10 Autoimmune Conditions That Are Frequently Misdiagnosed
2. Hashimoto's Thyroiditis - The Silent Saboteur of Metabolism
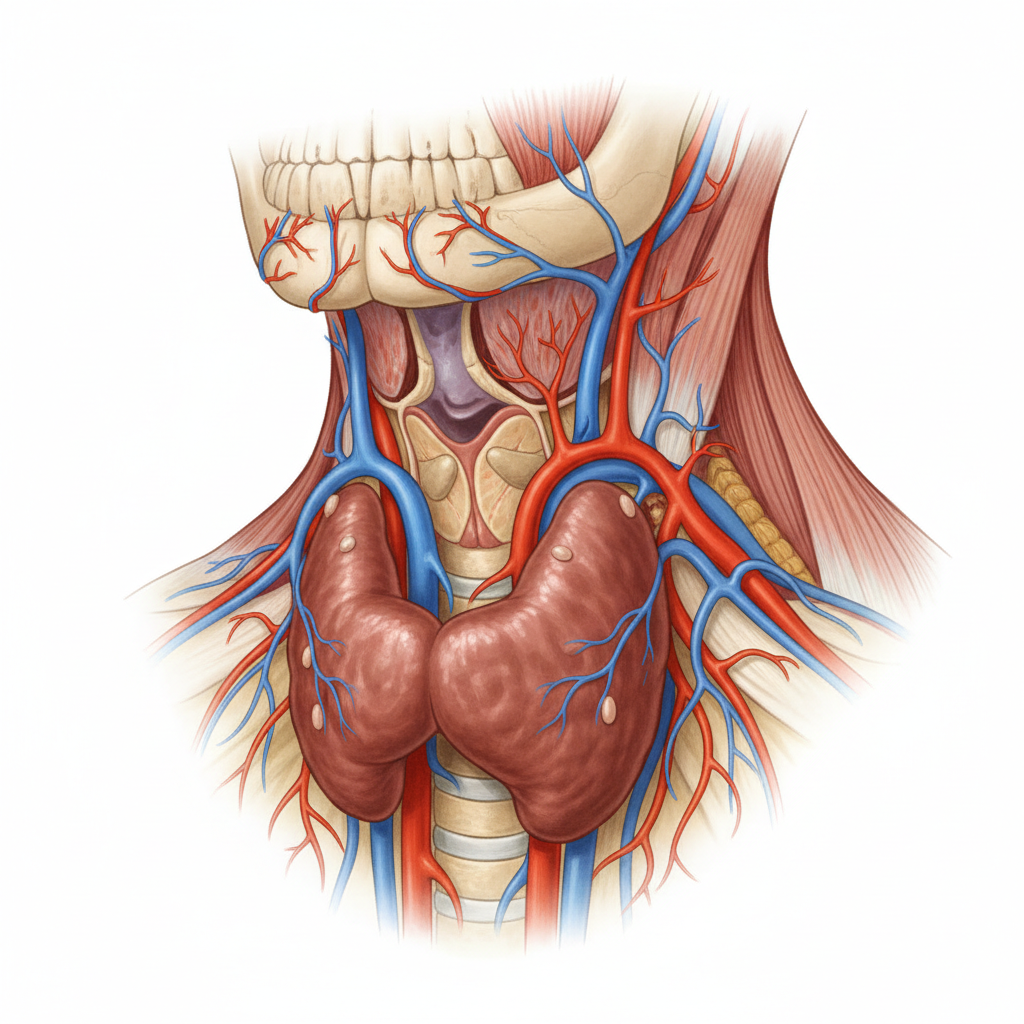
Hashimoto's thyroiditis, the most common cause of hypothyroidism in developed countries, exemplifies how autoimmune conditions can lurk beneath the surface for years before being properly identified. This condition occurs when the immune system gradually destroys thyroid tissue, leading to a progressive decline in thyroid hormone production that can profoundly impact every system in the body. The insidious nature of Hashimoto's makes it particularly prone to misdiagnosis, as symptoms develop slowly and are often attributed to aging, stress, depression, or lifestyle factors. Patients frequently present with complaints of unexplained weight gain, persistent fatigue, brain fog, hair loss, and cold intolerance – symptoms that are easily dismissed or attributed to other causes. Many healthcare providers rely solely on thyroid-stimulating hormone (TSH) levels for diagnosis, potentially missing cases where TSH remains normal despite significant thyroid antibody elevation and tissue destruction. The condition is often misdiagnosed as depression, chronic fatigue syndrome, or menopause-related changes, particularly in women over 40. Subclinical hypothyroidism, where TSH is mildly elevated but thyroid hormones remain within normal ranges, represents a diagnostic gray area where patients experience symptoms but may not receive treatment. The presence of thyroid peroxidase (TPO) and thyroglobulin antibodies confirms the autoimmune nature of the condition, yet these tests are not always ordered during initial evaluations. Early detection and treatment with thyroid hormone replacement can prevent progression to overt hypothyroidism and associated complications including cardiovascular disease, cognitive decline, and reproductive issues.