10 Oral Health Habits With Proven Links to Systemic Disease Prevention
The human mouth serves as far more than a gateway for food and speech—it functions as a critical window into overall systemic health, harboring complex microbial ecosystems that profoundly influence cardiovascular, metabolic, neurological, and immune system function throughout the body. Groundbreaking research over the past two decades has revolutionized our understanding of oral health, revealing that periodontal disease, oral inflammation, and pathogenic bacterial overgrowth in the mouth create cascading effects that significantly increase risks for heart disease, diabetes, stroke, Alzheimer's disease, respiratory infections, and even certain cancers. The oral cavity contains over 700 species of bacteria, many of which can enter the bloodstream through inflamed or bleeding gums, triggering systemic inflammatory responses that contribute to chronic disease development. This emerging field of oral-systemic health has prompted leading medical organizations to recognize that maintaining optimal oral hygiene represents one of the most accessible and cost-effective strategies for preventing serious health conditions. The following evidence-based oral health habits demonstrate remarkable potential for reducing systemic disease risk while promoting longevity and overall wellness.
1. Daily Flossing - Disrupting the Inflammatory Cascade
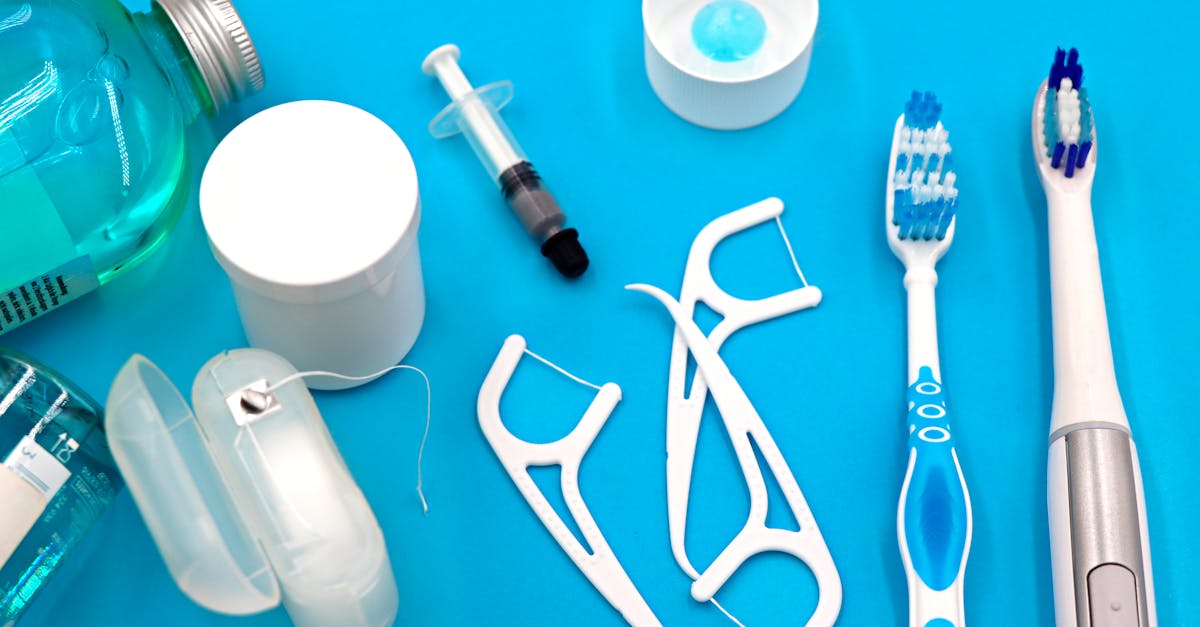
Daily flossing represents perhaps the most underutilized yet scientifically validated intervention for preventing systemic disease through oral health optimization. Research published in the Journal of Periodontology demonstrates that individuals who floss daily show significantly reduced levels of C-reactive protein (CRP), a key inflammatory marker associated with cardiovascular disease risk. The mechanical action of flossing removes bacterial biofilms from interdental spaces where toothbrush bristles cannot reach, preventing the accumulation of pathogenic bacteria like Porphyromonas gingivalis and Aggregatibacter actinomycetemcomitans, which have been directly linked to atherosclerotic plaque formation in coronary arteries. Studies indicate that people with periodontal disease face a 25-50% increased risk of coronary heart disease, making flossing a critical preventive measure. The technique involves gently sliding dental floss between teeth using a sawing motion, wrapping it around each tooth in a C-shape, and moving it up and down to remove plaque and debris. Proper flossing stimulates healthy blood flow to the gums while preventing the bacterial translocation that can trigger systemic inflammation. Clinical trials show that consistent flossing for just two weeks can reduce gingival bleeding by up to 38% and decrease inflammatory markers throughout the body.
