8 Thyroid Disorders and Their Common Symptoms
The thyroid gland, a small butterfly-shaped organ located at the base of your neck, serves as your body's metabolic control center, orchestrating a symphony of physiological processes that affect virtually every organ system. Despite weighing only about 20 grams, this remarkable endocrine gland produces hormones that regulate metabolism, heart rate, body temperature, energy levels, and countless other vital functions. When the thyroid malfunctions, the ripple effects can be profound and far-reaching, manifesting in symptoms that range from subtle fatigue to life-threatening complications. Thyroid disorders affect millions of people worldwide, with women being five to eight times more likely to develop these conditions than men. The complexity of thyroid dysfunction lies in its often insidious onset and the way symptoms can mimic other common health issues, leading to frequent misdiagnosis or delayed treatment. Understanding the eight most prevalent thyroid disorders and their characteristic symptoms is crucial for early detection and effective management, as proper diagnosis and treatment can dramatically improve quality of life and prevent serious complications. From the hyperactive state of Graves' disease to the sluggish metabolism of Hashimoto's thyroiditis, each condition presents unique challenges that require specialized medical attention and personalized treatment approaches.
1. Hypothyroidism - When Your Thyroid Runs Too Slow

Hypothyroidism represents the most common thyroid disorder, affecting approximately 4.6% of the U.S. population aged 12 and older, with the condition occurring when the thyroid gland fails to produce sufficient amounts of thyroid hormones to meet the body's metabolic demands. This hormonal deficiency creates a cascade of symptoms that essentially slow down the body's internal processes, much like a car running on empty fuel. The most frequently reported symptoms include persistent fatigue that doesn't improve with rest, unexplained weight gain despite normal eating habits, cold intolerance that leaves sufferers reaching for sweaters even in warm weather, and a general feeling of mental sluggishness often described as "brain fog." Additional manifestations include dry, coarse skin and hair, brittle nails, constipation, muscle weakness, joint pain, and irregular menstrual periods in women. Many patients also experience mood changes, particularly depression and irritability, which can significantly impact their personal and professional relationships. The insidious nature of hypothyroidism means symptoms often develop gradually over months or years, leading many people to attribute their declining energy and well-being to aging, stress, or other factors. Laboratory diagnosis typically reveals elevated thyroid-stimulating hormone (TSH) levels and decreased free thyroxine (T4) levels, confirming the thyroid's inability to meet the body's hormonal requirements.
