10 Bone Density Factors to Monitor After 40
After age 40, the human body undergoes a fundamental shift in bone metabolism that marks the beginning of a gradual but persistent decline in bone density. This biological milestone represents more than just another birthday—it signals the onset of a period where bone resorption begins to outpace bone formation, leading to an annual bone loss of approximately 0.5-1% per year in healthy adults. For women, this process accelerates dramatically during menopause, with bone loss rates potentially reaching 3-5% annually in the first five to ten years post-menopause. Understanding and monitoring the key factors that influence bone density becomes crucial during this phase of life, as the decisions made and lifestyle modifications implemented can significantly impact long-term skeletal health and quality of life. The complex interplay of hormonal changes, nutritional status, physical activity levels, and various health conditions creates a unique landscape of risk factors that require careful attention and proactive management to prevent osteoporosis and reduce fracture risk in later years.
1. Hormonal Changes and Their Impact on Bone Health

Hormonal fluctuations represent one of the most significant factors affecting bone density after 40, with estrogen and testosterone playing pivotal roles in maintaining skeletal integrity. Estrogen, often called the "bone protector hormone," directly inhibits osteoclast activity—the cells responsible for breaking down bone tissue—while simultaneously promoting osteoblast function for new bone formation. As women approach perimenopause and menopause, declining estrogen levels create an imbalance that favors bone resorption over formation, leading to accelerated bone loss. Similarly, men experience a gradual decline in testosterone levels, typically beginning around age 30 but becoming more pronounced after 40, which affects bone density through both direct and indirect mechanisms. Testosterone influences bone metabolism by converting to estrogen through the enzyme aromatase, and low testosterone levels are associated with increased fracture risk. Other hormonal factors include thyroid hormones, which when elevated can accelerate bone turnover, and parathyroid hormone, which regulates calcium metabolism. Growth hormone and insulin-like growth factor-1 also play crucial roles in bone remodeling, and their age-related decline contributes to the overall deterioration of bone health that characterizes the post-40 period.
2. Calcium Intake and Absorption Efficiency
Calcium serves as the primary building block of bone tissue, comprising approximately 99% of the body's total calcium stores, making adequate intake and absorption critical for maintaining bone density after 40. However, the relationship between calcium consumption and bone health becomes increasingly complex with age due to declining absorption efficiency and changing metabolic demands. Adults over 40 require 1,000-1,200 mg of calcium daily, but studies indicate that many individuals fall short of these recommendations, particularly those following restrictive diets or with lactose intolerance. More concerning is the age-related decline in calcium absorption efficiency, which drops from approximately 60% in young adults to 20% or less in older individuals due to decreased stomach acid production, reduced active vitamin D levels, and changes in intestinal calcium transport mechanisms. The timing and source of calcium intake also matter significantly—calcium from food sources generally provides better bioavailability than supplements, and spreading intake throughout the day optimizes absorption since the body can only absorb about 500 mg at one time. Additionally, certain foods and medications can interfere with calcium absorption, including high-sodium foods, excessive caffeine, and some antibiotics, making it essential to consider the overall dietary pattern rather than focusing solely on calcium quantity.
3. Vitamin D Status and Synthesis Challenges

Vitamin D functions as both a hormone and a vitamin, playing an indispensable role in calcium absorption and bone mineralization, yet vitamin D deficiency becomes increasingly common after age 40 due to multiple physiological and lifestyle factors. The skin's ability to synthesize vitamin D from sunlight exposure decreases by approximately 75% between ages 20 and 70, primarily due to reduced 7-dehydrocholesterol levels in the epidermis and changes in skin thickness. This age-related decline in cutaneous synthesis is compounded by lifestyle factors common in middle-aged adults, including increased time spent indoors, use of sunscreen, and living in northern latitudes with limited sun exposure during winter months. The kidneys' capacity to convert vitamin D to its active form, calcitriol, also diminishes with age, creating a double burden of reduced synthesis and impaired activation. Optimal vitamin D status requires serum 25-hydroxyvitamin D levels of at least 30 ng/mL (75 nmol/L), yet studies consistently show that 40-60% of adults over 40 have insufficient or deficient levels. Beyond its role in calcium absorption, vitamin D directly influences bone cells, with vitamin D receptors present on osteoblasts, osteoclasts, and osteocytes, making adequate levels essential for proper bone remodeling. The challenge of maintaining optimal vitamin D status through diet alone is significant, as few foods naturally contain substantial amounts, necessitating a combination of sensible sun exposure, fortified foods, and often supplementation.