2. Twice-Daily Brushing with Fluoride Toothpaste - Fortifying Systemic Defense
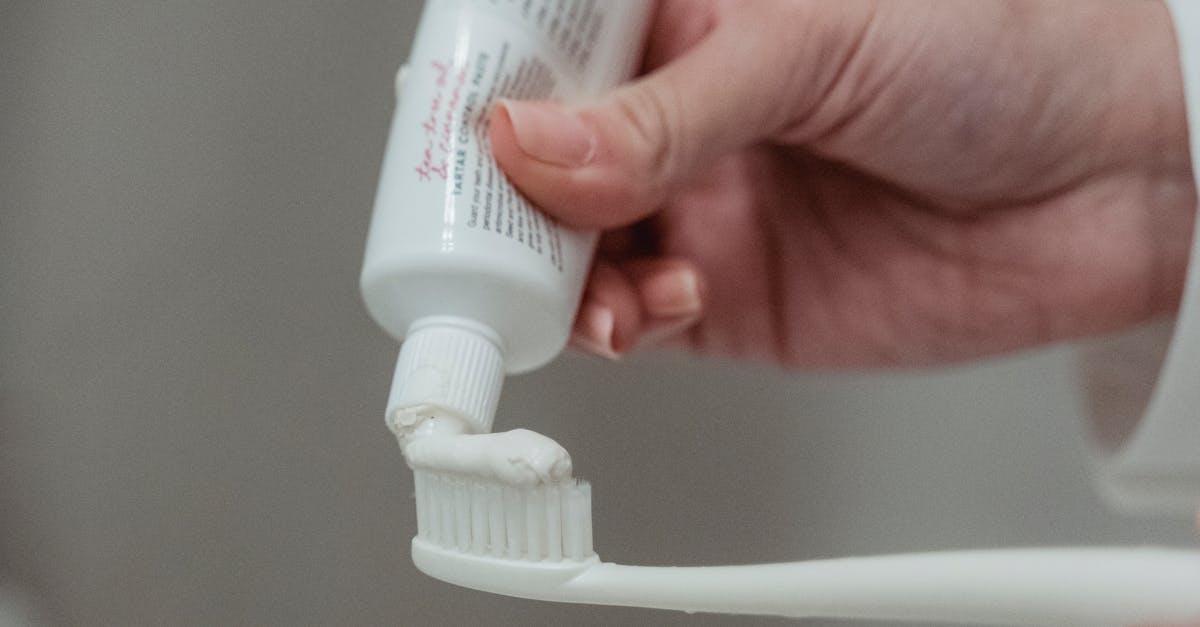
The simple act of brushing teeth twice daily with fluoride toothpaste creates a powerful protective barrier against systemic disease by maintaining optimal oral pH, reducing harmful bacterial loads, and preventing the inflammatory processes that contribute to chronic illness. Research from the American Heart Association reveals that individuals who brush their teeth less than twice daily have a 70% higher risk of developing heart disease compared to those who maintain consistent brushing habits. Fluoride toothpaste not only prevents dental caries but also possesses antimicrobial properties that inhibit the growth of pathogenic oral bacteria responsible for producing inflammatory cytokines and endotoxins. The mechanical action of proper brushing—using a soft-bristled toothbrush at a 45-degree angle to the gumline with gentle circular motions for two minutes—removes bacterial biofilms before they can mature and release toxins into the bloodstream. Studies demonstrate that effective brushing reduces oral bacterial counts by up to 85% immediately after cleaning, with sustained reductions lasting several hours. The timing of brushing is equally important; morning brushing removes overnight bacterial accumulation, while evening brushing eliminates food particles and bacteria that could proliferate during sleep when saliva production naturally decreases.