2. Hyperthyroidism - When Your Thyroid Goes Into Overdrive
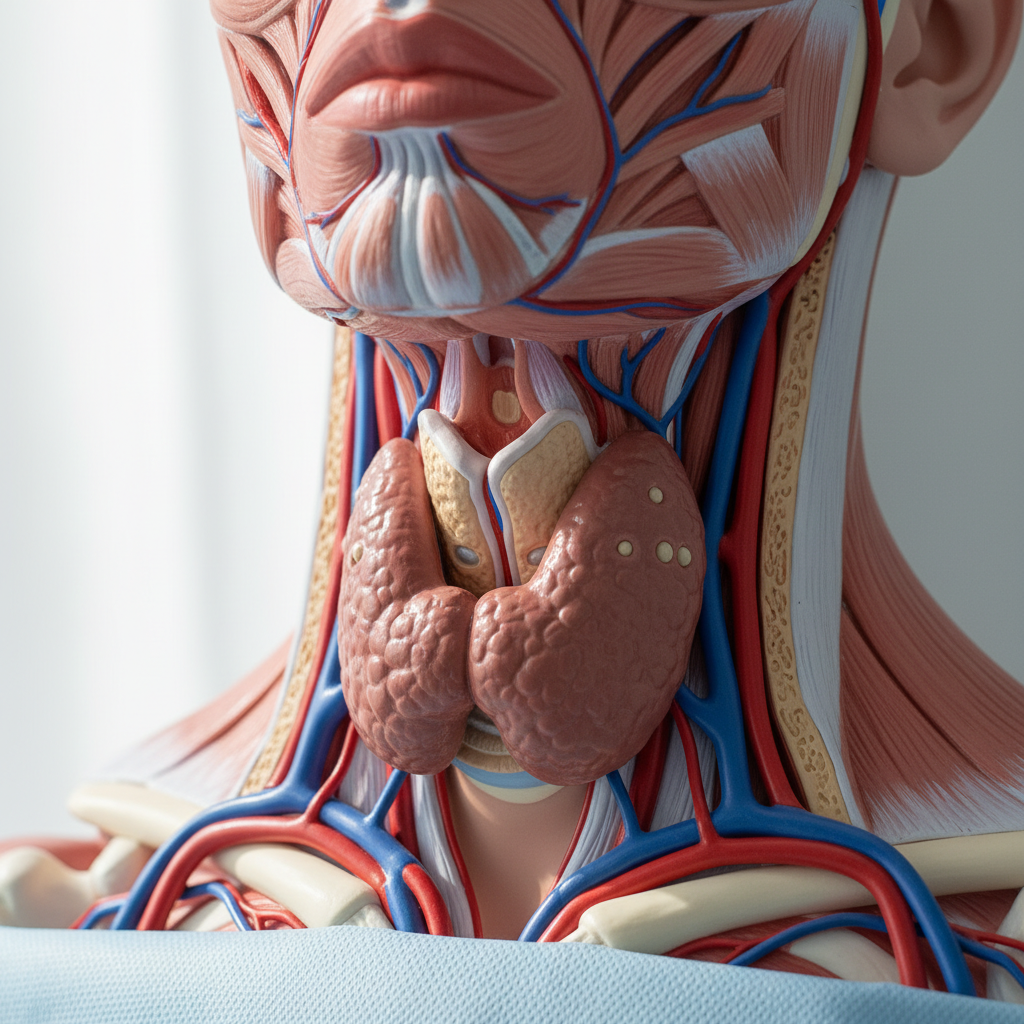
Hyperthyroidism occurs when the thyroid gland produces excessive amounts of thyroid hormones, effectively putting the body's metabolic processes into overdrive and creating a state of heightened physiological activity that can be both uncomfortable and potentially dangerous. This condition affects approximately 1.2% of the population and manifests through a constellation of symptoms that reflect the body's accelerated metabolism and increased energy expenditure. The hallmark symptoms include rapid or irregular heartbeat (palpitations), unexplained weight loss despite increased appetite, excessive sweating and heat intolerance, tremors or shakiness particularly in the hands, anxiety and restlessness, difficulty sleeping, frequent bowel movements or diarrhea, and muscle weakness especially in the upper arms and thighs. Patients often describe feeling "wired" or unable to relax, experiencing racing thoughts, and having difficulty concentrating on tasks. Women may notice lighter or less frequent menstrual periods, while both sexes might experience hair thinning or loss. The psychological impact can be significant, with many patients reporting increased irritability, mood swings, and anxiety that can strain relationships and affect work performance. In severe cases, hyperthyroidism can lead to a life-threatening condition called thyroid storm, characterized by extremely high fever, rapid heart rate, and altered mental status requiring immediate medical intervention. Laboratory tests typically show suppressed TSH levels and elevated free T4 and/or T3 levels, confirming the overproduction of thyroid hormones.
3. Hashimoto's Thyroiditis - The Autoimmune Attack on Your Thyroid
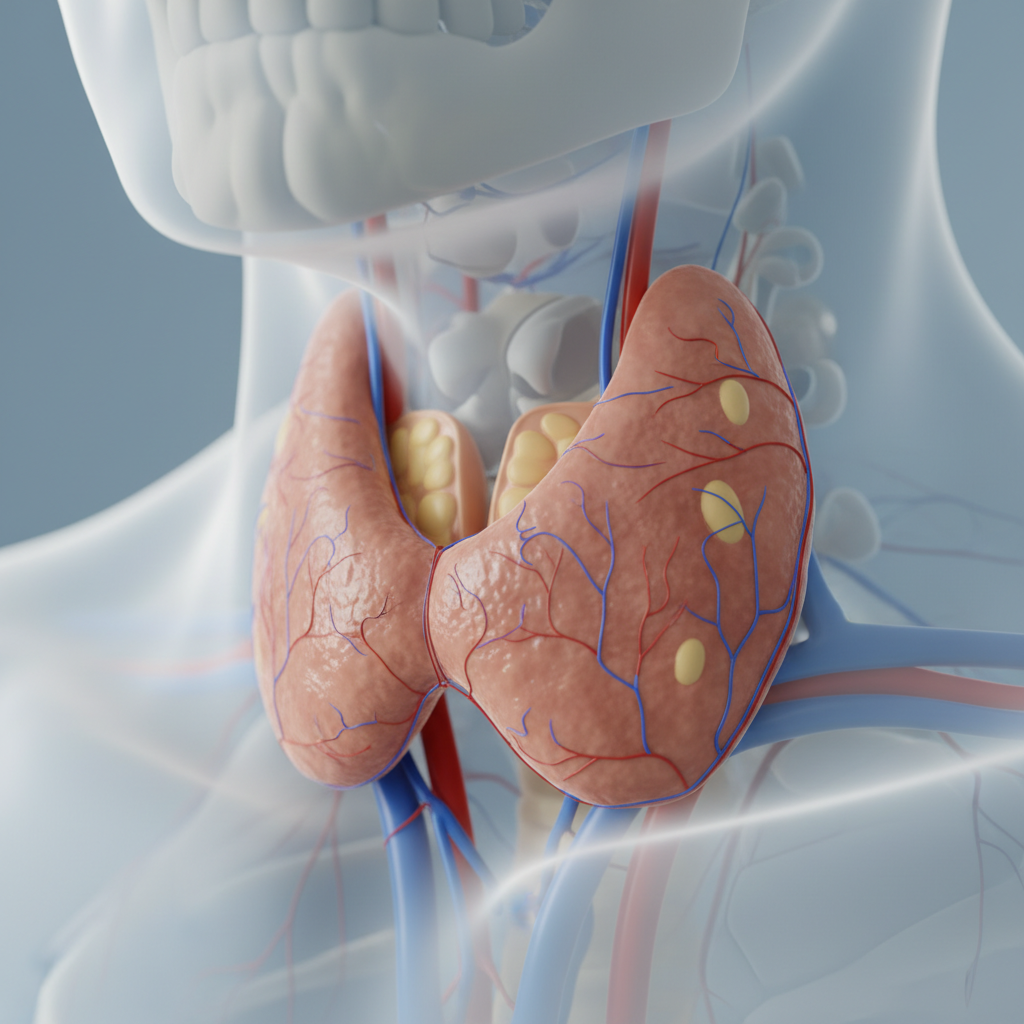
Hashimoto's thyroiditis, also known as chronic lymphocytic thyroiditis, represents the most common cause of hypothyroidism in developed countries and exemplifies how the body's immune system can mistakenly turn against its own tissues. This autoimmune condition occurs when the immune system produces antibodies that attack and gradually destroy thyroid tissue, leading to progressive thyroid dysfunction and eventual hormone deficiency. Named after Japanese physician Hakaru Hashimoto who first described it in 1912, this condition affects women approximately seven times more frequently than men and often has a genetic component, running in families alongside other