4. Physical Activity Patterns and Bone-Loading Exercises

Physical activity serves as one of the most powerful modifiable factors for maintaining and improving bone density after 40, with weight-bearing and resistance exercises providing the mechanical stress necessary to stimulate bone formation through Wolff's Law—the principle that bones adapt to the forces placed upon them. However, many adults experience a significant decline in physical activity levels after 40 due to career demands, family responsibilities, and the onset of age-related physical limitations, creating a detrimental cycle where reduced activity accelerates bone loss. High-impact activities such as jumping, running, and dancing provide the greatest osteogenic stimulus by creating ground reaction forces that exceed body weight, while resistance training with progressively increasing loads stimulates bone formation at specific skeletal sites. The concept of "bone-loading" exercises emphasizes activities that create novel loading patterns and higher strain magnitudes than those experienced in daily activities, as bones become accustomed to routine stresses and require progressive overload to continue adapting. Research demonstrates that adults who maintain regular weight-bearing exercise can reduce age-related bone loss by 1-2% annually and may even increase bone density at certain sites. Conversely, sedentary behavior and prolonged periods of immobilization lead to rapid bone loss, with bed rest studies showing bone density decreases of 1-2% per month. The timing and type of exercise matter significantly—activities performed during peak bone mass years (teens and twenties) provide greater long-term benefits, but initiating or intensifying exercise programs after 40 can still yield meaningful improvements in bone density and fracture risk reduction.
5. Protein Requirements and Bone Matrix Formation
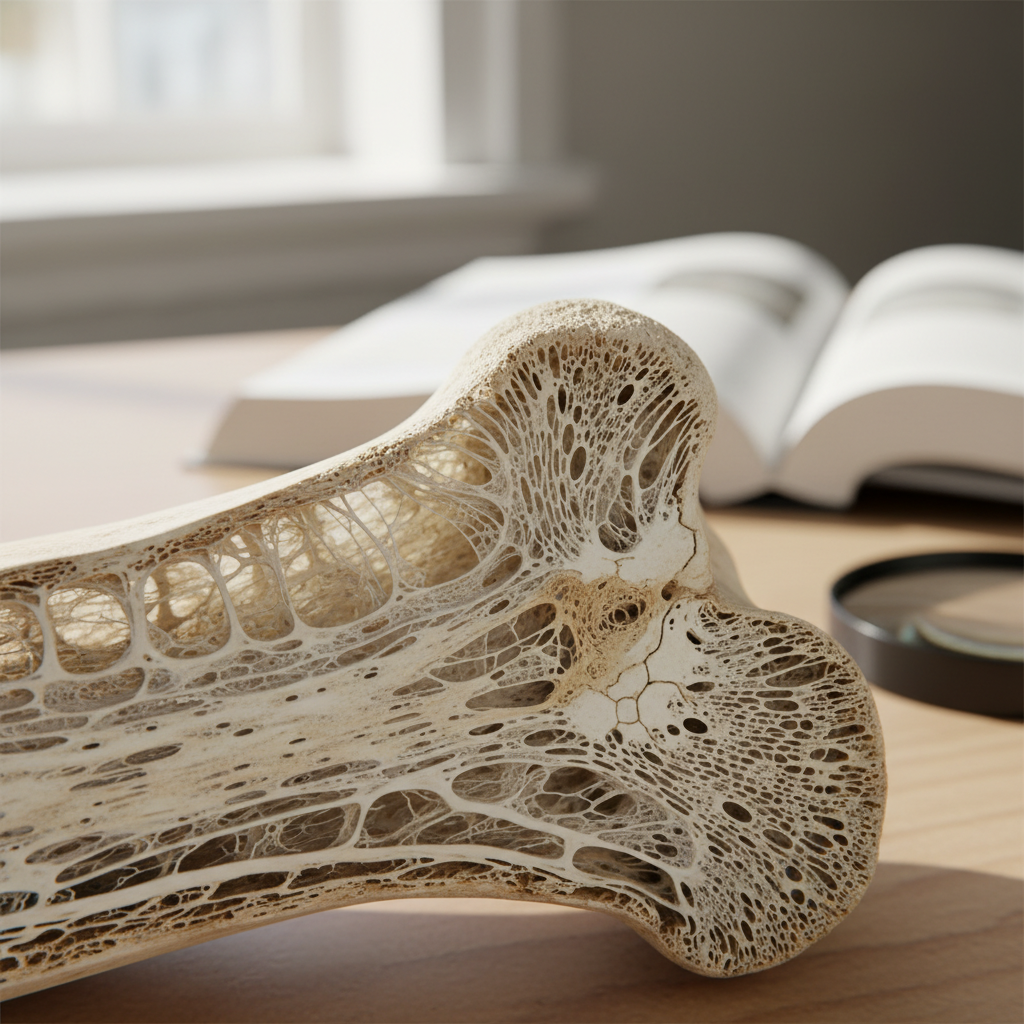
Protein plays a fundamental yet often underappreciated role in bone health, comprising approximately 50% of bone volume and providing the organic matrix upon which calcium and other minerals are deposited. After age 40, protein requirements for optimal bone health may actually increase due to age-related changes in protein metabolism, including decreased protein synthesis efficiency and increased protein breakdown rates. The recommended dietary allowance (RDA) of 0.8 grams per kilogram of body weight may be insufficient for older adults, with emerging research suggesting that 1.0-1.2 grams per kilogram may be more appropriate for maintaining bone health and muscle mass simultaneously. Protein provides essential amino acids, particularly lysine, proline, and