3. Regular Professional Dental Cleanings - Clinical Intervention for Disease Prevention
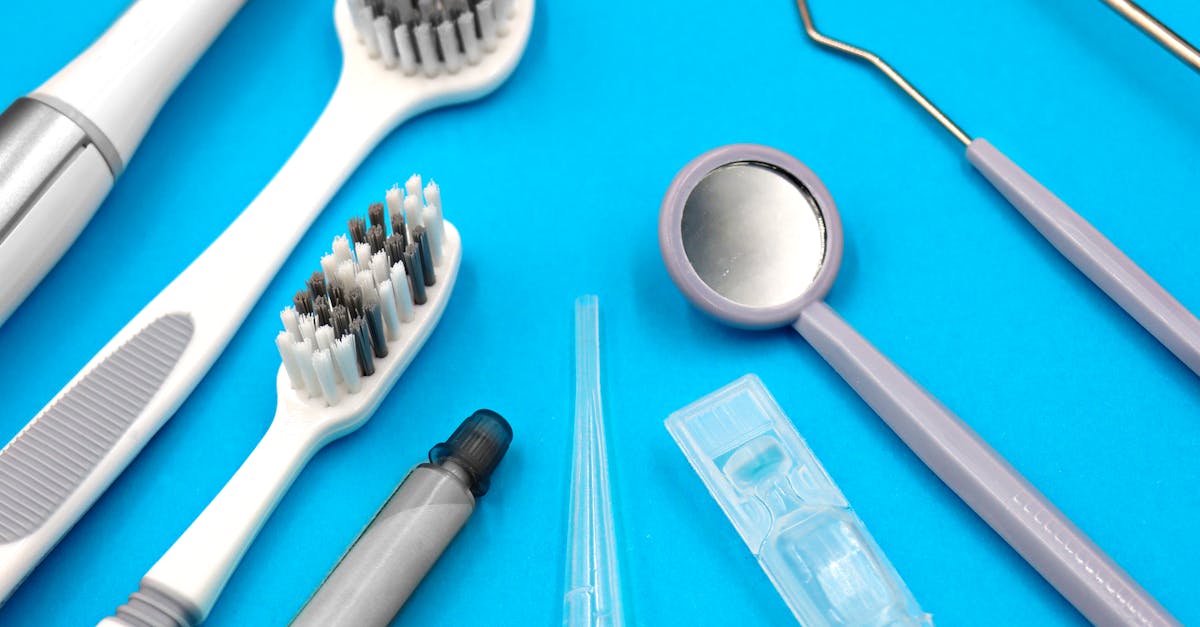
Professional dental cleanings performed every six months represent a crucial clinical intervention that extends far beyond cosmetic benefits, serving as a frontline defense against systemic diseases through the removal of calcified bacterial deposits and early detection of oral health problems. Research published in the American Journal of Preventive Medicine followed over 100,000 individuals for eight years and found that those receiving regular dental cleanings had 24% fewer heart attacks and 13% fewer strokes compared to those who neglected professional oral care. During professional cleanings, dental hygienists use specialized ultrasonic instruments and hand scalers to remove tartar and bacterial biofilms from below the gumline—areas inaccessible through home care alone. This process, known as scaling and root planing when performed therapeutically, reduces bacterial endotoxin levels and inflammatory markers throughout the body. Studies show that professional cleanings can reduce systemic inflammatory markers like interleukin-6 and tumor necrosis factor-alpha by up to 30% within weeks of treatment. The procedure also allows for early detection of oral cancer, periodontal disease, and other conditions that could impact systemic health. Regular cleanings help maintain healthy pocket depths around teeth, preventing the deep bacterial colonization associated with increased risks of diabetes complications, respiratory infections, and adverse pregnancy outcomes.