autoimmune disorders. The symptoms of Hashimoto's thyroiditis typically mirror those of hypothyroidism but may fluctuate in severity as the autoimmune process waxes and wanes. Patients commonly experience fatigue, weight gain, cold sensitivity, dry skin and hair, constipation, muscle aches, and depression, but these symptoms may vary in intensity over time. A distinctive feature of Hashimoto's is the potential for thyroid enlargement (goiter), which may cause a feeling of fullness in the neck, difficulty swallowing, or a visible swelling at the base of the throat. Some patients experience periods where symptoms temporarily worsen or improve as the inflammatory process affects different areas of the thyroid gland. The diagnosis is confirmed through blood tests showing elevated TSH, decreased free T4, and the presence of thyroid peroxidase (TPO) antibodies or thyroglobulin antibodies, which indicate the autoimmune nature of the condition.
4. Graves' Disease - The Most Common Cause of Hyperthyroidism

Graves' disease stands as the leading cause of hyperthyroidism, accounting for approximately 70-80% of all hyperthyroid cases and representing another example of autoimmune dysfunction where the body's immune system mistakenly stimulates rather than destroys thyroid tissue. Named after Irish physician Robert Graves who described the condition in 1835, this disorder occurs when antibodies called thyroid-stimulating immunoglobulins (TSI) bind to and activate the thyroid-stimulating hormone receptor, causing the thyroid gland to produce excessive amounts of hormones continuously. While Graves' disease shares many symptoms with other forms of hyperthyroidism, it presents several distinctive features that help differentiate it from other thyroid conditions. The classic triad of symptoms includes hyperthyroidism, diffuse goiter (enlarged thyroid gland), and Graves' ophthalmopathy, which affects the eyes and surrounding tissues. The eye-related symptoms, occurring in about 25-50% of patients, can include bulging eyes (exophthalmos), double vision, eye pain, excessive tearing, light sensitivity, and a gritty sensation in the eyes. These ocular manifestations result from inflammation and swelling of the muscles and tissues behind the eyes, and they can sometimes occur even before other thyroid symptoms become apparent. Additional unique features of Graves' disease may include pretibial myxedema, a rare skin condition causing thickening and redness of the skin on the shins, and in some cases, clubbing of the fingers and toes. The emotional and psychological impact of Graves' disease can be particularly challenging due to the combination of hyperthyroid symptoms and the cosmetic concerns related to eye changes.
