12 Kidney Health Practices Worth Starting Before Any Symptoms Appear
Your kidneys work tirelessly around the clock, filtering approximately 50 gallons of blood daily while maintaining the delicate balance of fluids, electrolytes, and waste products in your body. These bean-shaped organs, each about the size of your fist, perform over 400 vital functions that keep you alive and healthy. Yet kidney disease often progresses silently for years, earning it the ominous nickname "the silent killer." By the time symptoms like fatigue, swelling, or changes in urination patterns appear, significant kidney damage may have already occurred. The sobering reality is that chronic kidney disease affects over 37 million Americans, with 90% unaware they have the condition. This stark statistic underscores the critical importance of proactive kidney care. The good news is that kidney health is largely within your control through lifestyle choices and preventive measures. The following twelve evidence-based practices represent a comprehensive approach to kidney wellness that can help preserve these vital organs' function for decades to come, potentially preventing the need for dialysis or transplantation while enhancing your overall quality of life.
1. Hydration Excellence - The Foundation of Kidney Function

Proper hydration serves as the cornerstone of optimal kidney health, yet many people chronically underestimate their fluid needs. Your kidneys require adequate water intake to effectively filter waste products, maintain blood pressure, and produce urine of appropriate concentration. Research published in the Journal of the American Society of Nephrology demonstrates that individuals who consume adequate water throughout the day show significantly better kidney function markers compared to those who remain chronically dehydrated. The general recommendation of eight glasses daily serves as a baseline, but your individual needs may vary based on climate, physical activity, body size, and overall health status. Quality matters as much as quantity – filtered water free from excessive minerals, chemicals, and contaminants reduces the burden on your kidneys. Morning hydration proves particularly crucial, as your body naturally becomes dehydrated overnight, causing your kidneys to work harder to concentrate waste products. Establishing a consistent hydration routine, such as drinking a glass of water upon waking and before each meal, helps maintain steady kidney function throughout the day. Additionally, monitoring your urine color provides valuable feedback – pale yellow indicates proper hydration, while dark yellow or amber suggests the need for increased fluid intake.
2. Blood Pressure Management - Protecting Your Kidney's Delicate Filters
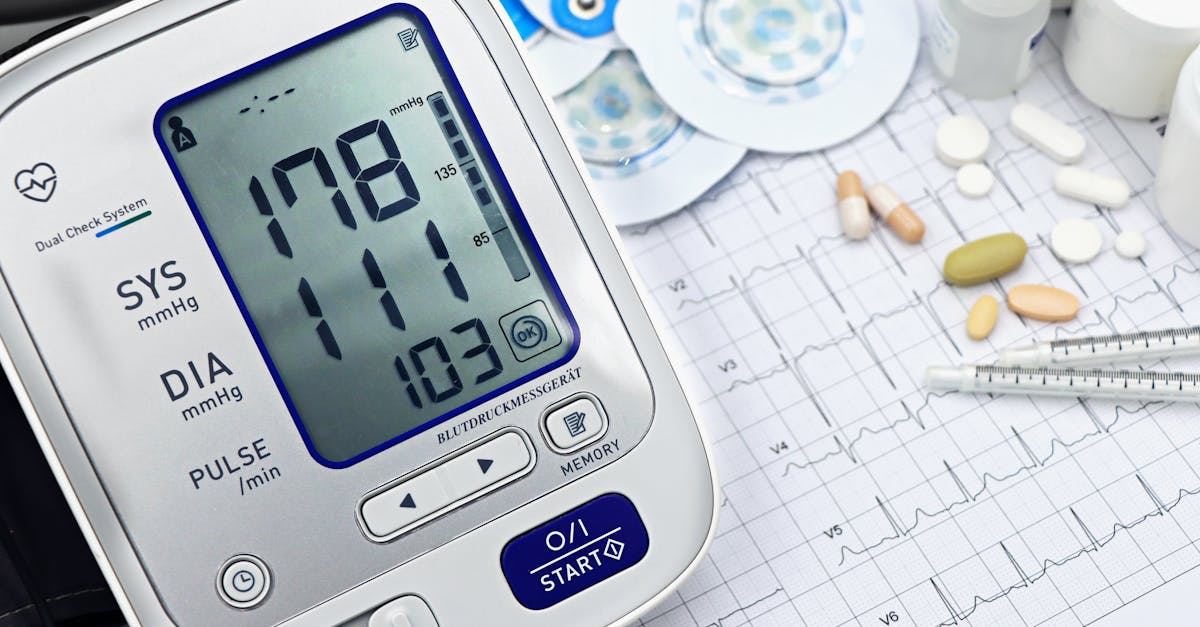
High blood pressure stands as one of the leading causes of kidney disease, creating a destructive cycle where elevated pressure damages the kidney's delicate filtering units called nephrons, which in turn makes blood pressure control more difficult. The kidneys contain millions of tiny blood vessels that can be irreversibly damaged by sustained high pressure, leading to scarring and reduced filtration capacity. Research from the National Kidney Foundation reveals that even slightly elevated blood pressure, previously considered "borderline," can cause significant kidney damage over time. Optimal blood pressure for kidney health targets below 130/80 mmHg, though some individuals may benefit from even lower targets. Regular monitoring becomes essential, as blood pressure can fluctuate throughout the day and may be influenced by factors such as stress, caffeine intake, and physical activity. Home blood pressure monitors provide valuable data for both you and your healthcare provider, enabling more precise management strategies. Lifestyle modifications including regular exercise, stress reduction techniques, adequate sleep, and dietary changes often prove remarkably effective in maintaining healthy blood pressure levels. When lifestyle changes alone prove insufficient, working closely with healthcare providers to find appropriate medications can prevent kidney damage while maintaining overall cardiovascular health.
3. Blood Sugar Optimization - Preventing Diabetic Kidney Disease
Diabetes represents the single most common cause of kidney failure, accounting for nearly half of all cases requiring dialysis or transplantation. Elevated blood glucose levels damage kidney blood vessels through a process called glycation, where sugar molecules attach to proteins and create harmful compounds that accumulate in kidney tissues. This damage occurs gradually and often without symptoms, making blood sugar management crucial even for individuals with prediabetes or occasional glucose elevations. The hemoglobin A1C test, which measures average blood sugar over three months, should ideally remain below 7% for most adults, though individual targets may vary based on age, health conditions, and life expectancy. Regular blood glucose monitoring, whether through traditional fingerstick testing or continuous glucose monitors, provides real-time feedback about how foods, exercise, stress, and medications affect your blood sugar levels. Dietary strategies focusing on complex carbohydrates, adequate protein, and healthy fats help maintain steady glucose levels throughout the day. Physical activity proves particularly powerful for blood sugar control, as muscle contractions increase glucose uptake independent of insulin. Even individuals without diabetes benefit from maintaining stable blood sugar levels, as frequent spikes and crashes can stress the kidneys and contribute to long-term damage. Understanding the glycemic impact of different foods empowers you to make kidney-friendly choices that support both current and future health.
4. Strategic Nutrition - Fueling Your Kidneys for Longevity