4. Antimicrobial Mouthwash Use - Targeting Pathogenic Bacteria

Strategic use of antimicrobial mouthwash provides an additional layer of protection against systemic disease by reaching areas of the mouth that brushing and flossing may miss while specifically targeting pathogenic bacteria linked to inflammatory conditions throughout the body. Clinical studies demonstrate that therapeutic mouthwashes containing cetylpyridinium chloride, chlorhexidine, or essential oils can reduce harmful oral bacteria by up to 99.9% and maintain these reductions for several hours post-use. Research from the Journal of Clinical Periodontology shows that individuals using antimicrobial mouthwash daily experience significant reductions in gingival inflammation and bleeding, which correlates with decreased systemic inflammatory markers. The key lies in selecting mouthwashes with proven antimicrobial efficacy rather than cosmetic products that merely mask odors. Therapeutic mouthwashes work by disrupting bacterial cell walls, inhibiting bacterial enzyme activity, and creating an inhospitable environment for pathogenic microorganisms. Studies indicate that regular mouthwash use can reduce the bacterial load associated with respiratory infections, particularly important for elderly individuals and those with compromised immune systems. The optimal protocol involves using mouthwash after brushing and flossing, swishing for 30-60 seconds to ensure adequate contact time with oral tissues, and avoiding eating or drinking for 30 minutes afterward to maximize antimicrobial benefits.
5. Tongue Cleaning - Eliminating Hidden Bacterial Reservoirs

Tongue cleaning represents a frequently overlooked yet scientifically validated practice that significantly reduces oral bacterial loads and associated systemic health risks by addressing one of the mouth's largest bacterial reservoirs. The tongue's papillated surface provides an ideal environment for bacterial colonization, harboring up to 50% of the mouth's total bacterial population, including species directly linked to cardiovascular disease and respiratory infections. Research published in the Journal of Periodontology demonstrates that individuals who clean their tongues daily show marked reductions in volatile sulfur compounds, bacterial endotoxins, and inflammatory markers compared to those who neglect this practice. The process involves using a tongue scraper or toothbrush to gently remove the bacterial coating from the tongue's surface, working from back to front with light pressure to avoid tissue damage. Studies indicate that proper tongue cleaning can reduce overall oral bacterial counts by up to 75% and significantly decrease the risk of bacterial aspiration into the lungs, particularly important for elderly individuals prone to pneumonia. Clinical trials show that tongue cleaning enhances the effectiveness of other oral hygiene measures, creating a synergistic effect that maximizes systemic health benefits. The practice also improves taste sensation and reduces halitosis while contributing to overall oral ecosystem balance that supports immune function and reduces inflammatory burden throughout the body.
6. Sugar Reduction and Dietary Modifications - Starving Pathogenic Bacteria

Reducing dietary sugar intake and implementing strategic nutritional modifications creates an inhospitable environment for pathogenic oral bacteria while supporting beneficial microbial populations that contribute to systemic health and disease prevention. Research from the American Journal of Clinical Nutrition demonstrates that individuals consuming high-sugar diets show significantly increased levels of inflammatory oral bacteria and elevated systemic inflammatory markers compared to those following low-sugar nutritional protocols. Pathogenic bacteria like Streptococcus mutans and Lactobacillus species thrive on simple sugars, producing acid byproducts that not only cause dental decay but also create inflammatory conditions that can trigger systemic health problems. Studies indicate that reducing added sugar intake to less than 10% of total daily calories can decrease harmful oral bacterial populations by up to 40% within just two weeks. Beyond sugar reduction, incorporating foods rich in polyphenols, omega-3 fatty acids, and prebiotics supports beneficial oral bacteria that compete with pathogenic species for resources and attachment sites. Research shows that foods like green tea, cranberries, and fermented vegetables contain compounds that specifically inhibit harmful oral bacteria while promoting beneficial microbial diversity. The timing of food consumption also matters; avoiding frequent snacking and implementing intermittent fasting protocols allows saliva pH to neutralize and beneficial bacteria to reestablish dominance in the oral ecosystem.
7. Hydration and Saliva Production - Maintaining Natural Defense Systems

Optimal hydration and saliva production serve as the mouth's primary natural defense mechanisms against pathogenic bacteria, with adequate fluid intake directly correlating to reduced systemic disease risk through enhanced oral immune function and bacterial clearance. Saliva contains over 3,000 proteins, including antimicrobial peptides, immunoglobulins, and enzymes that actively combat harmful bacteria while maintaining oral pH balance and facilitating the remineralization of tooth enamel. Research published in the Journal of Dental Research reveals that individuals with chronic dehydration or reduced saliva production face significantly increased risks of oral infections, which can subsequently lead to systemic complications including endocarditis, pneumonia, and exacerbated diabetes management. The recommended daily water intake of 8-10 glasses not only maintains adequate saliva production but also helps flush bacteria and food particles from the mouth, reducing the substrate available for pathogenic bacterial growth. Studies demonstrate that proper hydration increases saliva flow rates by up to 30% and enhances the concentration of protective proteins within saliva. Certain medications, medical conditions, and aging can compromise saliva production, making conscious hydration efforts even more critical for maintaining oral and systemic health. Clinical trials show that individuals who maintain optimal hydration levels experience fewer oral infections, reduced gingival inflammation, and lower systemic inflammatory markers compared to those with chronic mild dehydration.