glycine, which are crucial components of collagen—the primary protein in bone matrix that provides tensile strength and flexibility. Additionally, protein intake influences the production of insulin-like growth factor-1 (IGF-1), a hormone that promotes bone formation and helps maintain the coupling between bone resorption and formation. The source and timing of protein intake also matter, with complete proteins containing all essential amino acids being most beneficial for bone health. However, the relationship between protein and bone health is complex and influenced by acid-base balance—while adequate protein is essential, excessive protein intake without sufficient alkalizing foods (fruits and vegetables) may create an acidic environment that promotes calcium loss from bones. This highlights the importance of a balanced approach that emphasizes adequate protein intake within the context of an overall healthy dietary pattern rich in fruits, vegetables, and other bone-supporting nutrients.
6. Magnesium and Trace Mineral Balance

Magnesium serves as a critical cofactor in bone metabolism, with approximately 60% of the body's magnesium stored in bone tissue, yet magnesium deficiency is surprisingly common among adults over 40 and significantly impacts bone density and fracture risk. This essential mineral participates in over 300 enzymatic reactions related to bone health, including the conversion of vitamin D to its active form, the regulation of parathyroid hormone, and the formation of bone crystals. Magnesium deficiency can lead to impaired calcium absorption, altered vitamin D metabolism, and disrupted bone remodeling processes, creating a cascade of effects that compromise skeletal integrity. The recommended daily intake of magnesium for adults over 40 ranges from 320-420 mg, depending on gender and age, yet dietary surveys consistently show that 60-70% of adults consume less than the recommended amounts. This deficiency is particularly concerning because magnesium absorption decreases with age due to changes in intestinal function and increased use of medications that interfere with magnesium absorption, such as proton pump inhibitors and diuretics. Beyond magnesium, other trace minerals play crucial roles in bone health, including zinc, which is essential for collagen synthesis and bone formation; copper, which is required for cross-linking collagen fibers; manganese, which activates enzymes involved in bone matrix formation; and boron, which influences calcium and magnesium metabolism. The synergistic relationships between these minerals emphasize the importance of a comprehensive approach to bone nutrition rather than focusing on individual nutrients in isolation.