Nutritional choices profoundly impact kidney health, with certain foods providing protective benefits while others may accelerate damage when consumed excessively. A kidney-friendly diet emphasizes fresh, whole foods while limiting processed items high in sodium, phosphorus, and artificial additives that burden the kidneys' filtration system. Research published in the Clinical Journal of the American Society of Nephrology shows that individuals following Mediterranean-style eating patterns demonstrate significantly better kidney function preservation over time. This approach emphasizes colorful vegetables, fruits, whole grains, legumes, nuts, seeds, and moderate amounts of fish while limiting red meat and processed foods. Antioxidant-rich foods such as berries, leafy greens, and colorful vegetables help combat oxidative stress that can damage kidney tissues. Omega-3 fatty acids from sources like wild-caught fish, walnuts, and flaxseeds provide anti-inflammatory benefits that support kidney health. Portion control plays a crucial role, as excessive protein intake, particularly from animal sources, can strain the kidneys over time. However, adequate protein remains essential for maintaining muscle mass and overall health. The timing of meals also matters – eating regular, balanced meals helps maintain stable blood sugar and reduces metabolic stress on the kidneys. Staying informed about hidden sources of sodium and phosphorus in processed foods enables you to make choices that support long-term kidney function.
5. Sodium Reduction - Lightening the Load on Your Kidneys