8. Stress Management and Sleep Optimization - Supporting Oral Immune Function

Chronic stress and poor sleep quality significantly compromise oral immune function, creating conditions that favor pathogenic bacterial overgrowth and increase systemic disease risk through multiple interconnected pathways. Research from the Journal of Periodontology demonstrates that individuals experiencing chronic stress show elevated levels of cortisol, which suppresses local immune responses in the mouth and allows harmful bacteria to proliferate unchecked. Sleep deprivation further compounds these effects by reducing the production of antimicrobial proteins in saliva and impairing the body's ability to repair oral tissues damaged by bacterial toxins. Studies indicate that people sleeping less than six hours per night have a 30% higher risk of developing severe periodontal disease compared to those obtaining adequate rest. Stress-induced behaviors like teeth grinding (bruxism) can create micro-trauma to oral tissues, providing entry points for bacteria to invade deeper structures and trigger inflammatory responses. Effective stress management techniques including meditation, regular exercise, and cognitive behavioral therapy have been shown to reduce cortisol levels and improve oral health outcomes. Research reveals that individuals practicing stress reduction techniques experience significant improvements in gingival health and reduced systemic inflammatory markers within 8-12 weeks. Quality sleep of 7-9 hours per night supports optimal immune function, allowing the body to effectively combat oral pathogens and maintain the delicate microbial balance essential for preventing systemic disease.
9. Tobacco and Alcohol Cessation - Eliminating Major Risk Factors

Tobacco use and excessive alcohol consumption represent two of the most significant modifiable risk factors for both oral disease and associated systemic health complications, with cessation providing immediate and long-term benefits for disease prevention. Research published in the Journal of the American Medical Association shows that tobacco users face a 2-7 times higher risk of periodontal disease, with smoking specifically impairing immune cell function in the mouth and reducing blood flow to oral tissues. The chemicals in tobacco products create an environment that favors pathogenic bacteria while suppressing beneficial microbial populations, leading to increased inflammatory burden throughout the body. Studies demonstrate that smoking cessation results in measurable improvements in oral health within just two weeks, with continued benefits accumulating over months and years. Alcohol consumption, particularly when excessive, disrupts oral pH balance, reduces saliva production, and compromises immune function, creating conditions that promote bacterial overgrowth and inflammation. Research indicates that heavy alcohol users show significantly elevated levels of oral pathogens associated with cardiovascular disease and certain cancers. The combination of tobacco and alcohol creates synergistic effects that dramatically increase risks of oral cancer, periodontal disease, and related systemic complications. Clinical studies reveal that individuals who successfully quit tobacco and moderate alcohol consumption experience substantial reductions in inflammatory markers, improved cardiovascular health, and enhanced immune function within 6-12 months of cessation.