7. Body Weight and Mechanical Loading Effects

Body weight represents a double-edged factor in bone health after 40, with both extremely low and excessively high body weights presenting unique challenges for maintaining optimal bone density. Mechanical loading theory suggests that bones adapt to the forces placed upon them, and body weight provides a constant loading stimulus that helps maintain bone density—explaining why moderate overweight individuals often have higher bone density than their normal-weight counterparts. However, this relationship is complicated by the fact that excess adipose tissue, particularly visceral fat, produces inflammatory cytokines that can negatively impact bone metabolism and promote bone resorption. The relationship between body weight and bone health also varies by skeletal site, with weight-bearing bones like the hip and spine showing stronger correlations with body weight than non-weight-bearing sites like the radius. Rapid weight loss, whether intentional or unintentional, poses significant risks for bone health, with studies showing that losing more than 10% of body weight can result in substantial bone loss, particularly when weight loss occurs through caloric restriction alone without adequate protein intake or resistance exercise. This is particularly relevant for adults over 40 who may undergo weight loss interventions for health reasons but inadvertently compromise their bone health in the process. The timing and method of weight loss matter significantly—gradual weight loss combined with resistance training and adequate protein intake can minimize bone loss, while rapid weight loss through severe caloric restriction often results in significant bone density reductions. Additionally, weight cycling (repeated cycles of weight loss and regain) may have particularly detrimental effects on bone health, emphasizing the importance of sustainable weight management strategies.
8. Medication Effects and Drug-Induced Bone Loss

Numerous medications commonly prescribed to adults over 40 can significantly impact bone metabolism and accelerate bone loss, making medication review and monitoring essential components of bone health management. Glucocorticoids (corticosteroids) represent the most well-known class of bone-damaging medications, with even low doses causing rapid bone loss through multiple mechanisms including decreased calcium absorption, increased calcium excretion, reduced osteoblast function, and increased osteoclast activity. Proton pump inhibitors (PPIs), widely used for acid reflux and peptic ulcer disease, can impair calcium absorption by reducing stomach acid production and have been associated with increased fracture risk, particularly with long-term use. Selective serotonin reuptake inhibitors (SSRIs) and other antidepressants may affect bone density through their influence on serotonin signaling pathways in bone cells, with some studies showing increased fracture risk in long-term users. Anticonvulsants can interfere with vitamin D metabolism and calcium absorption, while certain cancer treatments, including aromatase inhibitors and androgen deprivation therapy, dramatically reduce sex hormone levels and accelerate bone loss. Diuretics present a complex picture—thiazide diuretics may actually benefit bone health by reducing calcium excretion, while loop diuretics can increase calcium loss and negatively impact bone density. Anticoagulants, particularly heparin with long-term use, can cause significant bone loss, and even some over-the-counter medications like aluminum-containing antacids can interfere with calcium absorption when used regularly. The challenge lies in balancing the medical necessity of these medications with their potential bone health consequences, often requiring collaborative care between multiple healthcare providers to optimize both disease management and skeletal health through careful medication selection, dosing adjustments, and implementation of bone-protective strategies.