Excessive sodium intake creates a cascade of problems for kidney health, forcing these organs to work harder to maintain proper fluid balance while contributing to high blood pressure and fluid retention. The average American consumes nearly twice the recommended daily sodium limit of 2,300 milligrams, with processed and restaurant foods contributing the majority of this excess. Your kidneys must filter all consumed sodium, and when intake exceeds the body's needs, the kidneys retain extra water to dilute the sodium concentration, leading to increased blood volume and elevated blood pressure. This additional workload can accelerate kidney damage over time, particularly in individuals with existing kidney disease or hypertension. Reading nutrition labels becomes essential, as sodium hides in unexpected places including bread, cereals, condiments, and canned vegetables. Fresh herbs, spices, citrus juices, and vinegars provide flavorful alternatives to salt while offering additional health benefits through their antioxidant and anti-inflammatory properties. Gradually reducing sodium intake allows your taste buds to adapt, making lower-sodium foods more appealing over time. Cooking at home provides the greatest control over sodium content, enabling you to create delicious, kidney-friendly meals. When dining out, requesting sauces and dressings on the side, choosing grilled over fried options, and asking about preparation methods helps minimize sodium exposure while maintaining social dining experiences.
6. Exercise Excellence - Moving Toward Better Kidney Health

Regular physical activity provides profound benefits for kidney health through multiple mechanisms, including improved blood pressure control, enhanced blood sugar regulation, weight management, and reduced inflammation throughout the body. Research from the American Journal of Kidney Diseases demonstrates that individuals who engage in regular moderate exercise show significantly slower rates of kidney function decline compared to sedentary individuals. Exercise enhances blood flow to the kidneys, promoting optimal filtration while helping maintain the health of kidney blood vessels. Both aerobic exercise and resistance training contribute unique benefits – cardiovascular exercise improves overall circulation and heart health, while strength training helps maintain muscle mass and metabolic health. The key lies in consistency rather than intensity; moderate activities such as brisk walking, swimming, cycling, or dancing for 150 minutes per week provide substantial kidney protection. High-intensity exercise, while beneficial for overall health, should be approached gradually and with adequate hydration to prevent acute kidney stress. Exercise also serves as a powerful stress reducer, helping manage cortisol levels that can impact kidney function when chronically elevated. For individuals with existing health conditions, working with healthcare providers or certified exercise professionals ensures safe, effective exercise programming. The psychological benefits of regular exercise, including improved mood and better sleep quality, create additional positive effects that support overall kidney health and well-being.
7. Weight Management - Reducing Kidney Burden Through Healthy Body Composition

Maintaining a healthy weight significantly reduces the risk of developing conditions that damage the kidneys, including diabetes, high blood pressure, and cardiovascular disease. Excess body weight, particularly abdominal fat, creates a state of chronic inflammation that can directly harm kidney tissues while increasing insulin resistance and blood pressure. Research published in the Journal of the American Medical Association shows that even modest weight loss of 5-10% can produce meaningful improvements in blood pressure, blood sugar control, and markers of kidney function. The kidneys must work harder to filter blood in individuals with larger body mass, and obesity-related conditions such as sleep apnea can further stress these vital organs. Sustainable weight management focuses on gradual changes rather than extreme measures that might actually harm kidney function. Crash diets, excessive protein intake, and dehydration associated with rapid weight loss can place additional stress on the kidneys. Instead, a balanced approach combining appropriate caloric intake with regular physical activity and adequate hydration supports both weight management and kidney health. Understanding the difference between healthy weight loss (1-2 pounds per week) and potentially harmful rapid weight loss helps protect kidney function while achieving body composition goals. Working with registered dietitians or healthcare providers ensures that weight management strategies align with kidney health objectives while meeting individual nutritional needs and preferences.
8. Sleep Quality - The Overnight Kidney Restoration Period

Quality sleep plays a crucial yet often overlooked role in kidney health, as these organs follow circadian rhythms that influence blood pressure, hormone production, and filtration rates. During sleep, blood pressure naturally decreases, giving the kidneys a period of reduced workload that allows for cellular repair and regeneration. Research from the National Sleep Foundation indicates that individuals who consistently get 7-9 hours of quality sleep show better kidney function markers compared to those with chronic sleep deprivation. Poor sleep quality contributes to elevated blood pressure, increased stress hormones, and impaired glucose metabolism – all factors that can damage kidney function over time. Sleep apnea, a condition where breathing repeatedly stops during sleep, creates particular risks for kidney health through intermittent oxygen deprivation and blood pressure spikes. Establishing consistent sleep hygiene practices, including regular bedtimes, comfortable sleep environments, and limiting screen exposure before bed, supports both sleep quality and kidney function. The timing of fluid intake also matters for kidney health – consuming most daily fluids earlier in the day and reducing intake 2-3 hours before bedtime helps prevent sleep disruption while ensuring adequate hydration. Chronic insomnia or sleep disorders warrant medical evaluation, as treating these conditions can provide significant benefits for kidney health. Creating a sleep-friendly environment with appropriate temperature, darkness, and noise control supports the natural restoration processes that occur during quality sleep.
9. Stress Management - Protecting Kidneys from Chronic Tension