10. Regular Oral Cancer Screenings - Early Detection for Systemic Health
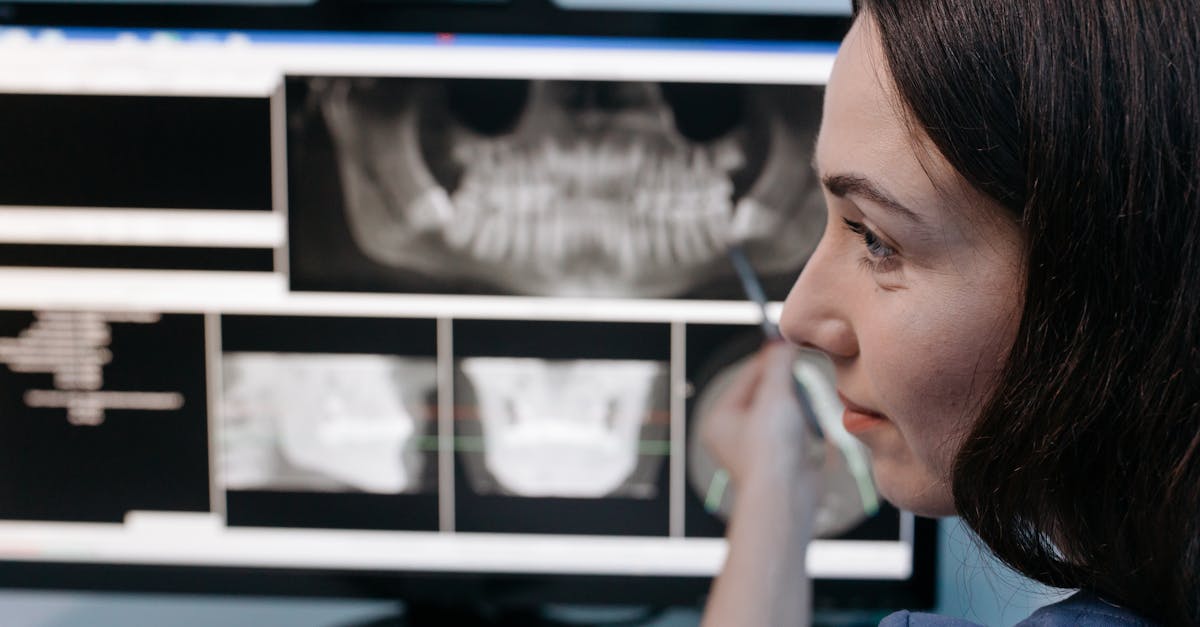
Regular oral cancer screenings performed by dental professionals serve as a critical component of systemic disease prevention, enabling early detection of malignancies that can have far-reaching health consequences if left undiagnosed. Oral cancer affects over 50,000 Americans annually, with five-year survival rates dramatically improving when detected in early stages—from 84% for localized disease to just 39% for advanced cases that have spread to distant sites. Research from the American Cancer Society demonstrates that routine oral examinations can identify precancerous lesions and early-stage cancers that may not yet present obvious symptoms, allowing for interventions that prevent progression to life-threatening systemic disease. The screening process involves visual and tactile examination of all oral tissues, including the tongue, floor of the mouth, soft palate, and throat, looking for unusual lesions, persistent sores, or changes in tissue color and texture. Studies indicate that oral cancer often develops in conjunction with other systemic health problems, including compromised immune function and chronic inflammatory conditions that may be addressed through comprehensive oral health management. Advanced screening technologies like VELscope fluorescence imaging and toluidine blue staining can detect cellular changes not visible to the naked eye, improving diagnostic accuracy and enabling earlier intervention. Regular screenings also provide opportunities for dental professionals to assess overall oral health status and identify risk factors that may contribute to both oral and systemic disease development.
11. Integrating Oral Health into Comprehensive Wellness
The overwhelming scientific evidence presented throughout this exploration clearly demonstrates that optimal oral health practices represent one of the most accessible and effective strategies for preventing serious systemic diseases while promoting overall wellness and longevity. The interconnected nature of oral and systemic health means that the simple daily habits of proper brushing, flossing, and professional care create cascading benefits that extend far beyond the mouth, reducing risks for cardiovascular disease, diabetes, respiratory infections, cognitive decline, and numerous other chronic conditions. Research consistently shows that individuals who maintain excellent oral hygiene experience lower levels of systemic inflammation, improved immune function, and reduced healthcare costs compared to those who neglect oral health. The economic implications are equally compelling, with studies indicating that every dollar invested in preventive oral care saves $3-5 in future medical expenses related to systemic disease treatment. Healthcare providers increasingly recognize that oral health assessment should be integrated into comprehensive medical evaluations, as the mouth often provides early warning signs of developing systemic conditions. The ten evidence-based habits outlined in this article—when implemented consistently and comprehensively—create a powerful foundation for lifelong health that extends far beyond dental concerns. By embracing the mouth-body connection and prioritizing oral health as an integral component of overall wellness, individuals can take control of their health destiny while potentially preventing serious diseases that could otherwise compromise their quality of life and longevity.