10 Annual Health Checks Men Most Commonly Skip and Why They Matter
Men's relationship with healthcare is paradoxical and deeply concerning. While women are 33% more likely to visit a doctor annually, men consistently postpone, avoid, or entirely skip crucial health screenings that could prevent serious medical conditions or detect them in their earliest, most treatable stages. This avoidance stems from a complex web of cultural conditioning, societal expectations of masculine stoicism, fear of vulnerability, and the dangerous misconception that seeking medical care is a sign of weakness. The statistics paint a sobering picture: men are 24% less likely than women to have visited a doctor within the past year, and they're significantly more prone to dying from preventable diseases. This systematic neglect of preventive healthcare doesn't just impact individual men—it creates ripple effects throughout families and communities, leading to premature deaths, increased healthcare costs, and unnecessary suffering. The ten essential health screenings that men most commonly skip represent critical opportunities for early intervention, yet cultural barriers and personal resistance continue to create dangerous gaps in men's healthcare. Understanding why these screenings matter and addressing the underlying reasons for avoidance is essential for improving men's health outcomes and longevity.
1. Prostate Cancer Screening - The Most Avoided Yet Critical Test
Prostate cancer screening represents perhaps the most significant gap in men's preventive healthcare, with nearly 40% of men over 50 avoiding this crucial examination despite prostate cancer being the second leading cause of cancer death among American men. The reluctance stems from multiple factors: the invasive nature of digital rectal exams, embarrassment about the procedure, and widespread misinformation about the necessity and frequency of screening. The prostate-specific antigen (PSA) blood test, a less invasive alternative, is often overlooked because men simply don't schedule regular check-ups where such tests would be routine. What makes this avoidance particularly dangerous is that prostate cancer typically develops slowly and silently, with no symptoms in its early stages when treatment is most effective. By the time symptoms like difficulty urinating, blood in urine, or pelvic pain appear, the cancer may have already advanced significantly. Early detection through regular screening can identify prostate cancer when the five-year survival rate exceeds 99%, compared to just 31% when detected at advanced stages. The American Cancer Society recommends that men discuss prostate cancer screening with their healthcare providers starting at age 50 for average-risk men, or at age 45 for those at higher risk, including African American men and those with a family history of prostate cancer.
2. Cardiovascular Health Assessments - Ignoring the Silent Killer
Heart disease remains the leading cause of death among men, claiming one life every 36 seconds in the United States, yet comprehensive cardiovascular assessments are among the most frequently skipped health evaluations. Men often dismiss early warning signs like chest discomfort, shortness of breath, or unusual fatigue as temporary stress or aging, failing to recognize these as potential indicators of serious heart conditions. The comprehensive cardiovascular assessment includes blood pressure monitoring, cholesterol panels, electrocardiograms, and stress tests—screenings that can identify risk factors and early-stage heart disease long before a heart attack or stroke occurs. The cultural expectation that men should be physically strong and resilient contributes to the dangerous tendency to "power through" symptoms that would prompt immediate medical attention in other contexts. Additionally, many men operate under the false assumption that heart problems only affect older individuals, leading younger men to skip cardiovascular screenings entirely. However, heart disease can begin developing in the twenties and thirties, with risk factors like high blood pressure, elevated cholesterol, diabetes, and obesity laying the groundwork for future cardiac events. Regular cardiovascular assessments can detect these risk factors early, allowing for lifestyle modifications and medical interventions that can prevent heart attacks, strokes, and other cardiovascular complications. The American Heart Association recommends that men begin regular cardiovascular screening by age 20, with frequency increasing based on risk factors and age.
3. Colorectal Cancer Screening - The Uncomfortable Truth About Prevention

Colorectal cancer screening represents one of the most effective yet underutilized preventive measures in men's healthcare, with colonoscopy avoidance rates reaching alarming levels despite colorectal cancer being the third most common cancer among men. The resistance to colorectal screening is multifaceted, involving embarrassment about the procedure, fear of discomfort, concerns about the preparation process, and the general reluctance to undergo what many perceive as an invasive examination. This avoidance is particularly tragic because colorectal cancer is highly preventable and treatable when detected early, with screening capable of identifying and removing precancerous polyps before they develop into malignant tumors. The colonoscopy procedure, while requiring preparation and temporary discomfort, can literally save lives by detecting cancer in its earliest stages when the five-year survival rate exceeds 90%. Men's tendency to postpone or avoid this screening often stems from a combination of practical concerns—such as taking time off work for the procedure and preparation—and psychological barriers related to vulnerability and loss of control. However, the alternatives to traditional colonoscopy, including stool-based tests and virtual colonoscopy, provide less invasive options that can still effectively screen for colorectal cancer. The American Cancer Society recommends that men at average risk begin regular colorectal cancer screening at age 45, with various screening options available to accommodate different comfort levels and medical situations.