Chronic stress creates a complex web of physiological changes that can significantly impact kidney health through elevated cortisol levels, increased blood pressure, and inflammatory responses throughout the body. When stress becomes chronic, the body's fight-or-flight response remains constantly activated, leading to sustained elevation in stress hormones that can damage kidney blood vessels and impair filtration function. Research published in the American Journal of Nephrology demonstrates that individuals with high chronic stress levels show accelerated decline in kidney function compared to those with effective stress management strategies. Stress also influences behaviors that affect kidney health, including poor dietary choices, inadequate sleep, reduced physical activity, and increased alcohol or tobacco use. Developing effective stress management techniques becomes essential for kidney protection, with options including meditation, deep breathing exercises, yoga, tai chi, and regular physical activity. The practice of mindfulness, whether through formal meditation or simply paying attention to present-moment experiences, helps reduce the physiological stress response while improving overall well-being. Social connections and strong support systems provide additional stress-buffering effects that benefit kidney health. Time management strategies, setting realistic expectations, and learning to say no to excessive commitments help prevent stress accumulation. Professional counseling or therapy can provide valuable tools for managing chronic stress, particularly when combined with lifestyle modifications that support both mental health and kidney function.
10. Toxin Avoidance - Minimizing Kidney Exposure to Harmful Substances

Your kidneys serve as the body's primary filtration system, making them particularly vulnerable to damage from environmental toxins, medications, and other harmful substances that accumulate over time. Common household and workplace chemicals, including cleaning products, pesticides, heavy metals, and industrial solvents, can cause both acute and chronic kidney damage when exposure levels exceed the body's ability to safely process and eliminate these substances. Research from Environmental Health Perspectives shows that individuals with higher exposure to certain environmental toxins demonstrate increased rates of kidney disease development. Over-the-counter medications, particularly nonsteroidal anti-inflammatory drugs (NSAIDs) like ibuprofen and naproxen, can cause kidney damage when used frequently or in high doses, especially in individuals who are dehydrated or have existing kidney problems. Reading medication labels carefully and following dosing instructions helps prevent medication-induced kidney injury. Choosing organic produce when possible reduces exposure to pesticide residues, while using natural cleaning products minimizes household chemical exposure. Proper ventilation when using chemicals, wearing protective equipment when necessary, and following safety guidelines for workplace exposures help protect kidney function. Water filtration systems can reduce exposure to chlorine, heavy metals, and other contaminants that may stress the kidneys over time. Being aware of potential kidney toxins in personal care products, including certain hair dyes and cosmetics, enables informed choices that support long-term kidney health.
11. Regular Health Monitoring - Early Detection for Optimal Outcomes
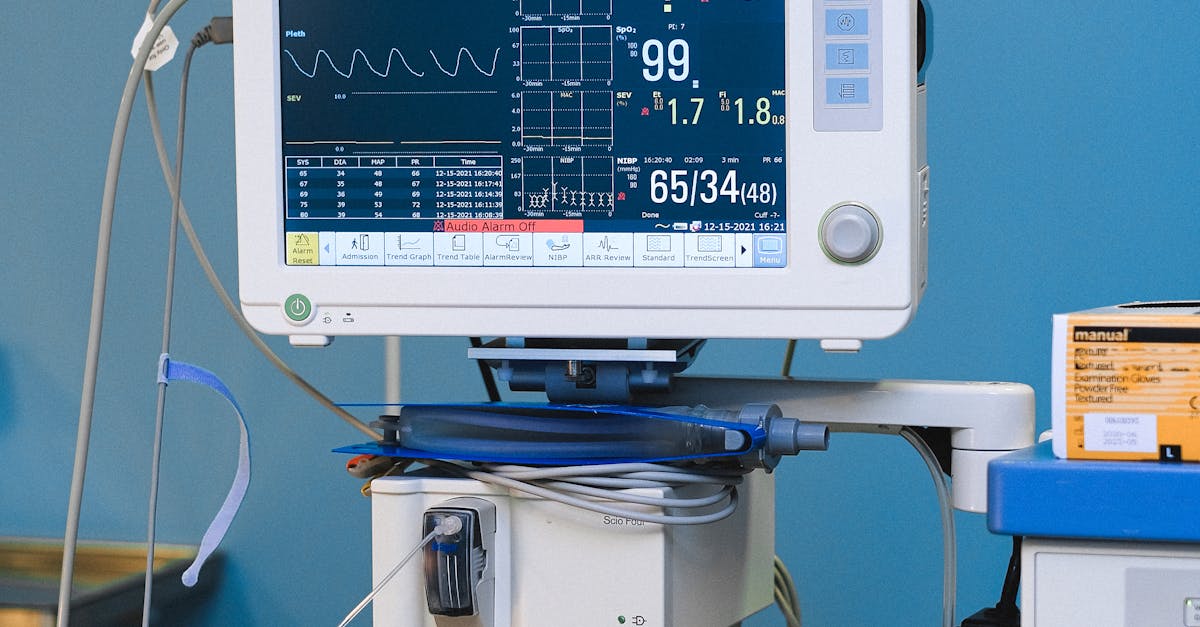
Proactive health monitoring provides the foundation for early detection of kidney problems, enabling intervention before irreversible damage occurs. Regular check-ups with healthcare providers should include specific tests that assess kidney function, including serum creatinine, blood urea nitrogen (BUN), estimated glomerular filtration rate (eGFR), and urinalysis to detect protein or blood in the urine. These tests can reveal kidney problems years before symptoms develop, providing crucial time for protective interventions. The frequency of testing depends on individual risk factors – those with diabetes, high blood pressure, family history of kidney disease, or other risk factors may need more frequent monitoring than healthy individuals with no risk factors. Understanding your test results empowers you to take an active role in kidney health management, with eGFR values above 90 indicating normal function, while values below 60 suggest chronic kidney disease. Home monitoring tools, including blood pressure cuffs and glucose meters for those at risk, provide valuable data between medical visits. Keeping detailed records of test results, medications, and symptoms helps healthcare providers track changes over time and adjust treatment strategies accordingly. Annual comprehensive metabolic panels should be considered standard care for adults over 40 or those with risk factors, regardless of symptoms. Building a strong relationship with healthcare providers who understand your health goals and concerns ensures that kidney health remains a priority in your overall healthcare plan.
12. Supplement Wisdom - Supporting Kidneys Through Targeted Nutrition

