heart-healthy options rich in omega-3 fatty acids, antioxidants, and fiber. Studies show that mindful eaters consume 300-400 fewer calories daily without feeling deprived, leading to sustainable weight management that reduces cardiovascular strain. Additionally, mindful eating practices help identify emotional eating triggers, breaking the cycle of stress-induced food consumption that often involves processed, high-sodium, and high-sugar foods detrimental to heart health. By creating sacred space around meals, eliminating distractions like television or smartphones, and focusing on the sensory experience of eating, individuals can transform each meal into an opportunity for cardiovascular nourishment and stress reduction.
4. Stress Management Through Deep Breathing - Calming the Cardiovascular Storm

Chronic stress acts as a silent assassin of cardiovascular health, triggering a cascade of physiological responses that directly damage the heart and blood vessels over time. The implementation of daily deep breathing exercises serves as a powerful antidote to stress-induced cardiovascular damage, with research from the Journal of Hypertension showing that regular breathing exercises can reduce systolic blood pressure by 10-15 mmHg. The physiological mechanism involves activation of the parasympathetic nervous system through stimulation of the vagus nerve, which counteracts the fight-or-flight response that chronically elevates heart rate, blood pressure, and stress hormone production. Deep breathing exercises, particularly the 4-7-8 technique (inhaling for 4 counts, holding for 7, exhaling for 8), have been shown to reduce cortisol levels by up to 25% within just 10 minutes of practice. This reduction in stress hormones directly translates to decreased inflammation, improved endothelial function, and reduced risk of arterial plaque formation. The beauty of this habit lies in its immediate accessibility and effectiveness; it requires no equipment, can be performed anywhere, and produces measurable physiological changes within minutes. Studies from the Mayo Clinic demonstrate that individuals who practice deep breathing exercises for just 5 minutes twice daily show improved heart rate variability, a key marker of cardiovascular resilience and autonomic nervous system balance. Regular practitioners also report improved sleep quality, reduced anxiety, and enhanced emotional regulation, creating a positive feedback loop that further supports cardiovascular health through multiple pathways.
5. Quality Sleep Patterns - Repairing and Protecting the Cardiovascular System

Sleep serves as the body's natural cardiovascular repair and maintenance period, making quality sleep patterns essential for heart health and disease prevention. The landmark Nurses' Health Study, following over 71,000 women for 10 years, revealed that individuals sleeping less than 5 hours per night had a 39% higher risk of coronary heart disease compared to those sleeping 8 hours. During deep sleep stages, blood pressure naturally decreases by 10-20%, giving the cardiovascular system crucial recovery time from daily stresses. This "nocturnal dipping" allows arterial walls to repair microscopic damage, reduces inflammation, and helps regulate hormones that control blood pressure and glucose metabolism. Sleep deprivation disrupts this restorative process while simultaneously increasing production of stress hormones like cortisol and inflammatory markers such as interleukin-6 and tumor necrosis factor-alpha. Poor sleep quality also affects appetite-regulating hormones ghrelin and leptin, leading to increased hunger and cravings for high-calorie, processed foods that contribute to cardiovascular risk. The relationship between sleep and cardiovascular health is bidirectional; sleep disorders like sleep apnea directly strain the heart through repeated episodes of oxygen deprivation and blood pressure spikes. Establishing consistent sleep hygiene practices, including maintaining regular bedtimes, creating a cool and dark sleep environment, and avoiding screens before bed, can significantly improve both sleep quality and cardiovascular outcomes. Research shows that improving sleep quality can reduce cardiovascular disease risk by 22% while also enhancing immune function, cognitive performance, and emotional well-being.
6. Social Connection and Community Engagement - The Heart's Need for Human Bonds

The profound impact of social connections on cardiovascular health represents one of the most compelling areas of modern medical research, with studies consistently showing that strong social bonds can reduce cardiovascular disease risk by 50%. The landmark Framingham Heart Study revealed that loneliness and social isolation create physiological stress responses equivalent to smoking 15 cigarettes daily, triggering chronic inflammation and elevating blood pressure through persistent activation of the sympathetic nervous system. Conversely, individuals with robust social networks demonstrate lower levels of inflammatory markers like C-reactive protein and interleukin-6, reduced cortisol production, and improved heart rate variability. The mechanisms underlying these protective effects are multifaceted, involving both direct physiological benefits and indirect behavioral influences. Social connections provide emotional support that buffers against stress, encourages healthy lifestyle choices, and creates accountability for maintaining beneficial habits like regular exercise and medical compliance. Research from Harvard Medical School shows that married individuals have a 5% lower risk of cardiovascular disease, while those with strong friendships show even greater protective effects. The quality of relationships matters more than quantity; toxic or stressful relationships can actually increase cardiovascular risk through chronic stress activation. Daily practices that strengthen social bonds, such as regular check-ins with friends, participating in community activities, volunteering, or simply sharing meals with others, create powerful protective effects against heart disease. Even brief positive social interactions, like expressing gratitude or offering help to others, trigger the release of oxytocin and other hormones that promote cardiovascular health and emotional well-being.
7. Omega-3 Rich Food Consumption - Essential Fatty Acids for Cardiovascular Protection

