10 Metabolic Health Indicators That Matter More Than Your Scale Number
The modern obsession with weight loss has created a dangerous misconception that the number on your bathroom scale is the ultimate measure of health and metabolic function. This reductive approach to wellness has led millions of people down a frustrating path of yo-yo dieting, metabolic damage, and psychological distress, all while missing the crucial indicators that truly reflect their body's internal health status. Metabolic health encompasses a complex web of physiological processes that determine how efficiently your body converts food into energy, regulates blood sugar, manages inflammation, and maintains cellular function. While weight can be one factor in overall health, it fails to capture the intricate dance of hormones, enzymes, and metabolic pathways that actually dictate your energy levels, disease risk, and longevity. Research consistently shows that individuals can maintain optimal metabolic health across a wide range of body weights, while others may appear "healthy" by conventional standards yet harbor significant metabolic dysfunction. This comprehensive exploration will unveil ten critical metabolic health indicators that provide a far more accurate and actionable picture of your body's true state, empowering you to make informed decisions that support genuine wellness rather than chasing arbitrary numbers that may actually work against your long-term health goals.
1. Insulin Sensitivity - The Master Metabolic Switch
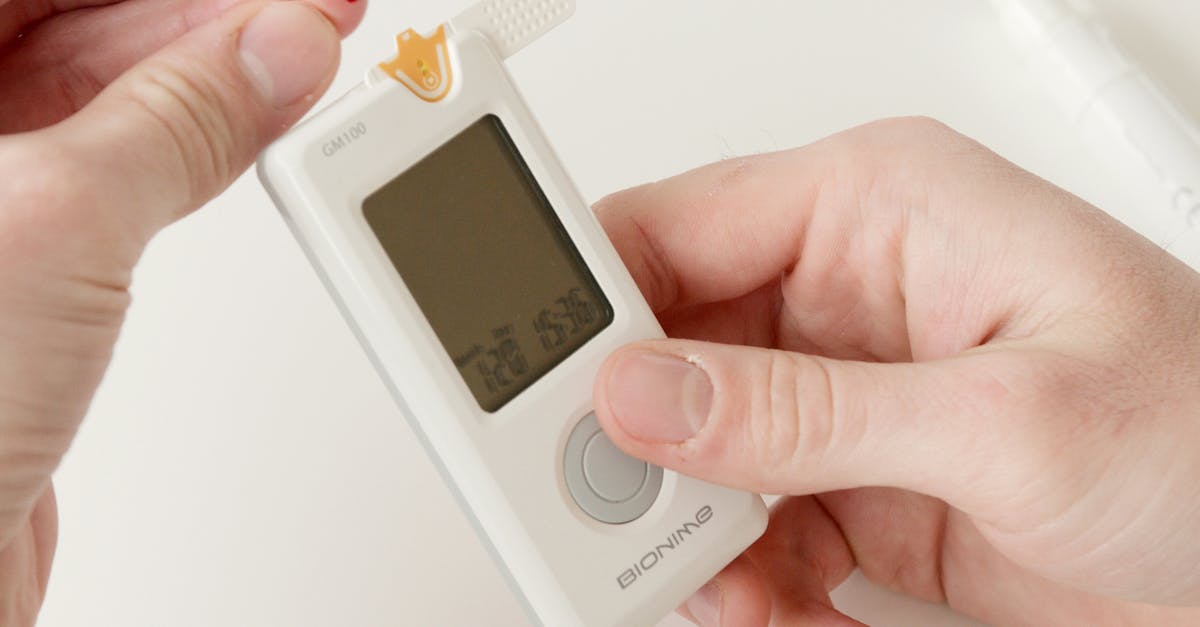
Insulin sensitivity stands as perhaps the most crucial metabolic health indicator, functioning as the master switch that controls how your body processes and stores energy from food. When your cells respond efficiently to insulin, glucose is readily absorbed from the bloodstream and either used for immediate energy or stored appropriately in muscle and liver tissue. However, when insulin sensitivity deteriorates—a condition known as insulin resistance—your pancreas must produce increasingly higher amounts of insulin to achieve the same glucose-lowering effect, creating a cascade of metabolic dysfunction that extends far beyond blood sugar control. This process affects every major organ system, influencing fat storage patterns, inflammatory responses, cardiovascular health, and even cognitive function. Unlike weight, which can fluctuate daily due to water retention, hormonal cycles, and other temporary factors, insulin sensitivity reflects the fundamental efficiency of your cellular machinery and provides insight into your risk for type 2 diabetes, metabolic syndrome, and cardiovascular disease. You can assess insulin sensitivity through various methods, including the HOMA-IR calculation (derived from fasting glucose and insulin levels), glucose tolerance tests, or even observing how your body responds to carbohydrate-containing meals. Improving insulin sensitivity through targeted lifestyle interventions—such as strength training, intermittent fasting, adequate sleep, and strategic carbohydrate timing—can dramatically enhance metabolic health regardless of whether significant weight loss occurs, making this marker far more valuable than scale weight for long-term health optimization.
