8 Skin Conditions That Signal an Underlying Health Issue
The skin, our body's largest organ, serves as far more than a protective barrier against the external environment. It functions as a sophisticated diagnostic tool, often revealing the first signs of internal health conditions long before other symptoms manifest. Medical professionals have long recognized that dermatological changes can serve as early warning systems for systemic diseases, autoimmune disorders, hormonal imbalances, and metabolic dysfunction. From subtle color changes to distinctive rashes, the skin's appearance can provide crucial insights into cardiovascular health, liver function, diabetes progression, and even certain cancers. Understanding these connections between skin manifestations and underlying health issues empowers individuals to seek timely medical intervention, potentially preventing serious complications. This comprehensive exploration examines eight significant skin conditions that frequently signal deeper health concerns, providing essential knowledge for recognizing when dermatological symptoms warrant immediate medical attention and comprehensive health evaluation.
1. Acanthosis Nigricans - The Dark Warning of Insulin Resistance
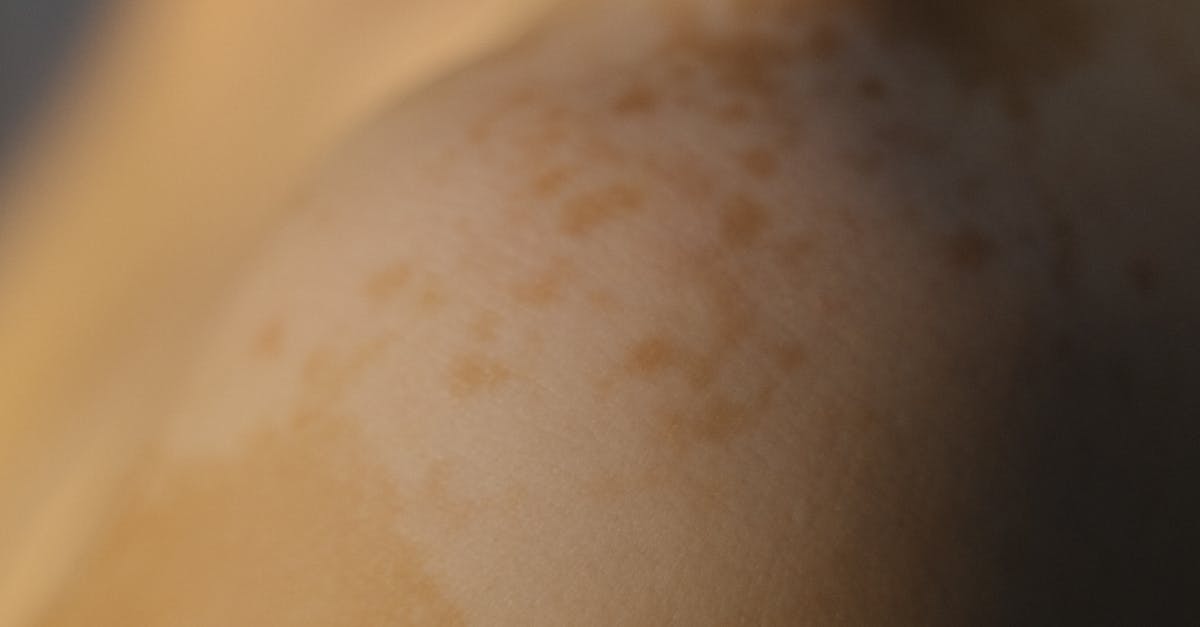
Acanthosis nigricans presents as dark, velvety patches of skin that typically appear in body folds such as the neck, armpits, groin, and under the breasts. This distinctive skin condition serves as a visible marker of insulin resistance, often preceding the development of type 2 diabetes by several years. The darkened skin results from elevated insulin levels that stimulate skin cell growth and melanin production, creating the characteristic hyperpigmented appearance. Research indicates that approximately 70% of individuals with acanthosis nigricans have underlying insulin resistance or diabetes, making this condition a crucial early warning sign. The severity and extent of the darkening often correlate with the degree of insulin resistance, providing healthcare providers with a visual assessment tool for metabolic dysfunction. Beyond diabetes, acanthosis nigricans can also indicate polycystic ovary syndrome (PCOS), Cushing's syndrome, or certain endocrine tumors. Early recognition and intervention through lifestyle modifications, including weight management and dietary changes, can significantly improve insulin sensitivity and may lead to the gradual lightening of affected skin areas, while also preventing the progression to full-blown diabetes.
