12 Types of Arthritis and How They Differ
Arthritis, derived from the Greek words "arthro" meaning joint and "itis" meaning inflammation, represents a complex family of musculoskeletal disorders that affects over 54 million adults in the United States alone. Far from being a single disease, arthritis encompasses more than 100 different conditions that cause pain, swelling, and reduced motion in joints and surrounding tissues. While many people associate arthritis exclusively with aging, this misconception overlooks the diverse nature of these conditions, which can affect individuals of all ages, from infants to elderly adults. The various types of arthritis differ significantly in their underlying causes, affected body parts, progression patterns, and treatment approaches. Some forms result from autoimmune processes where the body's immune system mistakenly attacks healthy tissues, while others stem from wear and tear, infections, or metabolic disorders. Understanding these distinctions is crucial for proper diagnosis and treatment, as what works for one type of arthritis may be ineffective or even harmful for another. This comprehensive exploration will examine twelve major types of arthritis, delving into their unique characteristics, symptoms, and management strategies to provide a clear understanding of how these conditions differ and why personalized treatment approaches are essential.
1. Osteoarthritis - The Wear and Tear Disease

Osteoarthritis stands as the most prevalent form of arthritis, affecting over 32.5 million adults in the United States and representing the leading cause of disability worldwide. Often referred to as "wear and tear" arthritis, osteoarthritis occurs when the protective cartilage that cushions the ends of bones gradually wears down over time. This degenerative joint disease primarily affects weight-bearing joints such as the knees, hips, and spine, though it can also impact the hands, particularly the finger joints closest to the fingernails. Unlike inflammatory forms of arthritis, osteoarthritis is characterized by mechanical damage rather than systemic inflammation, though some inflammatory processes do occur locally within affected joints. The condition typically develops slowly over years or decades, with symptoms including joint pain that worsens with activity, stiffness after periods of inactivity, reduced range of motion, and the formation of bone spurs around affected joints. Risk factors include advancing age, obesity, previous joint injuries, repetitive stress on joints from occupational or recreational activities, and genetic predisposition. The hallmark of osteoarthritis on X-rays includes joint space narrowing, osteophyte formation, and subchondral bone changes, distinguishing it from inflammatory arthritis types that may show different radiographic patterns.
2. Rheumatoid Arthritis - The Autoimmune Assault
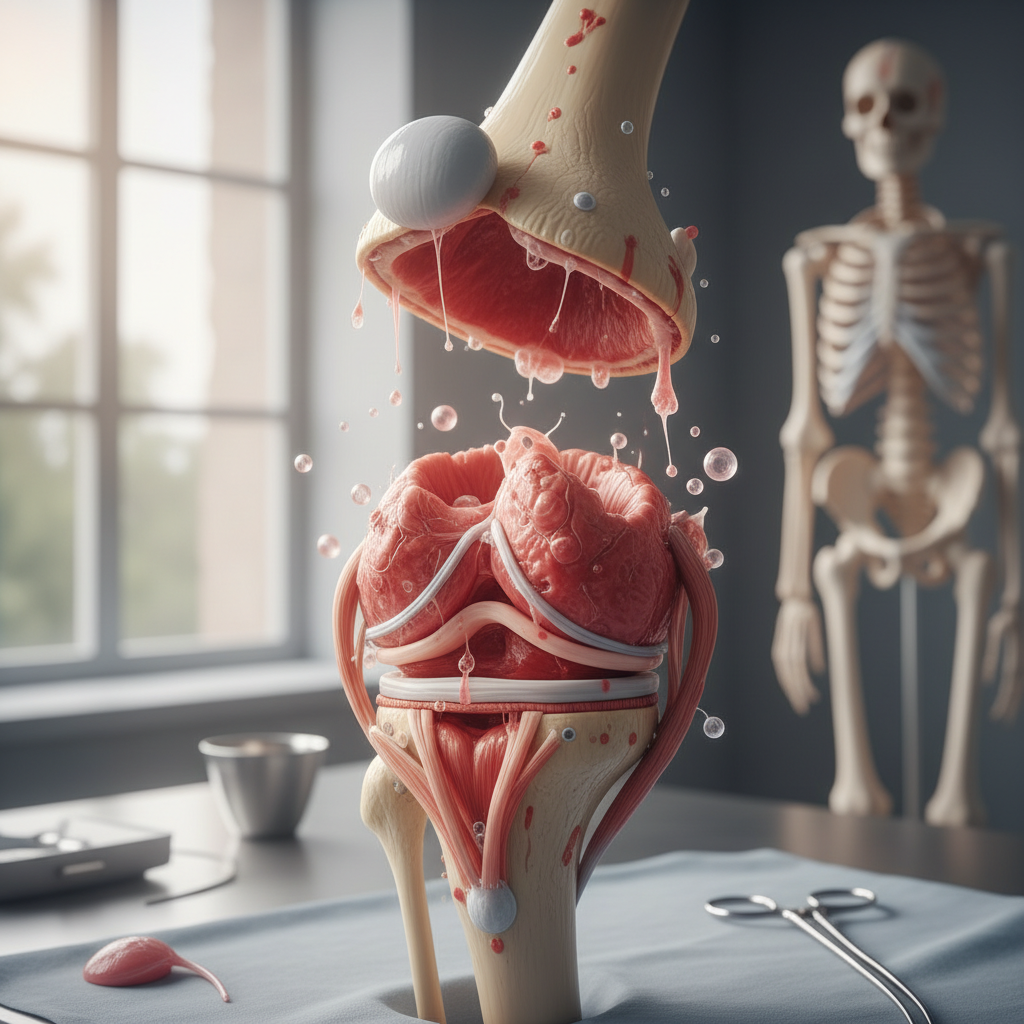