4. Skin Cancer Examinations - Overlooking the Body's Largest Organ
Skin cancer screening is dramatically underutilized among men, despite men being twice as likely as women to die from melanoma and having higher rates of all types of skin cancer. The neglect of regular skin examinations stems from several factors unique to male behavior patterns: men are less likely to use sunscreen consistently, more likely to work in outdoor occupations with prolonged sun exposure, and significantly less inclined to perform self-examinations or seek professional skin assessments. This oversight is particularly dangerous because skin cancer, including the deadly melanoma, is highly treatable when detected early but can be fatal when allowed to progress undetected. Men often dismiss changes in moles, freckles, or skin lesions as insignificant, failing to recognize the ABCDE warning signs (Asymmetry, Border irregularity, Color variation, Diameter larger than a pencil eraser, and Evolution or change over time) that could indicate malignant transformation. The cultural association of tanned skin with health and attractiveness, combined with the perception that skincare is primarily a female concern, contributes to men's casual attitude toward sun protection and skin monitoring. Professional dermatological examinations can detect skin cancers that are invisible to the untrained eye, including those in hard-to-see areas like the back, scalp, and between toes. The American Academy of Dermatology recommends annual professional skin examinations for all adults, with more frequent monitoring for those with risk factors such as fair skin, family history of skin cancer, or numerous moles.
5. Diabetes Screening - The Silent Epidemic Going Undetected
Type 2 diabetes screening is critically underutilized among men, with millions living with undiagnosed diabetes that silently damages their cardiovascular system, kidneys, eyes, and nerves. Men are statistically more likely to develop type 2 diabetes than women, yet they're less likely to undergo regular blood glucose testing that could detect the condition in its early stages when lifestyle interventions are most effective. The insidious nature of type 2 diabetes means that many men experience years of elevated blood sugar without obvious symptoms, during which time the disease progressively damages multiple organ systems. When symptoms like excessive thirst, frequent urination, unexplained weight loss, or persistent fatigue do appear, many men attribute them to stress, aging, or temporary lifestyle factors rather than recognizing them as potential indicators of diabetes. The reluctance to undergo diabetes screening often relates to fear of dietary restrictions, concerns about medication dependence, and the overwhelming nature of managing a chronic condition. However, early detection through simple blood tests—including fasting glucose, hemoglobin A1C, or glucose tolerance tests—can identify diabetes or prediabetes when interventions like diet modification, exercise, and medication can prevent or significantly delay complications. The American Diabetes Association recommends that all adults, particularly men over 35 or those with risk factors such as obesity, family history, or sedentary lifestyle, undergo regular diabetes screening. Uncontrolled diabetes can lead to heart disease, stroke, kidney failure, blindness, and lower limb amputations, making early detection and management crucial for long-term health and quality of life.
6. Blood Pressure Monitoring - The Silent Killer's Early Warning System
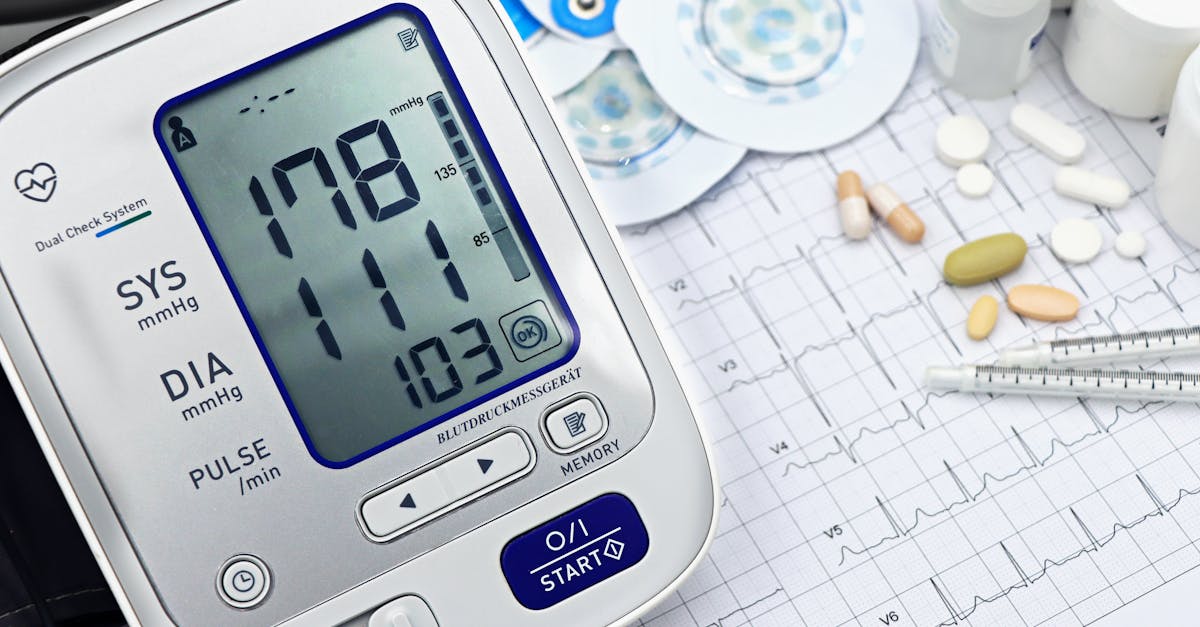
Hypertension, often called the "silent killer," affects nearly half of all American adults, yet regular blood pressure monitoring remains one of the most neglected aspects of men's preventive healthcare. Men are particularly susceptible to developing high blood pressure at younger ages than women, and they're more likely to have uncontrolled hypertension due to inconsistent medical care and medication non-adherence. The danger of untreated high blood pressure lies in its asymptomatic nature—most men feel perfectly normal while their elevated blood pressure silently damages their arteries, heart, brain, kidneys, and eyes. This false sense of wellness contributes to the casual attitude many men have toward blood pressure monitoring, often assuming that feeling good equates to being healthy. The cultural emphasis on male strength and invincibility makes it particularly difficult for men to accept that an invisible condition