The daily consumption of omega-3 fatty acids represents one of the most scientifically validated nutritional interventions for cardiovascular disease prevention, with over 40,000 published studies documenting their protective effects. These essential fatty acids, particularly EPA (eicosapentaenoic acid) and DHA (docosahexaenoic acid), cannot be produced by the human body and must be obtained through diet or supplementation. Research from the American Heart Association shows that individuals consuming omega-3 rich foods daily reduce their risk of sudden cardiac death by 36% and overall cardiovascular mortality by 17%. The cardioprotective mechanisms of omega-3 fatty acids are remarkably diverse and powerful. They reduce triglyceride levels by 15-30%, decrease blood pressure by 2-5 mmHg, improve endothelial function, and possess potent anti-inflammatory properties that help prevent arterial plaque formation and rupture. Omega-3s also enhance heart rate variability, reduce arrhythmia risk, and improve the stability of existing arterial plaques, making them less likely to rupture and cause heart attacks or strokes. The most effective sources include fatty fish like salmon, mackerel, sardines, and anchovies, which should be consumed at least twice weekly. Plant-based sources such as flaxseeds, chia seeds, walnuts, and algae-derived supplements provide alpha-linolenic acid (ALA), though conversion to EPA and DHA is limited. The optimal daily intake ranges from 1-3 grams of combined EPA and DHA, achievable through a 3.5-ounce serving of fatty fish or high-quality supplements. Regular omega-3 consumption also supports brain health, reduces depression risk, and enhances cognitive function, creating synergistic benefits that further support cardiovascular wellness through improved stress management and lifestyle choices.
8. Limiting Processed Food Intake - Protecting Against Industrial Cardiovascular Toxins

The systematic reduction of processed food consumption represents a critical daily habit for cardiovascular protection, as these industrial food products contain numerous compounds that directly damage the cardiovascular system. Ultra-processed foods, which comprise over 60% of the average American diet, are engineered for palatability and shelf-life rather than nutritional value, containing excessive sodium, refined sugars, trans fats, and chemical additives that promote inflammation and arterial damage. Research published in the BMJ following over 105,000 adults for five years found that each 10% increase in ultra-processed food consumption was associated with a 12% higher risk of cardiovascular disease. The mechanisms of cardiovascular damage from processed foods are multifaceted and insidious. Excessive sodium intake, averaging 3,400mg daily in processed food consumers versus the recommended 2,300mg, leads to fluid retention, increased blood volume, and elevated blood pressure that strains arterial walls over time. Refined sugars and high-fructose corn syrup trigger insulin resistance, promote glycation of proteins in arterial walls, and increase production of advanced glycation end products (AGEs) that accelerate atherosclerosis. Trans fats, still present in many processed foods despite regulations, directly increase LDL cholesterol while decreasing protective HDL cholesterol. Chemical preservatives, artificial colors, and flavor enhancers have been linked to endothelial dysfunction and increased oxidative stress. The solution involves gradually replacing processed foods with whole, minimally processed alternatives, focusing on foods with fewer than five recognizable ingredients. This transition naturally increases consumption of protective nutrients like fiber, antioxidants, and phytonutrients while eliminating harmful additives, creating a powerful shift toward cardiovascular health that extends beyond simple calorie reduction.
9. Regular Blood Pressure Monitoring - Early Detection and Prevention
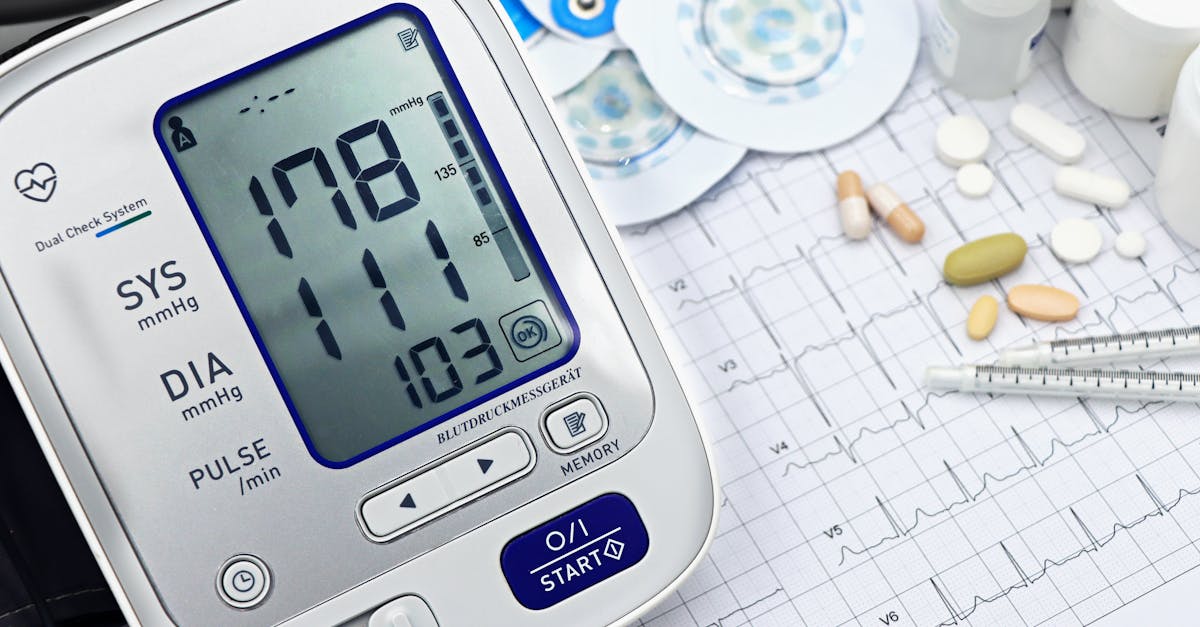
The establishment of regular blood pressure monitoring as a daily habit empowers individuals to detect cardiovascular changes before they progress to dangerous levels, enabling early intervention that can prevent heart attacks, strokes, and other cardiovascular events. Hypertension, affecting nearly half of American adults, is often called the "silent killer" because it typically produces no symptoms while steadily damaging arteries, the heart, brain, and kidneys. Home blood pressure monitoring has been shown to improve blood pressure control by 2.5-4.5 mmHg compared to clinic-only monitoring, a reduction that translates to a 10-15% decrease in cardiovascular event risk. The physiological understanding of blood pressure patterns throughout the day reveals important insights for cardiovascular health. Blood pressure naturally fluctuates based on circadian rhythms, physical activity, stress levels, and dietary factors, with morning readings typically being highest due to cortisol release and increased sympathetic nervous system activity. Regular monitoring helps identify these patterns and detect concerning trends like morning hypertension, which is associated with increased stroke risk, or lack of nocturnal dipping, which indicates poor cardiovascular recovery. Modern home monitors provide accurate readings when used correctly, and many feature smartphone connectivity for easy tracking and sharing with healthcare providers. The optimal monitoring schedule involves taking readings at the same times daily, preferably morning and evening, after sitting quietly for five minutes. This data becomes invaluable for healthcare providers in making treatment decisions and helps individuals understand how lifestyle factors like diet, exercise, stress, and sleep affect their cardiovascular health. Regular monitoring also increases awareness and motivation for maintaining healthy lifestyle habits, creating a positive feedback loop that reinforces cardiovascular protective behaviors.
10. Moderate Alcohol Consumption or Abstinence - Navigating the Cardiovascular Paradox