Rheumatoid arthritis represents a chronic, systemic autoimmune disorder that affects approximately 1.3 million Americans, with women being three times more likely to develop the condition than men. Unlike osteoarthritis, rheumatoid arthritis occurs when the immune system mistakenly attacks the synovium, the thin membrane that lines the joints, causing inflammation that can eventually destroy cartilage and bone. This condition typically affects joints symmetrically, meaning if one knee or hand is affected, the other usually is as well, and commonly targets smaller joints first, such as those in the hands and feet, before progressing to larger joints. The inflammatory nature of rheumatoid arthritis means that patients often experience systemic symptoms beyond joint pain, including fatigue, low-grade fever, loss of appetite, and morning stiffness that can last for hours. Laboratory tests reveal elevated inflammatory markers such as C-reactive protein and erythrocyte sedimentation rate, along with specific antibodies like rheumatoid factor and anti-cyclic citrullinated peptide antibodies. Early diagnosis and aggressive treatment with disease-modifying antirheumatic drugs (DMARDs) are crucial, as the condition can cause irreversible joint damage within the first two years if left untreated. The chronic inflammation associated with rheumatoid arthritis also increases the risk of cardiovascular disease, osteoporosis, and other systemic complications.
3. Psoriatic Arthritis - When Skin and Joints Collide
Psoriatic arthritis affects approximately 30% of individuals with psoriasis, a chronic skin condition characterized by red, scaly patches, though joint symptoms can sometimes precede skin manifestations. This inflammatory arthritis belongs to a group called spondyloarthropathies and presents unique challenges due to its diverse clinical presentations and potential for affecting multiple body systems. Unlike rheumatoid arthritis, psoriatic arthritis often affects joints asymmetrically and can involve the spine, causing inflammation in the sacroiliac joints and vertebrae. The condition is characterized by five distinct patterns: asymmetric oligoarticular (affecting few joints), symmetric polyarticular (similar to rheumatoid arthritis), distal interphalangeal joint involvement, arthritis mutilans (a severe, deforming type), and spondylitis (spinal involvement). Patients frequently experience enthesitis, inflammation at the sites where tendons and ligaments attach to bones, particularly affecting the Achilles tendon and plantar fascia. Dactylitis, or "sausage digits," represents another hallmark feature where entire fingers or toes become swollen and painful. The presence of nail changes, including pitting, ridging, and separation from the nail bed, often provides important diagnostic clues. Treatment typically involves a combination of medications targeting both skin and joint symptoms, including methotrexate, biologics, and targeted synthetic DMARDs.