9. Lifestyle Factors - Smoking, Alcohol, and Caffeine
Lifestyle choices significantly impact bone health after 40, with smoking, excessive alcohol consumption, and high caffeine intake representing modifiable risk factors that can accelerate bone loss and increase fracture risk through various physiological mechanisms. Smoking represents one of the most detrimental lifestyle factors for bone health, with cigarette smoke containing numerous toxic compounds that directly and indirectly damage bone tissue. Nicotine and other chemicals in tobacco smoke reduce blood flow to bones, impair osteoblast function, increase osteoclast activity, and interfere with calcium absorption and vitamin D metabolism. Additionally, smoking affects hormone levels, reducing estrogen production in women and testosterone in men, further compromising bone health. The effects of smoking on bone density are dose-dependent and duration-dependent, with long-term smokers showing significantly lower bone density and higher fracture rates than non-smokers. Alcohol consumption presents a complex relationship with bone health—moderate consumption (1-2 drinks per day) may have neutral or even slightly beneficial effects on bone density, possibly due to alcohol's influence on estrogen levels and its anti-inflammatory properties. However, excessive alcohol consumption (more than 2-3 drinks per day) significantly impairs bone formation, interferes with calcium and vitamin D metabolism, increases fall risk, and is associated with poor nutritional status. Caffeine intake, while less dramatic in its effects, can increase calcium excretion and may negatively impact bone health when consumption exceeds 400 mg per day (approximately 4 cups of coffee) without adequate calcium intake. The timing of caffeine consumption also matters, as consuming caffeine with calcium-rich foods can further impair calcium absorption.
10. Chronic Disease Impact on Bone Metabolism
Chronic diseases become increasingly prevalent after age 40 and can significantly impact bone metabolism through direct effects on bone cells, indirect effects on hormone levels and nutrient absorption, and through the medications used for treatment. Diabetes mellitus, both type 1 and type 2, affects bone health through multiple pathways including advanced glycation end products (AGEs) that accumulate in bone collagen and compromise bone quality, chronic inflammation that promotes bone resorption, and microvascular complications that impair bone blood supply. Additionally, some diabetes medications, particularly thiazolidinediones, can accelerate bone loss and increase fracture risk. Inflammatory conditions such as rheumatoid arthritis, inflammatory bowel disease, and chronic kidney disease create systemic inflammation that disrupts the balance between bone formation and resorption, often leading to accelerated bone loss even before treatment begins. The inflammatory cytokines produced in these conditions, including tumor necrosis factor-alpha and interleukin-6, directly stimulate osteoclast activity and inhibit osteoblast function. Gastrointestinal disorders can impair nutrient absorption, particularly calcium, vitamin D, and other bone-essential nutrients, while liver disease affects vitamin D metabolism and protein synthesis necessary for bone matrix formation. Endocrine disorders, including hyperthyroidism, hyperparathyroidism, and Cushing's syndrome, can dramatically accelerate bone turnover and lead to rapid bone loss. Cancer and cancer treatments present particular challenges, with many chemotherapy agents, radiation therapy, and hormone-blocking treatments having significant negative effects on bone health. The cumulative impact of multiple chronic conditions, often present simultaneously in older adults, creates complex interactions that require comprehensive management strategies to preserve bone health while treating the underlying diseases.
11. Monitoring Strategies and Preventive Measures
Effective monitoring of bone health after 40 requires a comprehensive approach that combines clinical assessments, laboratory testing, imaging studies, and lifestyle evaluations to identify risk factors early and implement appropriate preventive measures. Bone density testing using dual-energy X-ray absorptiometry (DEXA) scanning represents the gold standard for assessing bone health, with initial screening recommended for all women at age 65 and men at age 70, though earlier screening may be warranted for individuals with risk factors. The frequency of follow-up DEXA scans depends on initial results and risk factors, typically ranging from 1-2 years for high-risk individuals to 3-5 years for those with normal bone density. However, DEXA scanning only measures bone quantity, not quality, leading to increased interest in additional assessment tools such as trabecular bone score (TBS), which evaluates bone microarchitecture, and biochemical markers of bone turnover that can provide insights into the rate of bone remodeling. Laboratory monitoring should include assessment of vitamin D status (25-hydroxyvitamin D), calcium levels, parathyroid hormone, and markers of bone turnover such as C-terminal telopeptide (CTX) and procollagen type 1 N-terminal propeptide (P1NP). Regular evaluation of modifiable risk factors includes assessment of dietary intake, physical activity levels, medication use, and lifestyle factors, with particular attention to changes that may impact bone health. Preventive measures should be individualized based on risk assessment and may include dietary modifications to ensure adequate calcium and vitamin