5. Thyroid Nodules - Understanding Lumps and Bumps on Your Thyroid
Thyroid nodules are discrete lumps or masses that develop within the thyroid gland, representing one of the most common thyroid abnormalities encountered in clinical practice, with studies suggesting that up to 50% of people will develop thyroid nodules during their lifetime, though many remain undetected. These growths can vary significantly in size, composition, and clinical significance, ranging from tiny, inconsequential bumps to large masses that cause visible neck swelling or compression symptoms. The vast majority of thyroid nodules—approximately 90-95%—are benign (non-cancerous), but the presence of nodules often causes considerable anxiety for patients due to concerns about cancer. Most thyroid nodules are asymptomatic and discovered incidentally during routine physical examinations or imaging studies performed for other reasons, earning them the designation "incidentalomas." However, larger nodules may produce noticeable symptoms including a visible lump or swelling in the neck, difficulty swallowing (dysphagia), a sensation of pressure or fullness in the throat, hoarseness or voice changes if the nodule presses on the recurrent laryngeal nerve, and rarely, difficulty breathing if the nodule is large enough to compress the trachea. Some nodules, called "hot" or hyperfunctioning nodules, can produce excess thyroid hormone independently of normal regulatory mechanisms, leading to symptoms of hyperthyroidism such as rapid heartbeat, weight loss, nervousness, and heat intolerance. The evaluation of thyroid nodules typically involves a combination of physical examination, thyroid function tests, ultrasound imaging, and often fine-needle aspiration biopsy to determine whether the nodule is benign or malignant and to guide appropriate treatment decisions.
6. Thyroid Cancer - Recognizing the Warning Signs

Thyroid cancer, while representing only about 1% of all cancers, has shown a significant increase in incidence over the past several decades, making it the fastest-growing cancer diagnosis in the United States, though this increase is largely attributed to improved detection methods rather than a true rise in disease occurrence. The four main types of thyroid cancer—papillary, follicular, medullary, and anaplastic—each present with different characteristics and prognoses, with papillary thyroid cancer being the most common and generally having the best outcomes when detected early. The symptoms of thyroid cancer can be subtle and often overlap with those of benign thyroid conditions, which is why many cases are discovered during routine examinations or imaging studies rather than through patient-reported symptoms. The most common presenting symptom is a painless lump or nodule in the neck that may be felt during self-examination or detected by a healthcare provider during a routine physical exam. As the cancer progresses, patients may experience persistent hoarseness or voice changes that don't resolve, difficulty swallowing that progressively worsens, persistent cough not related to a cold or respiratory infection, pain in the neck or throat that may radiate to the ears, and swollen lymph nodes in the neck. Unlike benign thyroid conditions, thyroid cancer typically does not cause significant changes in thyroid hormone levels, so patients usually don't experience the classic symptoms of hyperthyroidism or hypothyroidism unless the cancer has extensively damaged the thyroid gland. The key to successful treatment lies in early detection, as most thyroid cancers have excellent survival rates when caught in their early stages, with five-year survival rates exceeding 95% for localized papillary and follicular thyroid cancers.