4. Ankylosing Spondylitis - The Spine's Silent Stiffener
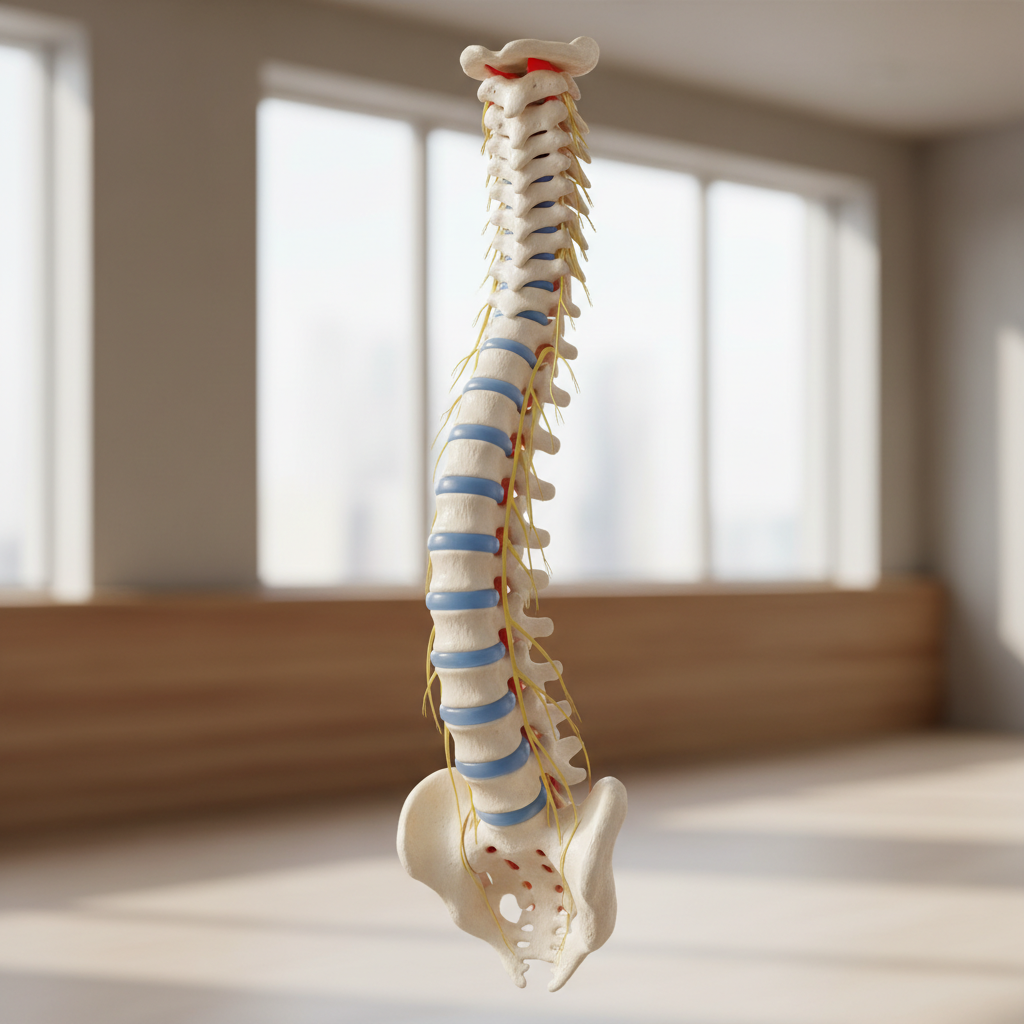
Ankylosing spondylitis primarily affects the spine and sacroiliac joints, causing inflammation that can eventually lead to fusion of vertebrae and significant spinal rigidity. This chronic inflammatory condition typically begins in early adulthood, with men being affected more frequently than women, though recent research suggests the gender gap may be narrower than previously thought. The hallmark symptom is inflammatory back pain that improves with exercise and worsens with rest, often causing patients to wake up in the early morning hours due to stiffness and discomfort. Unlike mechanical back pain from injury or degenerative changes, ankylosing spondylitis pain is typically worse in the morning and after periods of inactivity, improving throughout the day with movement. The condition has a strong genetic component, with over 90% of patients carrying the HLA-B27 gene, though having this gene doesn't guarantee development of the disease. As the condition progresses, inflammation can cause the formation of syndesmophytes, bony growths that bridge vertebrae, potentially leading to a completely fused spine known as "bamboo spine." Extra-articular manifestations include acute anterior uveitis (eye inflammation), inflammatory bowel disease, and cardiovascular complications. Early diagnosis and treatment with anti-TNF biologics or IL-17 inhibitors can significantly slow disease progression and maintain spinal mobility, emphasizing the importance of recognizing symptoms in young adults with chronic back pain.