2. Psoriasis - Autoimmune Inflammation Beyond the Skin
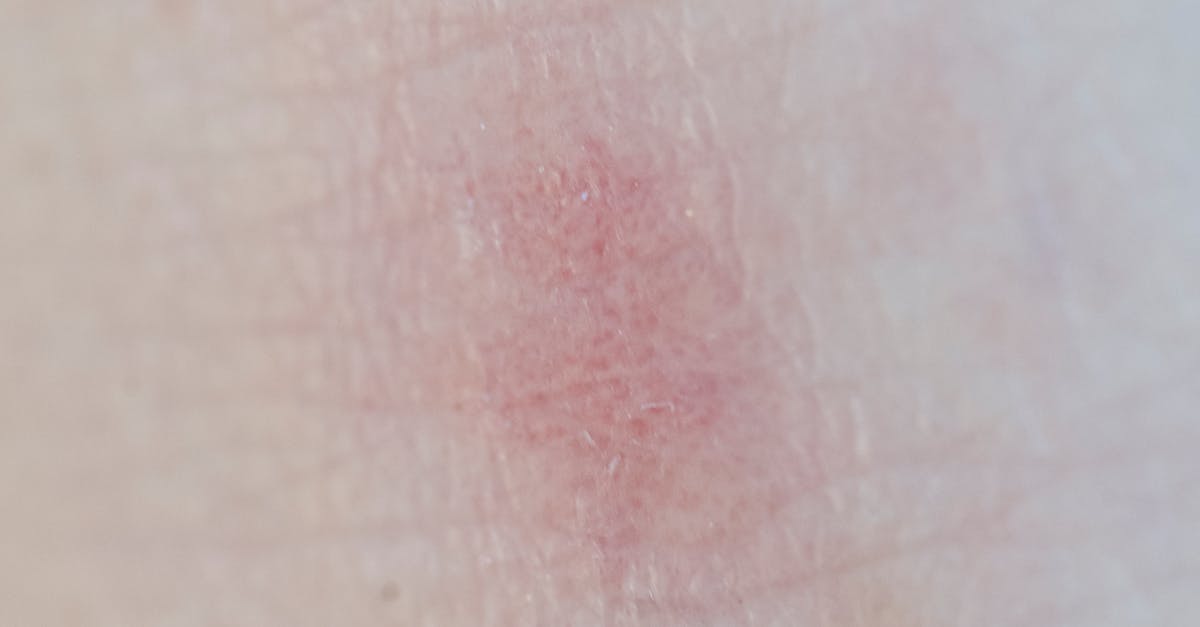
Psoriasis, characterized by raised, red, scaly patches on the skin, represents far more than a cosmetic concern—it's a systemic inflammatory condition with significant implications for overall health. This autoimmune disorder affects approximately 3% of the global population and serves as a visible manifestation of chronic inflammation that extends throughout the body. Research has established strong connections between psoriasis and numerous comorbidities, including cardiovascular disease, metabolic syndrome, inflammatory bowel disease, and depression. The inflammatory cytokines responsible for psoriatic skin lesions also contribute to arterial inflammation, increasing the risk of heart attack and stroke by up to 50% in severe cases. Additionally, individuals with psoriasis face elevated risks of developing psoriatic arthritis, which can cause permanent joint damage if left untreated. The condition also correlates with increased rates of obesity, diabetes, and fatty liver disease, suggesting shared inflammatory pathways. Mental health implications are equally significant, with psoriasis patients experiencing higher rates of anxiety and depression due to both the visible nature of the condition and the systemic inflammatory burden. Modern treatment approaches recognize psoriasis as a systemic disease, emphasizing the importance of comprehensive care that addresses both skin symptoms and associated health risks through targeted therapies and lifestyle interventions.