2. Waist-to-Hip Ratio - The Shape of Health

The distribution of body fat provides significantly more insight into metabolic health than total body weight, with the waist-to-hip ratio serving as a powerful predictor of cardiovascular disease, diabetes risk, and overall metabolic function. This simple measurement reflects the critical distinction between subcutaneous fat (stored just beneath the skin) and visceral fat (accumulated around internal organs), with the latter being metabolically active tissue that secretes inflammatory compounds and interferes with normal organ function. Research consistently demonstrates that individuals with higher waist-to-hip ratios—indicating more abdominal fat accumulation—face elevated risks of insulin resistance, dyslipidemia, hypertension, and chronic inflammation, regardless of their overall body weight or BMI classification. The optimal waist-to-hip ratio varies slightly between sexes, with values below 0.90 for men and 0.85 for women generally indicating lower metabolic risk, while ratios above 1.0 for men and 0.85 for women signal increased health concerns. This measurement proves particularly valuable because it can improve significantly through targeted interventions like resistance training and stress management, even when total body weight remains stable or increases due to muscle gain. Unlike the scale, which cannot distinguish between muscle, fat, water, and bone mass, the waist-to-hip ratio specifically targets the type of fat accumulation most strongly linked to metabolic dysfunction. Regular monitoring of this ratio provides actionable feedback about the effectiveness of lifestyle interventions and offers a more accurate assessment of health improvements than weight alone, making it an essential tool for anyone serious about optimizing their metabolic health.
3. Resting Metabolic Rate - Your Cellular Engine's Efficiency

Resting metabolic rate (RMR) represents the energy your body requires to maintain basic physiological functions while at complete rest, serving as a window into the efficiency and health of your cellular machinery. This measurement reflects the cumulative activity of all your body's energy-demanding processes, including protein synthesis, cellular repair, immune function, cardiovascular activity, and neurological operations, providing insight into your metabolic health that weight alone cannot capture. A robust RMR indicates healthy mitochondrial function, adequate muscle mass, optimal thyroid activity, and efficient cellular processes, while a suppressed metabolic rate may signal metabolic adaptation, nutrient deficiencies, hormonal imbalances, or the aftermath of restrictive dieting practices. Unlike weight, which can decrease due to muscle loss, dehydration, or metabolic slowdown, a healthy RMR should remain relatively stable or even increase as you build lean tissue and optimize your metabolic health through appropriate nutrition and exercise strategies. The relationship between RMR and body composition proves particularly important, as muscle tissue burns significantly more calories at rest than fat tissue, meaning two individuals of identical weight can have vastly different metabolic rates depending on their body composition. Factors that support a healthy RMR include adequate protein intake, regular resistance training, sufficient sleep, proper hydration, and avoiding extreme caloric restrictions that can trigger adaptive thermogenesis. Monitoring RMR through indirect calorimetry or bioelectrical impedance analysis provides valuable feedback about the metabolic impact of your lifestyle choices, helping you distinguish between healthy weight changes that preserve metabolic function and counterproductive approaches that may compromise your long-term metabolic health.