5. Gout - The Crystal Clear Culprit
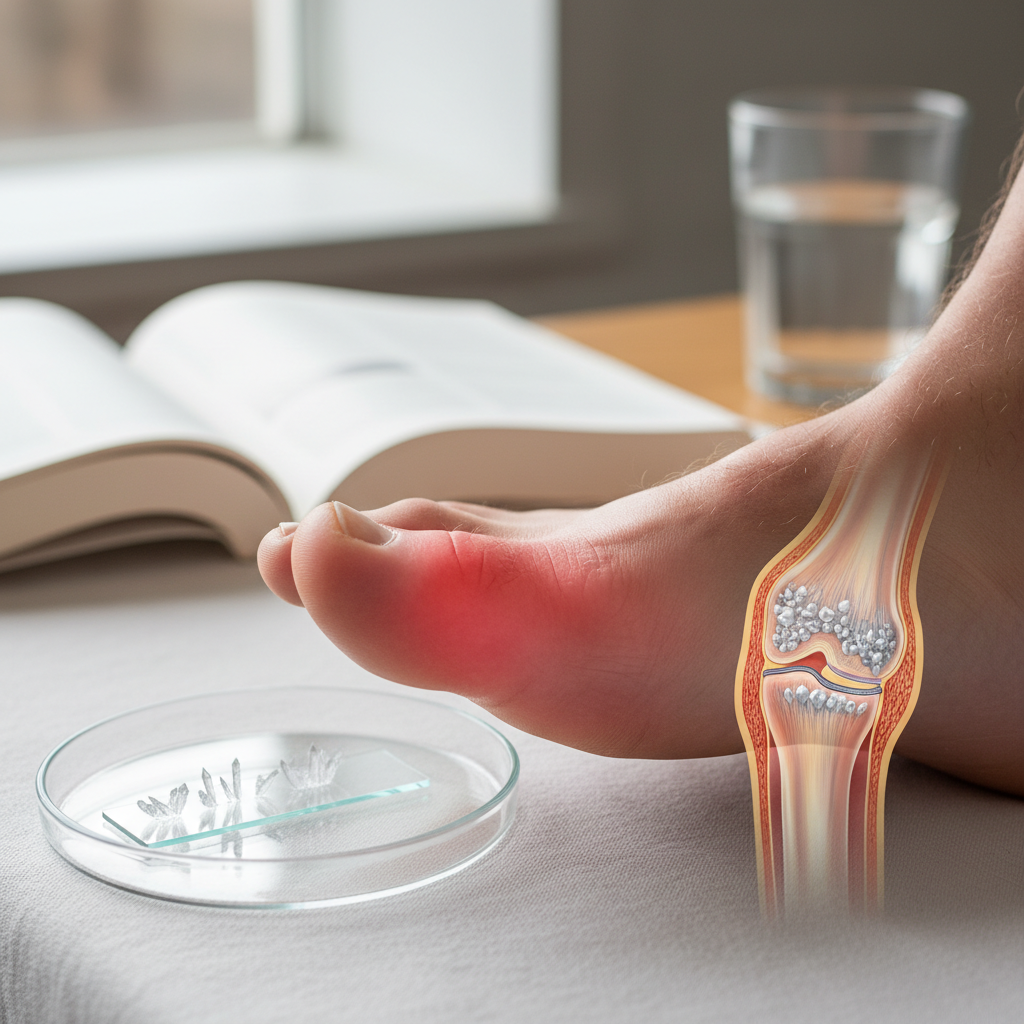
Gout represents a unique form of inflammatory arthritis caused by the deposition of uric acid crystals in joints and surrounding tissues, creating one of the most acutely painful arthritis experiences known to medicine. This metabolic disorder affects approximately 4% of adults in the United States, with men being four times more likely to develop the condition than premenopausal women, though the risk equalizes after menopause. The classic presentation involves sudden onset of severe pain, typically in the big toe (a condition called podagra), though gout can affect any joint, including the ankle, knee, wrist, and fingers. Attacks often occur at night and can be triggered by dietary factors such as red meat, shellfish, alcohol (particularly beer), and foods high in purines, as well as dehydration, stress, or certain medications. The affected joint becomes exquisitely tender, swollen, red, and warm, with pain so severe that even the weight of bed sheets can be unbearable. Chronic gout can lead to the formation of tophi, chalky deposits of uric acid crystals that appear as lumps under the skin around joints, ears, or other areas. Diagnosis is confirmed through synovial fluid analysis revealing needle-shaped, negatively birefringent uric acid crystals under polarized light microscopy. Management involves both acute treatment with anti-inflammatory medications and long-term uric acid-lowering therapy to prevent future attacks and complications.