3. Xanthelasma - Cholesterol Deposits Revealing Cardiovascular Risk
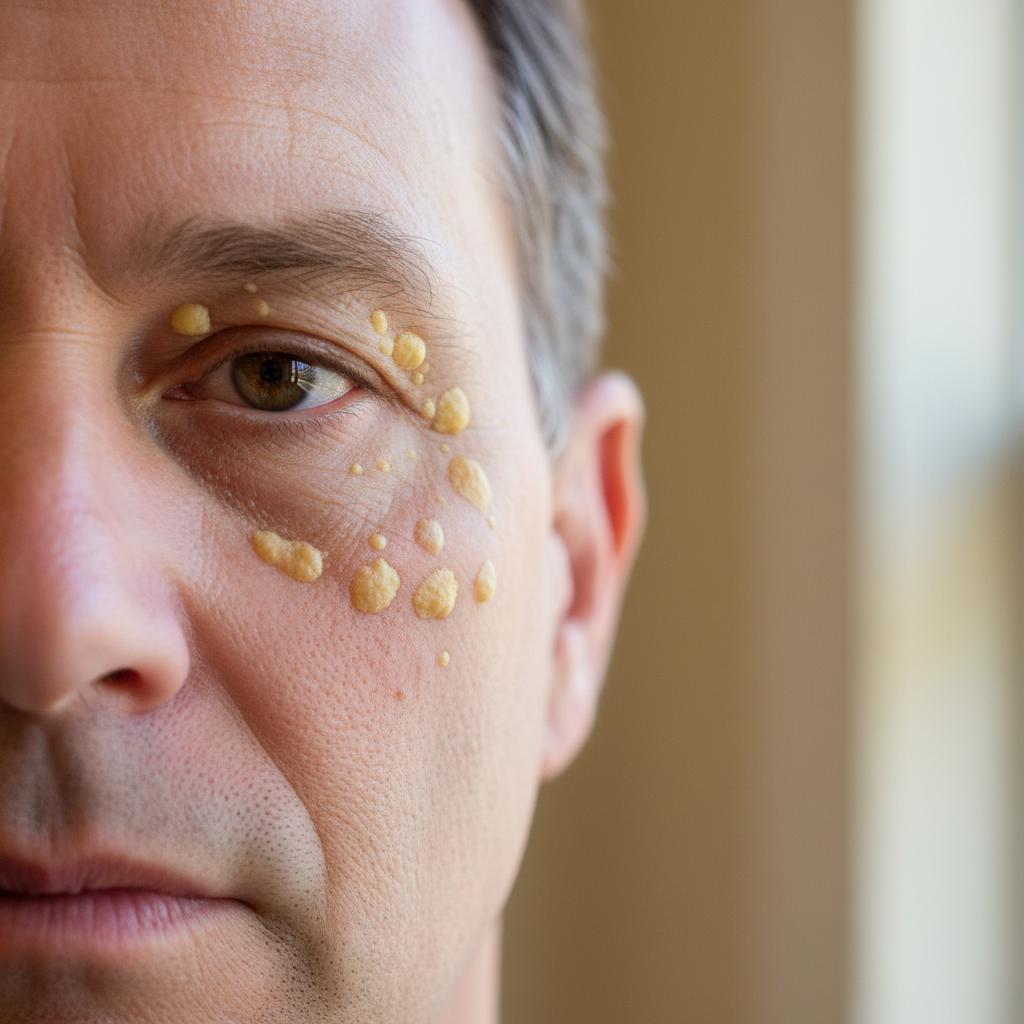
Xanthelasma appears as yellowish, waxy deposits around the eyelids, particularly near the inner corners, and serves as a visible indicator of lipid metabolism disorders and cardiovascular disease risk. These cholesterol-rich lesions develop when excess lipids accumulate in the skin, often reflecting elevated blood cholesterol levels or genetic predisposition to lipid disorders. Studies demonstrate that approximately 50% of individuals with xanthelasma have abnormal lipid profiles, including elevated LDL cholesterol, reduced HDL cholesterol, or elevated triglycerides. More concerning is the strong association with cardiovascular disease—research indicates that people with xanthelasma face a significantly increased risk of heart attack, stroke, and peripheral artery disease, even when cholesterol levels appear normal. This connection exists because xanthelasma can indicate familial hypercholesterolemia, a genetic condition causing extremely high cholesterol levels from birth, or suggest the presence of small, dense LDL particles that are particularly atherogenic. The presence of these lesions should prompt comprehensive cardiovascular risk assessment, including lipid panels, inflammatory markers, and cardiac imaging studies. While xanthelasma can be removed cosmetically through laser therapy or surgical excision, addressing the underlying lipid disorder through dietary modifications, exercise, and potentially statin therapy is crucial for reducing cardiovascular risk and preventing lesion recurrence.