7. Goiter - When Your Thyroid Becomes Enlarged
Goiter, defined as an abnormal enlargement of the thyroid gland, represents a visible manifestation of various underlying thyroid disorders and can occur in association with normal, increased, or decreased thyroid hormone production. This condition affects millions of people worldwide and can range from barely noticeable swelling to dramatic neck enlargement that causes significant cosmetic concerns and functional problems. The development of goiter can result from numerous causes, including iodine deficiency (the most common cause globally), autoimmune thyroid diseases like Hashimoto's thyroiditis or Graves' disease, thyroid nodules, inflammation, or certain medications. In regions with adequate iodine intake, autoimmune thyroid disease represents the most frequent cause of goiter development. The symptoms associated with goiter depend largely on its size and the underlying cause, with small goiters often producing no symptoms at all while larger ones can cause significant discomfort and functional impairment. Common symptoms include visible swelling at the base of the neck that may be more noticeable when looking in a mirror or wearing tight-fitting clothing, a feeling of tightness or fullness in the throat, difficulty swallowing (dysphagia) especially when consuming solid foods, shortness of breath or difficulty breathing particularly when lying flat, coughing that persists without other signs of respiratory illness, and hoarseness or voice changes due to pressure on the vocal cords. Some patients describe a choking sensation or the feeling that something is stuck in their throat. The psychological impact of visible goiter can be substantial, affecting self-esteem and social interactions, particularly in cases where the enlargement is cosmetically significant.
8. Thyroiditis - Understanding Thyroid Inflammation
Thyroiditis encompasses a group of inflammatory conditions affecting the thyroid gland, each with distinct causes, clinical presentations, and treatment approaches, making it essential to understand the various forms this condition can take. The inflammation can result from autoimmune processes, viral infections, bacterial infections, radiation exposure, or certain medications, and the clinical course can vary dramatically depending on the underlying cause. The most common forms include Hashimoto's thyroiditis (chronic autoimmune thyroiditis), subacute thyroiditis (also known as de Quervain's thyroiditis), postpartum thyroiditis, silent thyroiditis, and acute infectious thyroiditis. Each type presents with a unique constellation of symptoms and follows a different clinical trajectory. Subacute thyroiditis, often triggered by viral infections, typically presents with severe neck pain that may radiate to the jaw, ears, or chest, accompanied by fever, malaise, and symptoms of hyperthyroidism as stored thyroid hormone is released from the inflamed gland. Patients often describe the neck pain as excruciating and may notice that it worsens with swallowing or neck movement. The condition typically progresses through phases, beginning with hyperthyroidism due to hormone release, followed by a hypothyroid phase as hormone stores become depleted, and finally returning to normal thyroid function in most cases. Postpartum thyroiditis affects approximately 5-10% of women within the first year after childbirth and follows a similar pattern of initial hyperthyroidism followed by hypothyroidism, though the neck pain characteristic of subacute thyroiditis is typically absent. Silent thyroiditis presents similarly to postpartum thyroiditis but occurs in individuals who haven't recently given birth and may be related to autoimmune processes or other triggers.
9. Thyroid Storm and Myxedema Coma - Life-Threatening Thyroid Emergencies

Thyroid storm and myxedema coma represent the most severe manifestations of hyperthyroidism and hypothyroidism, respectively, constituting true medical emergencies that require immediate recognition and aggressive treatment to prevent potentially fatal outcomes. These conditions illustrate how thyroid disorders, when left untreated or inadequately managed, can progress to life-threatening states that affect multiple organ systems simultaneously. Thyroid storm, also known as thyrotoxic crisis, occurs when hyperthyroidism reaches extreme levels, typically triggered by stressors such as infection, surgery, trauma, pregnancy, or discontinuation of antithyroid medications. This condition presents with dramatically exaggerated symptoms of hyperthyroidism including extremely high fever (often exceeding 104°F), rapid heart rate that may exceed 150 beats per minute, severe agitation or delirium, profuse sweating, nausea and vomiting, diarrhea, and potentially cardiovascular collapse. Patients may appear confused, restless, or even psychotic, and the condition can rapidly progress to coma and death if not treated promptly. Myxedema coma, conversely, represents the end stage of severe, untreated hypothyroidism and is characterized by profound mental status changes, hypothermia (body temperature often below 95°F), slow heart rate, low blood pressure, decreased breathing rate, and potentially life-threatening complications such as respiratory failure, heart failure, and coma. This condition typically affects elderly patients with long-standing hypothyroidism and may be precipitated by factors such as infection, cold exposure, surgery, or certain medications. Both conditions require immediate hospitalization and intensive care management, with thyroid storm requiring rapid reduction of thyroid hormone levels and supportive care for hyperthermia and cardiovascular instability, while myxedema coma necessitates careful thyroid hormone replacement and management of hypothermia and cardiovascular complications.