could pose serious health risks. Regular blood pressure monitoring is simple, non-invasive, and can be performed in various settings, yet many men only discover they have hypertension during emergency situations or routine procedures for other conditions. The consequences of untreated hypertension are severe and often irreversible: heart attacks, strokes, heart failure, kidney disease, and vision problems. The American Heart Association recommends that all adults have their blood pressure checked at least once every two years, with more frequent monitoring for those with elevated readings or risk factors. Early detection and management of hypertension through lifestyle modifications and medication can prevent most of these serious complications and significantly improve long-term health outcomes.
7. Cholesterol Testing - Understanding the Cardiovascular Risk Factor

Cholesterol screening represents a critical yet frequently overlooked component of men's preventive healthcare, with many men going years without understanding their cardiovascular risk profile. The lipid panel, a simple blood test that measures total cholesterol, LDL (bad) cholesterol, HDL (good) cholesterol, and triglycerides, provides essential information about heart disease and stroke risk, yet it's often skipped due to men's tendency to avoid routine medical appointments. The misconception that cholesterol problems only affect older or obviously unhealthy individuals leads many younger men to postpone this crucial screening, unaware that cholesterol issues can begin developing in the twenties and thirties. Men's dietary patterns, which often include higher consumption of saturated fats and processed foods, combined with lifestyle factors like stress, smoking, and sedentary behavior, make them particularly susceptible to developing unhealthy cholesterol levels. The absence of symptoms associated with high cholesterol creates a false sense of security, as elevated cholesterol silently contributes to atherosclerosis—the buildup of plaque in arteries that can lead to heart attacks and strokes. Cultural factors also play a role, as discussions about cholesterol and heart health are often perceived as less masculine concerns compared to more visible health issues. However, cholesterol screening is painless, quick, and provides actionable information that can guide dietary changes, exercise recommendations, and medication decisions. The American Heart Association recommends that men begin cholesterol screening by age 20, with follow-up testing every four to six years for those with normal levels, and more frequent monitoring for those with elevated readings or additional risk factors.
8. Testicular Cancer Self-Examinations - The Overlooked Young Man's Cancer

Testicular cancer, while relatively rare, represents the most common cancer among men aged 15 to 35, yet testicular self-examinations are among the most neglected aspects of men's health awareness and screening practices. The reluctance to perform regular testicular self-examinations stems from a combination of embarrassment, lack of education about proper technique, and the general discomfort many men feel about examining their own bodies. This avoidance is particularly concerning because testicular cancer, when detected early, has a cure rate exceeding 95%, but delayed detection can significantly complicate treatment and reduce survival rates. The cultural taboo surrounding male genital health contributes to the silence around testicular cancer awareness, with many men never receiving proper education about warning signs or examination techniques. Unlike many other cancers that primarily affect older individuals, testicular cancer strikes men in their prime reproductive and career-building years, making early detection crucial for preserving fertility and minimizing treatment impact on life goals. The signs of testicular cancer—including lumps, swelling, pain, or changes in testicle size or consistency—are often dismissed as minor injuries or temporary discomfort, leading to dangerous delays in seeking medical attention. Monthly testicular self-examinations, ideally performed after a warm shower when the scrotal skin is relaxed, can detect abnormalities early and prompt timely medical evaluation. Healthcare providers should educate young men about proper self-examination techniques and encourage open discussions about testicular health, while men should overcome embarrassment and prioritize this simple yet potentially life-saving screening practice.