4. Blood Glucose Variability - The Hidden Metabolic Disruptor

Blood glucose variability—the degree to which blood sugar levels fluctuate throughout the day—has emerged as a critical metabolic health indicator that often reveals dysfunction long before traditional markers like fasting glucose or HbA1c show abnormalities. While conventional diabetes screening focuses on average blood sugar levels or single-point measurements, glucose variability captures the dynamic nature of metabolic function and provides insight into how well your body maintains homeostasis in response to meals, stress, sleep, and physical activity. High glucose variability, characterized by dramatic spikes and crashes in blood sugar levels, indicates poor metabolic flexibility and can contribute to oxidative stress, inflammation, endothelial dysfunction, and accelerated aging processes, even when average glucose levels appear normal. This metabolic turbulence affects energy levels, mood stability, cognitive function, and hunger regulation, creating a cycle of cravings, energy crashes, and metabolic stress that weight measurements cannot detect. Continuous glucose monitoring technology has revolutionized our understanding of glucose variability, revealing that individuals can maintain stable weight while experiencing significant metabolic dysfunction, or conversely, achieve excellent glucose control across various body weights. Factors that influence glucose variability include meal timing and composition, sleep quality, stress levels, physical activity patterns, and individual genetic variations in glucose metabolism. Optimizing glucose variability through strategies like balanced macronutrient intake, regular meal timing, stress management, and appropriate exercise can dramatically improve metabolic health markers, energy levels, and long-term disease risk, regardless of whether these interventions result in weight loss. This makes glucose variability a far more sensitive and actionable indicator of metabolic health than scale weight, particularly for individuals seeking to optimize their energy and prevent chronic disease.
5. Inflammatory Markers - The Silent Metabolic Saboteur
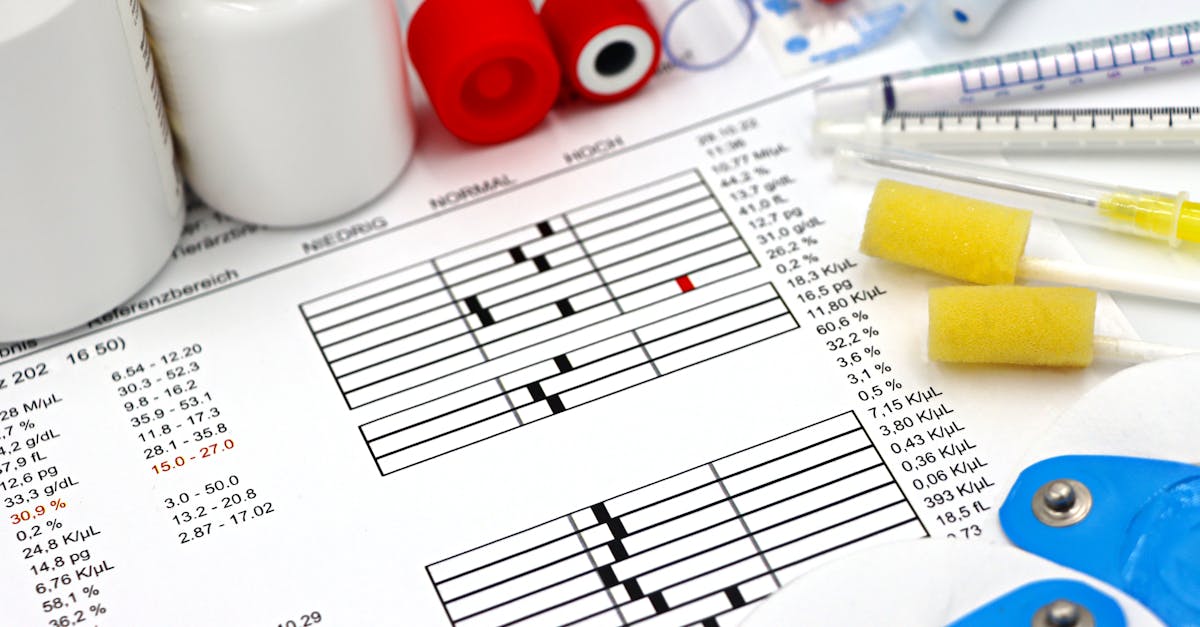
Chronic low-grade inflammation represents one of the most insidious threats to metabolic health, operating as a silent saboteur that disrupts normal cellular function, impairs insulin sensitivity, and accelerates the development of chronic diseases long before symptoms become apparent. Unlike acute inflammation, which serves as a protective response to injury or infection, chronic inflammation persists at subclinical levels, creating a state of metabolic dysfunction that cannot be detected by simply stepping on a scale. Key inflammatory markers such as C-reactive protein (CRP), interleukin-6 (IL-6), and tumor necrosis factor-alpha (TNF-α) provide direct insight into this hidden metabolic disruption, revealing the true state of your body's internal environment and its capacity for optimal function. Elevated inflammatory markers correlate strongly with insulin resistance, cardiovascular disease, neurodegenerative conditions, and accelerated aging, making them far more predictive of long-term health outcomes than body weight alone. The relationship between inflammation and metabolism