4. Vitiligo - Autoimmune Activity and Associated Conditions
Vitiligo, characterized by the loss of skin pigmentation resulting in white patches, represents an autoimmune condition where the immune system attacks melanocytes, the cells responsible for skin color. While often viewed primarily as a cosmetic concern, vitiligo frequently signals broader autoimmune activity and increased susceptibility to other autoimmune disorders. Research reveals that individuals with vitiligo have significantly higher rates of thyroid disorders, particularly Hashimoto's thyroiditis and Graves' disease, affecting up to 25% of vitiligo patients. The condition also shows strong associations with type 1 diabetes, alopecia areata, pernicious anemia, and Addison's disease, suggesting shared autoimmune pathways and genetic predispositions. The psychological impact of vitiligo extends beyond appearance, as the unpredictable progression and visible nature of the condition can lead to social anxiety, depression, and reduced quality of life. Additionally, the loss of melanocytes eliminates natural sun protection in affected areas, dramatically increasing the risk of skin cancer, particularly in fair-skinned individuals. Recent advances in understanding vitiligo's pathophysiology have led to targeted therapies, including JAK inhibitors and topical immunomodulators, which can halt progression and promote repigmentation. Comprehensive care for vitiligo patients should include regular screening for associated autoimmune conditions, psychological support, and aggressive sun protection measures to prevent secondary complications.
5. Hirsutism - Hormonal Imbalances and Metabolic Disorders

Hirsutism, defined as excessive hair growth in women following a male pattern distribution, serves as a visible manifestation of underlying hormonal imbalances, particularly elevated androgen levels. This condition affects approximately 10% of women and most commonly indicates polycystic ovary syndrome (PCOS), which encompasses a complex array of metabolic and reproductive abnormalities. Beyond PCOS, hirsutism can signal more serious conditions including adrenal tumors, Cushing's syndrome, or congenital adrenal hyperplasia, making proper evaluation crucial for identifying potentially life-threatening disorders. The hormonal disruptions causing hirsutism often coincide with insulin resistance, increasing the risk of type 2 diabetes, cardiovascular disease, and metabolic syndrome. Women with hirsutism frequently experience additional symptoms including irregular menstrual cycles, acne, male-pattern baldness, and weight gain, particularly around the midsection. The psychological impact can be profound, leading to decreased self-esteem, social withdrawal, and depression. Diagnostic evaluation should include comprehensive hormone testing, including testosterone, DHEA-S, 17-hydroxyprogesterone, and prolactin levels, along with assessment for insulin resistance and thyroid function. Treatment approaches vary depending on the underlying cause but may include hormonal contraceptives, anti-androgen medications like spironolactone, metformin for insulin resistance, and cosmetic hair removal techniques. Early intervention can prevent progression of associated metabolic complications while improving quality of life and reproductive health outcomes.
6. Erythema Migrans - The Telltale Sign of Lyme Disease
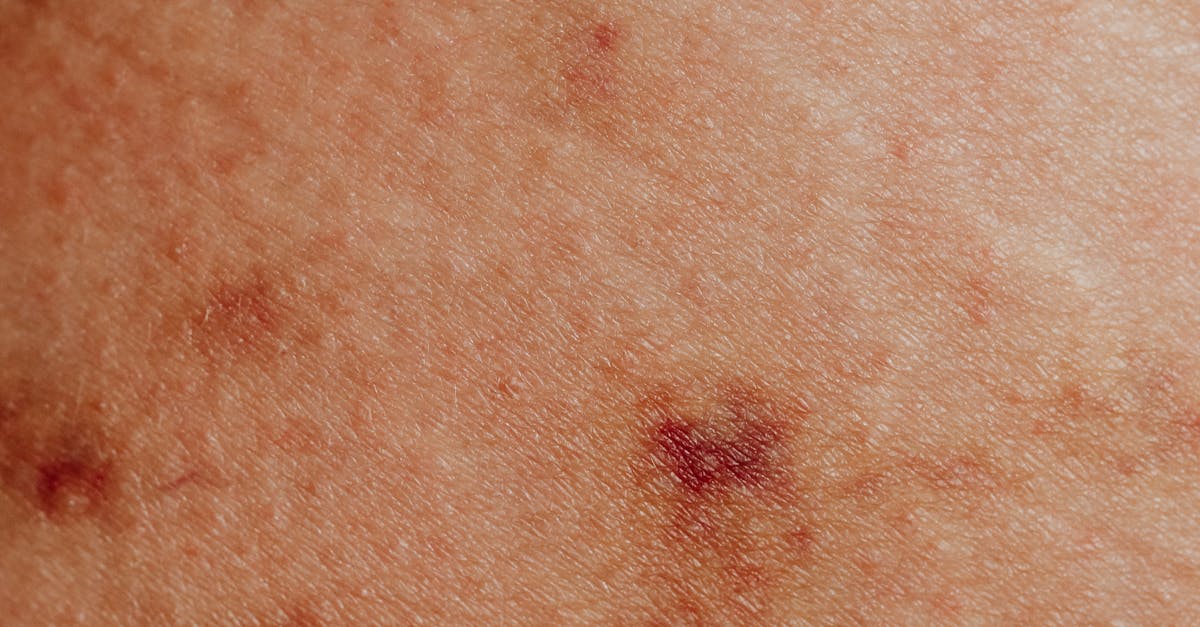