The relationship between alcohol consumption and cardiovascular health represents one of the most complex and controversial areas in preventive cardiology, requiring careful consideration of individual risk factors and consumption patterns. The famous "French Paradox" observed that moderate wine consumption appeared to protect against cardiovascular disease despite high saturated fat intake, leading to decades of research into alcohol's cardiovascular effects. Current evidence suggests that light to moderate alcohol consumption (defined as up to one drink daily for women and two for men) may provide modest cardiovascular benefits through several mechanisms: increasing HDL cholesterol, improving insulin sensitivity, reducing inflammation, and providing antioxidants, particularly from red wine's resveratrol content. However, these potential benefits must be weighed against significant risks, including increased blood pressure, elevated triglycerides, enhanced risk of atrial fibrillation, and the potential for alcohol dependency. Recent large-scale studies, including analysis of over 600,000 individuals published in The Lancet, suggest that any cardiovascular benefits of alcohol are outweighed by increased risks of cancer, liver disease, and accidents, particularly at higher consumption levels. The cardioprotective effects previously attributed to alcohol may actually result from other lifestyle factors common among moderate drinkers, such as higher socioeconomic status, better healthcare access, and healthier overall lifestyle patterns. For individuals who choose to consume alcohol, the key principles include strict moderation, avoiding binge drinking patterns, choosing quality over quantity, and never drinking and driving. For those who don't currently drink, the evidence does not support starting alcohol consumption for cardiovascular benefits, as the same protective effects can be achieved through other lifestyle modifications without the associated risks.
## Section 12: Sun Exposure and Vitamin D Optimization - The Sunshine Vitamin's Cardiovascular Connection
Daily appropriate sun exposure and vitamin D optimization represent underappreciated but crucial components of cardiovascular health, with research revealing that vitamin D deficiency affects over one billion people worldwide and significantly increases cardiovascular disease risk. The relationship between vitamin D and heart health extends far beyond its traditional role in bone metabolism, as cardiovascular tissues contain vitamin D receptors and the enzyme necessary for converting vitamin D to its active form. Studies consistently show that individuals with vitamin D levels below 20 ng/mL have a 30-50% higher risk of cardiovascular disease, hypertension, and diabetes compared to those with optimal levels above 30 ng/mL. The mechanisms underlying vitamin D's cardiovascular protection are multifaceted and impressive. Adequate vitamin D levels help regulate the renin-angiotensin-aldosterone system, which controls blood pressure and fluid balance, while also supporting healthy endothelial function and reducing arterial calcification. Vitamin D deficiency is associated with increased inflammation, insulin resistance, and elevated parathyroid hormone levels, all of which contribute to cardiovascular disease progression. The optimal approach to vitamin D optimization involves sensible sun exposure,