proves particularly complex, as inflammatory cytokines can directly interfere with insulin signaling pathways, promote fat storage (especially visceral fat), and disrupt the normal regulation of appetite and energy expenditure. Factors that influence inflammatory status include diet quality, sleep patterns, stress levels, physical activity, gut health, and environmental toxin exposure—many of which can be optimized regardless of weight changes. Anti-inflammatory interventions such as omega-3 fatty acid supplementation, regular moderate exercise, stress reduction techniques, and consumption of polyphenol-rich foods can significantly improve inflammatory markers and metabolic health even when body weight remains stable. Monitoring inflammatory markers provides valuable feedback about the effectiveness of lifestyle interventions and offers early warning signs of metabolic dysfunction, making these measurements infinitely more valuable than scale weight for assessing and optimizing long-term health outcomes.
6. Sleep Quality and Recovery Metrics - The Metabolic Reset Button

Sleep quality and recovery metrics serve as fundamental pillars of metabolic health, functioning as the body's natural reset button that orchestrates hormonal balance, cellular repair, and metabolic optimization during periods of rest. Unlike weight, which provides no information about the quality of your recovery processes, sleep metrics reveal the efficiency of critical metabolic functions including growth hormone release, cortisol regulation, glucose metabolism, and inflammatory resolution that occur predominantly during deep sleep phases. Poor sleep quality disrupts the delicate balance of hunger hormones (ghrelin and leptin), leading to increased appetite, cravings for high-calorie foods, and impaired satiety signaling that can persist for days after a single night of inadequate rest. Additionally, sleep deprivation directly impairs insulin sensitivity, with studies showing that even one night of poor sleep can reduce glucose tolerance by up to 40%, creating a state of temporary diabetes-like metabolism that compounds with chronic sleep debt. Modern sleep tracking technology allows for precise monitoring of sleep architecture, including time spent in deep sleep, REM sleep, and light sleep phases, as well as recovery metrics like heart rate variability (HRV) that reflect autonomic nervous system balance and stress resilience. These measurements provide actionable insights into metabolic health that weight cannot capture, revealing how lifestyle factors like caffeine timing, screen exposure, meal timing, and stress management affect your body's ability to recover and maintain optimal metabolic function. Individuals can maintain excellent sleep quality and recovery metrics across a wide range of body weights, while others may achieve their "ideal" weight through methods that severely compromise sleep and recovery, ultimately damaging their metabolic health. Prioritizing sleep optimization through consistent sleep schedules, optimal sleep environment conditions, and stress management techniques often leads to improvements in all other metabolic health markers, making sleep quality a cornerstone metric that deserves equal or greater attention than scale weight in any comprehensive health assessment.