Erythema migrans, the characteristic "bull's-eye" rash of Lyme disease, represents one of the most diagnostically significant skin manifestations in infectious disease medicine. This distinctive rash typically appears 3-30 days after a tick bite infected with Borrelia burgdorferi, beginning as a small red area that gradually expands outward while often clearing in the center, creating the pathognomonic target-like appearance. The rash occurs in approximately 70-80% of Lyme disease cases and serves as the most reliable early indicator of infection, often appearing before other systemic symptoms develop. Recognition of erythema migrans is crucial because early antibiotic treatment can prevent the progression to disseminated Lyme disease, which can affect the heart, joints, and nervous system with potentially devastating consequences. The rash is typically painless and non-itchy, which can lead to delayed recognition, particularly when it appears in less visible locations. Without treatment, the infection can progress to cause cardiac arrhythmias, arthritis, facial paralysis, meningitis, and cognitive impairment. The expanding nature of the rash reflects the spirochete's movement through tissue, and multiple lesions may appear in cases of disseminated infection. Geographic location and seasonal timing provide important diagnostic clues, as Lyme disease is most common in the northeastern and upper Midwestern United States during spring and summer months. Prompt recognition and treatment of erythema migrans with appropriate antibiotics can achieve cure rates exceeding 95%, emphasizing the critical importance of this dermatological diagnosis.
7. Dermatomyositis Rash - Muscle Disease and Cancer Connections
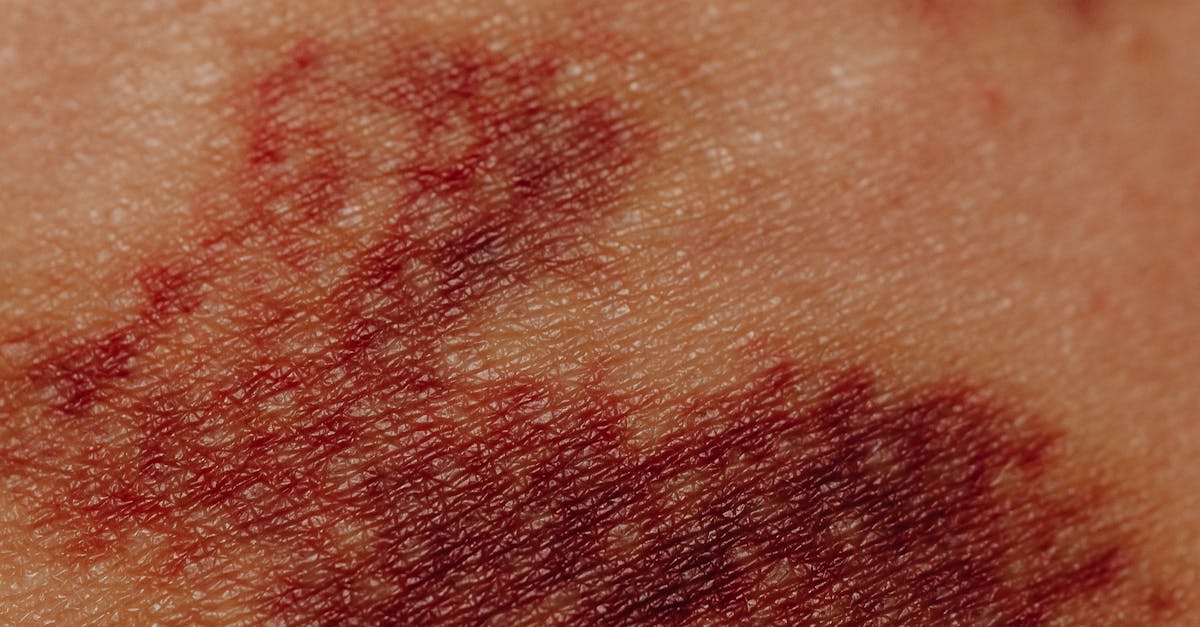
Dermatomyositis presents with distinctive skin changes that serve as hallmarks of an underlying inflammatory muscle disease with significant systemic implications. The characteristic rash includes heliotrope discoloration around the eyes, Gottron's papules over the knuckles, and a shawl-sign rash across the shoulders and upper back. These pathognomonic skin findings often precede or accompany progressive muscle weakness, particularly affecting the proximal muscles of the arms and legs. The condition represents an autoimmune process where inflammatory cells attack both muscle tissue and skin, leading to characteristic histological changes and elevated muscle enzymes. Of particular concern is the strong association between dermatomyositis and malignancy, with studies indicating that 15-25% of adult patients have an underlying cancer, most commonly ovarian, lung, breast, or gastrointestinal tumors. The risk is highest in older patients and those with rapidly progressive disease or certain autoantibody profiles. The inflammatory process in dermatomyositis can also affect internal organs, including the lungs (causing interstitial lung disease), heart (leading to cardiomyopathy), and gastrointestinal tract (resulting in dysphagia and aspiration risk). Early recognition of the characteristic rash should prompt immediate evaluation including muscle enzyme testing, electromyography, muscle biopsy, and comprehensive cancer screening. Treatment typically involves immunosuppressive therapy with corticosteroids and disease-modifying agents, along with aggressive cancer surveillance and supportive care for muscle weakness and skin manifestations.
8. Necrobiosis Lipoidica - Diabetes and Vascular Complications
