12 Types of Arthritis and How They Differ
9. Infectious Arthritis - When Microbes Attack Joints
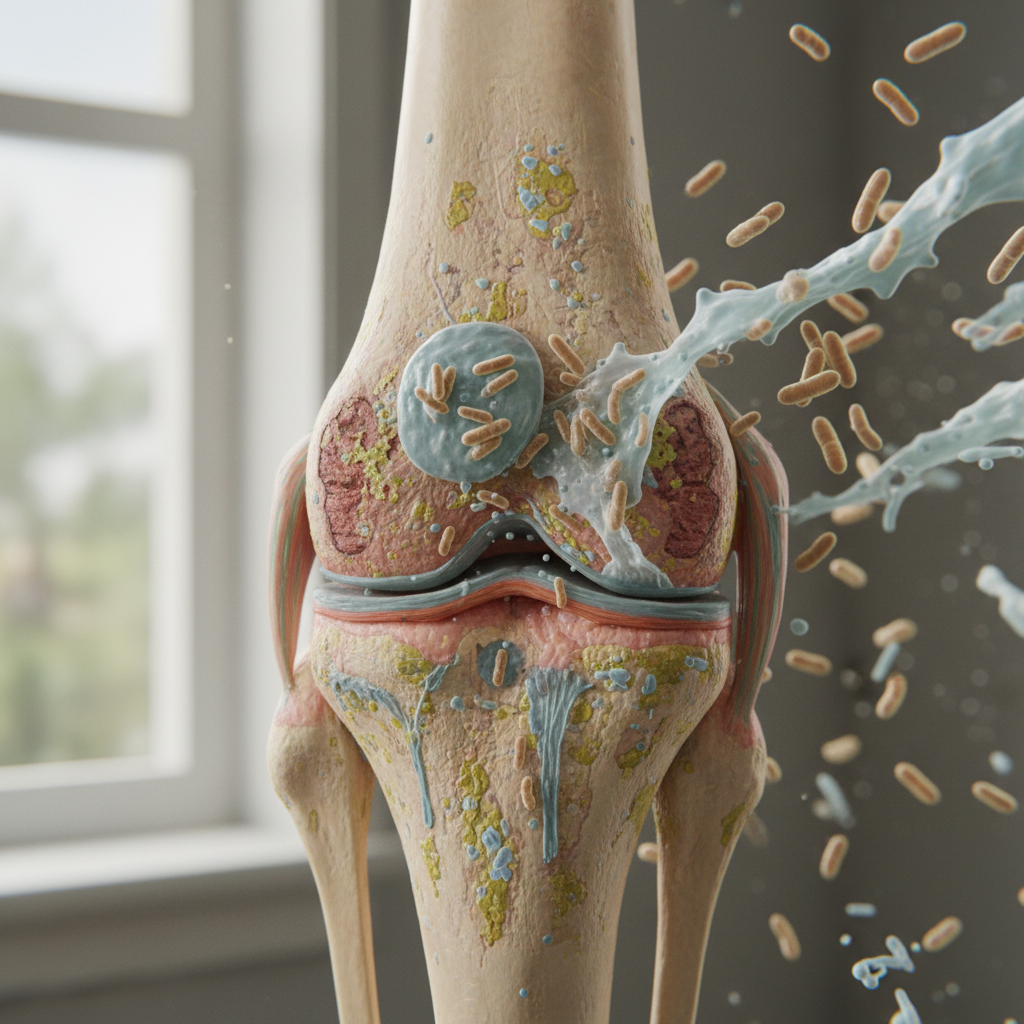
Infectious arthritis, also known as septic arthritis, occurs when bacteria, viruses, fungi, or other microorganisms directly invade joint spaces, causing acute inflammation and potentially devastating joint destruction if not promptly treated. Bacterial arthritis represents a medical emergency, with Staphylococcus aureus being the most common causative organism in adults, while Streptococcus species and gram-negative bacteria are also frequently implicated. The condition typically affects a single joint, most commonly the knee, followed by the hip, ankle, and shoulder, though polyarticular involvement can occur, particularly in immunocompromised patients or those with underlying rheumatoid arthritis. Patients present with acute onset of severe joint pain, swelling, warmth, and restricted movement, often accompanied by systemic symptoms such as fever, chills, and malaise. Risk factors include advanced age, immunosuppression, diabetes, chronic kidney disease, intravenous drug use, recent joint surgery or injection, and pre-existing joint disease. Prompt diagnosis requires immediate arthrocentesis with synovial fluid analysis showing elevated white blood cell counts (typically >50,000 cells/μL with >90% neutrophils), low glucose levels, and positive cultures when possible. Treatment involves immediate drainage of infected synovial fluid through repeated aspirations or surgical intervention, combined with appropriate antimicrobial therapy based on culture results and sensitivity patterns. Delayed treatment can result in irreversible joint damage, osteomyelitis, and systemic sepsis, making early recognition and aggressive management crucial for optimal outcomes.