6. Lupus Arthritis - The Great Imitator's Joint Manifestation

Systemic lupus erythematosus (SLE) affects multiple organ systems, with arthritis being one of the most common manifestations, occurring in approximately 90% of patients with this autoimmune condition. Lupus arthritis typically presents as a non-erosive, symmetric polyarthritis that primarily affects the small joints of the hands, wrists, and knees, though it can involve virtually any joint in the body. Unlike rheumatoid arthritis, lupus arthritis rarely causes permanent joint deformity or bone erosion, though it can lead to reversible joint deformities such as swan neck deformities of the fingers due to ligament laxity. The arthritis associated with lupus is often accompanied by other systemic manifestations including the characteristic butterfly rash across the cheeks and nose bridge, photosensitivity, oral ulcers, kidney involvement, and neurological symptoms. Morning stiffness is common but typically shorter in duration compared to rheumatoid arthritis, usually lasting less than an hour. Laboratory findings include positive antinuclear antibodies (ANA), anti-double-stranded DNA antibodies, and complement consumption, which help distinguish lupus from other forms of inflammatory arthritis. The unpredictable nature of lupus means that arthritis symptoms can flare and remit, often correlating with overall disease activity. Treatment focuses on controlling systemic inflammation with antimalarials like hydroxychloroquine, corticosteroids during flares, and immunosuppressive agents for severe cases, while avoiding medications that might trigger lupus flares.
7. Juvenile Idiopathic Arthritis - When Childhood Meets Chronic Disease

Juvenile idiopathic arthritis (JIA) encompasses a group of chronic arthritis conditions that begin before age 16 and persist for at least six weeks, affecting approximately 300,000 children in the United States. This complex group of disorders is classified into several subtypes based on the number of joints affected, presence of systemic symptoms, and specific clinical features. Oligoarticular JIA affects four or fewer joints in the first six months and is the most common subtype, particularly in young girls, often affecting large joints like knees and ankles. Polyarticular JIA involves five or more joints and can be either rheumatoid factor positive or negative, with the positive form more closely resembling adult rheumatoid arthritis. Systemic JIA presents with high spiking fevers, salmon-colored rash, lymphadenopathy, and hepatosplenomegaly in addition to arthritis, representing the most severe form. Enthesitis-related arthritis primarily affects boys and involves inflammation at tendon and ligament attachment sites, often progressing to involve the spine. Psoriatic JIA combines features of arthritis with psoriasis or a family history of the skin condition. Early diagnosis and treatment are crucial to prevent growth disturbances, joint contractures, and vision-threatening complications such as chronic anterior uveitis. Treatment approaches must consider the child's growth and development, often involving a multidisciplinary team including pediatric rheumatologists, ophthalmologists, physical therapists, and psychologists.
8. Fibromyalgia - The Widespread Pain Syndrome

Fibromyalgia represents a chronic pain disorder characterized by widespread musculoskeletal pain, fatigue, and tender points throughout the body, affecting an estimated 2-4% of the population, with women being affected seven times more frequently than men. While not technically a form of arthritis since it doesn't involve joint inflammation or damage, fibromyalgia is often confused with arthritis due to its widespread pain and is frequently seen in conjunction with various arthritis conditions. The condition is characterized by abnormal pain processing in the central nervous system, leading to amplified pain signals and reduced pain thresholds. Patients typically experience pain in all four quadrants of the body for at least three months, accompanied by fatigue, sleep disturbances, cognitive difficulties often referred to as "fibro fog," and mood disorders such as depression and anxiety. The 2010 American College of Rheumatology criteria for fibromyalgia diagnosis include a widespread pain index and symptom severity scale, moving away from the previous tender point examination. Unlike inflammatory arthritis, fibromyalgia doesn't cause joint swelling, deformity, or laboratory abnormalities, and imaging studies appear normal. The condition often coexists with other chronic pain conditions, autoimmune diseases, and psychiatric disorders, suggesting shared pathophysiological mechanisms. Treatment focuses on a multimodal approach including medications that modulate pain processing (such as pregabalin, duloxetine, and milnacipran), regular exercise, stress management, and cognitive behavioral therapy.