Necrobiosis lipoidica presents as distinctive yellowish-brown, atrophic plaques with a waxy appearance, most commonly occurring on the shins, and serves as a significant marker of diabetes mellitus and associated vascular complications. This rare but diagnostically important condition affects approximately 0.3% of diabetic patients, with women being affected three times more frequently than men. The lesions typically begin as small, reddish-brown papules that gradually enlarge and develop the characteristic atrophic center with prominent blood vessels visible through the thinned skin. The pathophysiology involves diabetic microangiopathy and collagen degeneration, reflecting the same vascular processes that cause diabetic retinopathy and nephropathy. While necrobiosis lipoidica can occasionally occur in non-diabetic individuals, its presence should prompt comprehensive diabetes screening and evaluation for diabetic complications. The condition often indicates poor glycemic control and advanced microvascular disease, correlating with increased risk of diabetic retinopathy, nephropathy, and neuropathy. The lesions are typically asymptomatic but can become painful or ulcerated, particularly with trauma, leading to chronic wounds that heal poorly due to underlying vascular compromise. The cosmetic impact can be significant, affecting quality of life and self-esteem. Treatment is challenging and often unsatisfactory, focusing on optimal diabetes management, topical corticosteroids, and protection from trauma. The presence of necrobiosis lipoidica should prompt intensified diabetes management and regular screening for other diabetic complications, as it often signals the need for more aggressive therapeutic intervention.
9. Integrating Dermatological Signs into Comprehensive Health Assessment
The intricate relationship between skin manifestations and systemic health underscores the critical importance of viewing dermatological symptoms within the broader context of overall wellness and disease prevention. Each of the eight conditions explored—from acanthosis nigricans signaling metabolic dysfunction to erythema migrans indicating infectious disease—demonstrates how the skin serves as an early warning system for potentially serious underlying health issues. Healthcare providers and patients alike must recognize that skin changes often represent the tip of the iceberg, with more significant pathological processes occurring beneath the surface. The integration of dermatological assessment into routine healthcare evaluation can facilitate earlier diagnosis, more timely intervention, and ultimately better health outcomes across multiple organ systems. Modern medicine's understanding of these skin-systemic health connections continues to evolve, with emerging research revealing new associations and refining our understanding of existing relationships. Patient education regarding these connections empowers individuals to seek appropriate medical attention when concerning skin changes occur, potentially preventing the progression of serious diseases. The multidisciplinary approach to managing these conditions—involving dermatologists, endocrinologists, cardiologists, and other specialists—reflects the complex, interconnected nature of human health. As our knowledge expands, the skin's role as a diagnostic window will likely become even more sophisticated, potentially incorporating genetic markers, inflammatory profiles, and advanced imaging techniques to provide even more precise insights into internal health status, ultimately revolutionizing both preventive care and disease management strategies.