9. Mental Health Assessments - Breaking the Stigma of Emotional Wellness
Mental health screening represents perhaps the most stigmatized and avoided aspect of men's healthcare, with devastating consequences reflected in suicide rates that are nearly four times higher among men than women. The cultural expectation that men should be emotionally stoic, self-reliant, and capable of handling problems independently creates significant barriers to seeking mental health assessment and treatment. Many men view mental health struggles as personal failures or signs of weakness, leading them to suffer in silence rather than seek professional help or even acknowledge their emotional distress. This avoidance is compounded by the tendency for depression and anxiety to manifest differently in men, often appearing as anger, irritability, substance abuse, or reckless behavior rather than the sadness or worry more commonly associated with mental health conditions. The workplace culture that rewards emotional suppression and the fear that mental health treatment could impact career advancement further discourage men from seeking help. Regular mental health assessments can identify conditions like depression, anxiety, PTSD, and substance abuse disorders before they reach crisis levels, enabling early intervention and treatment that can prevent suicide, relationship breakdown, and career destruction. Mental health screening doesn't require lengthy therapy commitments—it can begin with simple questionnaires and brief conversations with healthcare providers who can assess emotional well-being and provide appropriate referrals when needed. The normalization of mental health care as an essential component of overall wellness, rather than a sign of weakness, is crucial for encouraging men to prioritize their emotional well-being alongside their physical health.
10. Bone Density Testing - The Overlooked Risk of Male Osteoporosis
Bone density testing is dramatically underutilized among men, despite the fact that one in four men over age 50 will experience an osteoporosis-related fracture during their lifetime. The perception that osteoporosis is primarily a women's disease leads to significant gaps in male bone health screening, leaving millions of men unaware of their fracture risk until they experience a debilitating break. Men's bone density naturally peaks in their thirties and begins declining thereafter, but the gradual nature of bone loss means that osteoporosis develops silently without obvious symptoms until a fracture occurs. The cultural association of bone health with femininity, combined with men's general reluctance to discuss aging-related health concerns, contributes to the widespread neglect of bone density screening among the male population. Risk factors for male osteoporosis include age, family history, smoking, excessive alcohol consumption, sedentary lifestyle, certain medications (particularly corticosteroids), and underlying conditions like hypogonadism or gastrointestinal disorders that affect nutrient absorption. The consequences of undiagnosed osteoporosis in men can be severe, with hip fractures leading to significant disability, loss of independence, and increased mortality risk. Men who experience fractures from minor trauma or have risk factors for bone loss should undergo dual-energy X-ray absorptiometry (DEXA) scanning to assess bone density and fracture risk. Early detection of low bone density allows for interventions including calcium and vitamin D supplementation, weight-bearing exercise, lifestyle modifications, and medications that can prevent fractures and maintain bone health throughout aging.
11. Comprehensive Physical Examinations - The Foundation of Preventive Care
The annual comprehensive physical examination serves as the cornerstone of preventive healthcare, yet it remains one of the most commonly skipped medical appointments among men, with far-reaching consequences for early disease detection and health maintenance. This comprehensive assessment provides healthcare providers with the opportunity to evaluate multiple body systems, review family and personal medical history, assess risk factors, and coordinate the various screenings discussed throughout this article. Men's tendency to avoid routine physical examinations stems from multiple factors: the perception that they're unnecessary when feeling well, time constraints related to work and family obligations, cost concerns, and the general male inclination to seek medical care only when experiencing obvious symptoms. However, the comprehensive physical examination is designed to detect problems before symptoms appear, when interventions are most effective and least invasive. During these appointments, healthcare providers can identify subtle changes in vital signs, detect early signs of chronic diseases, assess mental health status, review medications and supplements, and provide personalized recommendations for lifestyle modifications. The examination also serves as an opportunity to establish a relationship with a healthcare provider who becomes familiar with individual health patterns and can recognize deviations from baseline more effectively. Regular comprehensive physical examinations enable the coordination of age-appropriate screenings, ensure that vaccinations remain current, and provide a forum for discussing health concerns in a confidential, professional setting. The investment in annual comprehensive physical examinations pays dividends through early disease detection, prevention of complications, and the development of a proactive rather than reactive approach to health management that can significantly improve both quality and quantity of life.