9. Infectious Arthritis - When Microbes Attack Joints
Infectious arthritis, also known as septic arthritis, occurs when bacteria, viruses, fungi, or other microorganisms directly invade joint spaces, causing acute inflammation and potentially devastating joint destruction if not promptly treated. Bacterial arthritis represents a medical emergency, with Staphylococcus aureus being the most common causative organism in adults, while Streptococcus species and gram-negative bacteria are also frequently implicated. The condition typically affects a single joint, most commonly the knee, followed by the hip, ankle, and shoulder, though polyarticular involvement can occur, particularly in immunocompromised patients or those with underlying rheumatoid arthritis. Patients present with acute onset of severe joint pain, swelling, warmth, and restricted movement, often accompanied by systemic symptoms such as fever, chills, and malaise. Risk factors include advanced age, immunosuppression, diabetes, chronic kidney disease, intravenous drug use, recent joint surgery or injection, and pre-existing joint disease. Prompt diagnosis requires immediate arthrocentesis with synovial fluid analysis showing elevated white blood cell counts (typically >50,000 cells/μL with >90% neutrophils), low glucose levels, and positive cultures when possible. Treatment involves immediate drainage of infected synovial fluid through repeated aspirations or surgical intervention, combined with appropriate antimicrobial therapy based on culture results and sensitivity patterns. Delayed treatment can result in irreversible joint damage, osteomyelitis, and systemic sepsis, making early recognition and aggressive management crucial for optimal outcomes.
10. Reactive Arthritis - The Post-Infectious Response

Reactive arthritis, formerly known as Reiter's syndrome, represents a sterile inflammatory arthritis that develops following certain bacterial infections, typically involving the genitourinary or gastrointestinal tract. This condition affects approximately 1-3% of individuals following triggering infections with organisms such as Chlamydia trachomatis, Salmonella, Shigella, Campylobacter, or Yersinia species. The arthritis typically develops 1-4 weeks after the initial infection and predominantly affects lower extremity joints in an asymmetric pattern, commonly involving the knees, ankles, and feet. The classic triad includes arthritis, urethritis, and conjunctivitis, though complete triad presentation occurs in only about 30% of patients. Additional features may include enthesitis, dactylitis, inflammatory back pain, and characteristic skin lesions such as keratoderma blennorrhagicum on the palms and soles. Like other spondyloarthropathies, reactive arthritis shows a strong association with HLA-B27, present in 60-80% of patients, which may influence disease severity and chronicity. The condition is typically self-limiting, resolving within 6-12 months, though some patients develop chronic arthritis or recurrent episodes. Diagnosis relies primarily on clinical presentation and history of preceding infection, as there are no specific laboratory tests, though elevated inflammatory markers and HLA-B27 testing may provide supportive evidence. Treatment focuses on symptomatic relief with NSAIDs and, in severe or chronic cases, disease-modifying antirheumatic drugs such as sulfasalazine or methotrexate.
11. Polymyalgia Rheumatica - The Great Stiffness

Polymyalgia rheumatica represents an inflammatory condition that primarily affects adults over 50 years of age, characterized by severe muscle pain and stiffness in the neck, shoulders, and hips, often accompanied by constitutional symptoms such as fatigue, low-grade fever, and weight loss. This condition has a strong predilection for individuals of Northern European descent and shows a clear female predominance, with women being affected twice as often as men. The hallmark symptom is profound morning stiffness lasting more than one hour, particularly affecting the shoulder and hip girdles, making simple activities like getting out of bed, combing hair, or putting on clothes extremely difficult. Unlike true arthritis, polymyalgia rheumatica primarily affects muscles and surrounding soft tissues rather than joints themselves, though some patients may experience mild joint swelling. The condition is closely associated with giant cell arteritis (temporal arteritis), with approximately 15-20% of polymyalgia rheumatica patients developing this serious vasculitic complication that can lead to blindness if untreated. Laboratory findings typically show markedly elevated inflammatory markers, with erythrocyte sedimentation rates often exceeding 50 mm/hour and elevated C-reactive protein levels. The diagnosis is largely clinical, supported by laboratory findings and dramatic response to low-dose corticosteroids, which often provide relief within days of initiation. Treatment typically involves prednisone starting at 15-20 mg daily, with gradual tapering over 1-2 years, though some patients require longer treatment periods or steroid-sparing agents such as methotrexate.