7. Cardiovascular Efficiency Markers - The Metabolic Highway System
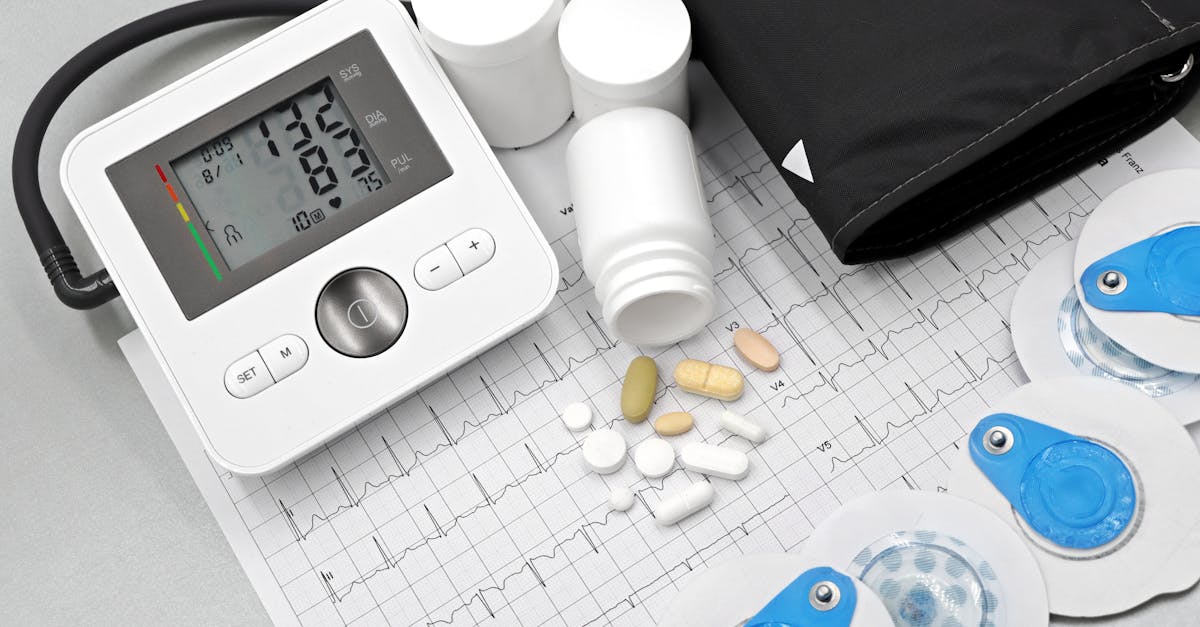
Cardiovascular efficiency markers provide crucial insights into your body's metabolic highway system, revealing how effectively your circulatory system delivers nutrients and oxygen to tissues while removing metabolic waste products—functions that are essential for optimal cellular metabolism but completely invisible to bathroom scales. Key cardiovascular metrics include resting heart rate, heart rate variability, blood pressure, and recovery heart rate after exercise, each offering unique perspectives on cardiovascular health and metabolic function that transcend simple weight measurements. A lower resting heart rate typically indicates a more efficient cardiovascular system that can pump more blood with each beat, reducing the workload on the heart and reflecting good cardiovascular conditioning and metabolic health. Heart rate variability (HRV), which measures the variation in time between heartbeats, serves as a window into autonomic nervous system balance and stress resilience, with higher HRV generally indicating better metabolic flexibility and recovery capacity. Blood pressure measurements reveal the health of your vascular system and its ability to efficiently transport nutrients and hormones throughout the body, with optimal readings supporting better insulin sensitivity, cognitive function, and overall metabolic performance. Exercise recovery metrics, such as how quickly your heart rate returns to baseline after physical activity, provide insight into cardiovascular fitness and metabolic efficiency that can improve dramatically through appropriate training regardless of weight changes. These cardiovascular markers often improve significantly through metabolic health interventions like regular aerobic exercise, strength training, stress management, and dietary optimization, even when body weight remains stable or increases due to muscle gain. Unlike weight, which can fluctuate based on numerous temporary factors, cardiovascular efficiency markers reflect the fundamental health of your body's transport and delivery systems, making them invaluable indicators of metabolic health and predictors of long-term health outcomes that deserve primary attention in any comprehensive health assessment.