While a balanced diet provides the foundation for kidney health, certain supplements may offer additional protective benefits when used appropriately and under professional guidance. Research suggests that specific nutrients, including omega-3 fatty acids, vitamin D, and certain antioxidants, may help protect kidney function and slow the progression of kidney disease. However, the supplement industry remains largely unregulated, making quality and dosing inconsistent across products. Some supplements can actually harm kidney function, particularly in high doses or when combined with certain medications. Vitamin C supplements exceeding 1000mg daily can increase oxalate production, potentially contributing to kidney stone formation in susceptible individuals. Herbal supplements, while natural, can interact with medications and may contain compounds that stress the kidneys. Working with healthcare providers or registered dietitians helps identify which supplements might benefit your individual situation while avoiding potentially harmful interactions. High-quality fish oil supplements providing EPA and DHA omega-3 fatty acids show promise for reducing inflammation and supporting kidney health, particularly in individuals with diabetes or cardiovascular disease. Vitamin D deficiency, common in individuals with kidney disease, may warrant supplementation under medical supervision. Probiotics may support kidney health by reducing uremic toxins and supporting overall metabolic health. The key principle remains that supplements should supplement, not replace, a healthy diet and lifestyle, and any supplementation strategy should be developed in partnership with qualified healthcare professionals.
13. Building Your Kidney Health Action Plan - Sustainable Implementation Strategies

Creating lasting change in kidney health requires a systematic approach that transforms knowledge into sustainable daily practices. Begin by assessing your current habits and identifying the areas where you have the greatest opportunity for improvement, whether that's increasing water intake, reducing sodium consumption, or establishing a regular exercise routine. Research from behavioral psychology demonstrates that focusing on one or two changes at a time increases the likelihood of long-term success compared to attempting multiple simultaneous changes. Start with the practices that feel most achievable and gradually build upon your successes. Creating specific, measurable goals helps track progress – for example, "I will drink 8 glasses of water daily" rather than "I will drink more water." Environmental modifications, such as keeping a water bottle visible, preparing healthy snacks in advance, or scheduling exercise like appointments, support behavior change by reducing barriers to healthy choices. Tracking tools, whether simple journals, smartphone apps, or wearable devices, provide valuable feedback and motivation. Building accountability through family members, friends, or healthcare providers increases adherence to healthy practices. Regular reassessment and adjustment of your action plan ensures that it remains relevant and achievable as your life circumstances change. Remember that kidney health is a long-term investment,