8. Hormonal Balance Indicators - The Metabolic Orchestra Conductors

Hormonal balance serves as the master conductor of your metabolic orchestra, coordinating complex physiological processes that determine energy production, fat storage, muscle synthesis, and cellular repair—functions that operate independently of the number displayed on your bathroom scale. Key hormonal indicators include thyroid hormones (TSH, T3, T4), sex hormones (testosterone, estrogen, progesterone), stress hormones (cortisol), and metabolic hormones (leptin, ghrelin, adiponectin), each playing crucial roles in metabolic health that weight measurements cannot capture or reflect. Thyroid function directly controls metabolic rate, with even subclinical thyroid dysfunction capable of significantly impacting energy levels, body composition, and metabolic efficiency while potentially maintaining stable weight through compensatory mechanisms. Sex hormone balance affects muscle mass, fat distribution, bone density, and insulin sensitivity, with hormonal imbalances often manifesting as metabolic dysfunction long before weight changes become apparent. Chronic stress and elevated cortisol levels can promote visceral fat accumulation, impair glucose metabolism, and disrupt sleep patterns while potentially maintaining or even reducing total body weight through muscle catabolism and appetite suppression. The intricate relationships between these hormones create feedback loops that can either support or undermine metabolic health regardless of weight status, making hormonal assessment far more informative than scale measurements for understanding true metabolic function. Factors that influence hormonal balance include sleep quality, stress management, nutrient intake, exercise patterns, environmental toxin exposure, and circadian rhythm regulation—all of which can be optimized through targeted interventions that may or may not result in weight changes. Regular monitoring of key hormonal markers provides valuable insights into the effectiveness of lifestyle interventions and can reveal metabolic improvements or dysfunction that weight alone would never detect, making hormonal assessment an essential component of any comprehensive metabolic health evaluation that prioritizes long-term wellness over short-term weight fluctuations.
9. Body Composition Analysis - Beyond the Scale's Deception

Body composition analysis reveals the true story of your metabolic health by distinguishing between muscle mass, fat mass, bone density, and water content—critical information that remains completely hidden when you rely solely on total body weight measurements. This detailed breakdown of body composition provides insight into metabolic health that can be dramatically different from what scale weight suggests, as individuals can maintain identical weights while having vastly different metabolic profiles based on their muscle-to-fat ratios and fat distribution patterns. Muscle tissue serves as a metabolically active reservoir that burns calories at rest, improves insulin sensitivity, and supports healthy aging, making muscle mass preservation and development far more important for long-term health than achieving any particular weight target. Advanced body composition analysis methods, including DEXA scans, bioelectrical impedance analysis, and hydrostatic weighing, can reveal improvements in metabolic health such as increased lean mass, reduced visceral fat, and improved bone density that occur independently of weight changes and provide more accurate assessments of health progress. The relationship between body composition and metabolic health proves particularly important during periods of lifestyle change, as effective interventions often result in simultaneous muscle gain and fat loss that may produce minimal weight changes while dramatically improving metabolic function, cardiovascular health, and physical performance. Factors that positively influence body composition include resistance training, adequate protein intake, proper recovery, and hormonal optimization—strategies that can significantly enhance metabolic health across a wide range of body weights. Regular body composition monitoring provides actionable feedback about the effectiveness of training and nutrition protocols, helping individuals distinguish between beneficial changes that improve metabolic health and counterproductive approaches that may achieve weight loss through muscle loss or dehydration. This makes body composition analysis an invaluable tool for anyone seeking to optimize their metabolic health based on physiological improvements rather than arbitrary weight targets that may actually work against long-term health and wellness goals.
10. Energy Levels and Physical Performance - The Metabolic Output Indicators

Energy levels and physical performance serve as real-world indicators of metabolic health that reflect how efficiently your body converts nutrients into usable energy and maintains physiological function under various demands—metrics that provide far more practical insight than scale weight into your body's true operational capacity. Consistent energy levels throughout the day indicate stable blood sugar regulation, efficient mitochondrial function, adequate nutrient status, and balanced hormonal production, while energy crashes, fatigue, and performance declines often signal underlying metabolic dysfunction that may exist regardless of body weight. Physical performance metrics, including strength, endurance, power output, and recovery capacity, reflect the integrated function of multiple metabolic systems working in harmony to support movement and adaptation to training stimuli. These performance indicators often improve dramatically through metabolic health optimization strategies, even when body weight remains stable or increases due to muscle development and improved hydration status. The relationship between energy levels and metabolic health proves particularly revealing during daily activities, as individuals with optimal metabolic function typically experience stable mood, sustained mental clarity, and consistent physical energy that doesn't require constant stimulation from caffeine or sugar to maintain. Factors that support optimal energy levels and performance include balanced macronutrient intake, proper meal timing, adequate sleep, stress management, regular physical activity, and sufficient micronutrient status—interventions that can dramatically improve quality of life regardless of their impact on scale weight. Monitoring energy patterns and physical