12 Resting Heart Rate Ranges by Age and What Yours Is Telling You
Your resting heart rate serves as one of the most accessible and revealing windows into your cardiovascular health, functioning as a silent messenger that continuously broadcasts vital information about your body's condition. This fundamental vital sign, measured when you're completely at rest and relaxed, represents the number of times your heart beats per minute to maintain essential circulation throughout your body. While many people focus on dramatic health indicators or complex medical tests, your resting heart rate offers immediate insights that can predict everything from your fitness level to potential health risks. Understanding the intricate relationship between age, lifestyle, and heart rate patterns empowers you to make informed decisions about your health and recognize when changes might signal underlying issues. As we age, our cardiovascular system undergoes natural transformations that directly influence our resting heart rate, making age-specific ranges crucial for accurate health assessment. This comprehensive exploration will guide you through twelve distinct age-related heart rate ranges, revealing what your personal numbers are telling you about your current health status and future cardiovascular risks.
1. The Science Behind Resting Heart Rate - Understanding Your Body's Natural Rhythm
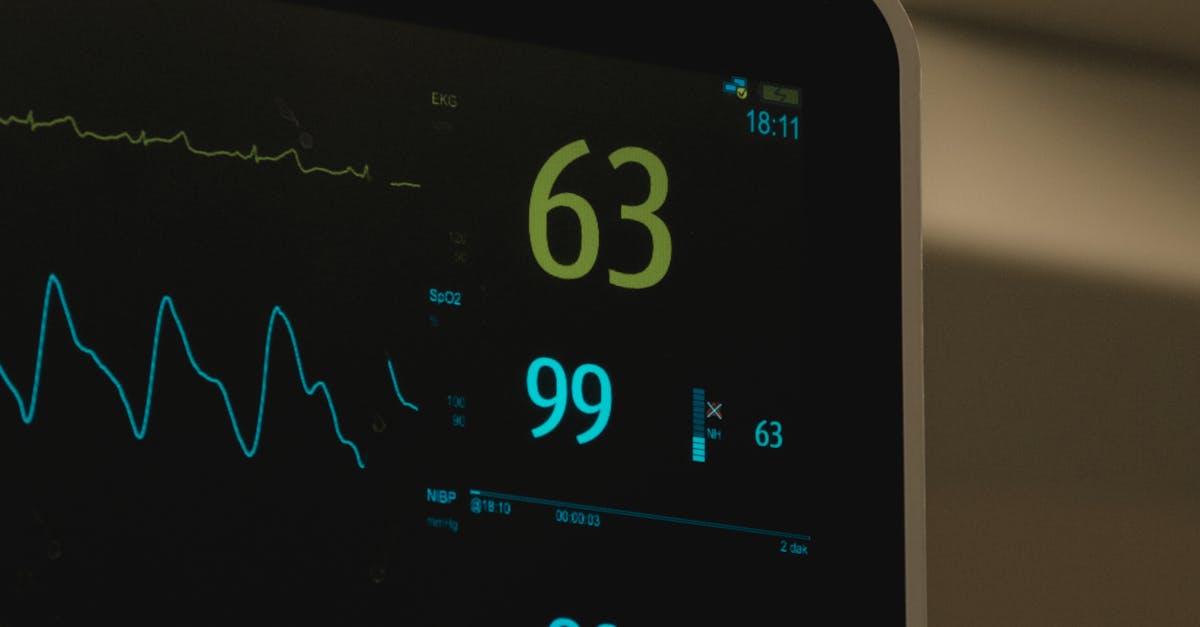
The physiological mechanisms governing your resting heart rate involve a complex interplay between your autonomic nervous system, cardiac muscle efficiency, and overall cardiovascular conditioning. Your heart's natural pacemaker, the sinoatrial node, generates electrical impulses that regulate heartbeat frequency, while the parasympathetic and sympathetic nervous systems fine-tune this rhythm based on your body's immediate needs and long-term conditioning. Research published in the European Heart Journal demonstrates that resting heart rate serves as a reliable predictor of cardiovascular mortality, with each 10-beat-per-minute increase correlating to a 16% higher risk of death from heart disease. The efficiency of your heart muscle directly influences how many beats are required to pump adequate blood throughout your circulatory system, explaining why well-conditioned athletes often display remarkably low resting heart rates. Factors such as blood volume, stroke volume (the amount of blood pumped with each heartbeat), and peripheral resistance all contribute to determining your optimal resting heart rate. Additionally, hormonal influences, including thyroid function, stress hormones like cortisol, and even seasonal variations in daylight exposure, can significantly impact your baseline heart rate measurements.
2. Newborns to Toddlers (0-2 Years) - The Rapid Rhythm of Growth

Infants and toddlers exhibit the highest resting heart rates across all age groups, typically ranging from 100 to 160 beats per minute, reflecting their accelerated metabolic demands and developing cardiovascular systems. During the first year of life, a baby's heart must support rapid physical growth, brain development, and the establishment of efficient circulation patterns, requiring significantly more cardiac output per unit of body weight compared to adults. Pediatric cardiologists explain that newborns' hearts beat faster partly because their stroke volume is naturally smaller, necessitating increased frequency to maintain adequate circulation. The American Heart Association notes that heart rates in this age group can vary dramatically based on activity level, emotional state, and even feeding schedules, with sleeping rates often dropping to the lower end of the range while active play can push rates toward the upper limits. Parents should understand that brief spikes above 160 beats per minute during crying or active play are typically normal, but sustained elevated rates or unusually low rates below 100 beats per minute warrant pediatric evaluation. Environmental factors such as room temperature, clothing layers, and even the presence of fever can significantly influence heart rate measurements in this vulnerable population, making context crucial for accurate interpretation.
3. Preschoolers (3-5 Years) - Transitioning to Stability

Preschool-aged children typically display resting heart rates between 90 and 130 beats per minute, representing a gradual decline from infancy as their cardiovascular systems mature and become more efficient. This age group experiences significant developmental changes that directly impact heart rate patterns, including improved cardiac muscle strength, increased blood volume, and enhanced nervous system regulation of cardiovascular function. Research from the American Academy of Pediatrics indicates that children in this age range begin developing more predictable heart rate patterns, though individual variations remain substantial based on genetics, activity levels, and overall health status. The transition from toddlerhood to preschool age marks an important period where parents and healthcare providers can begin establishing baseline measurements that will serve as reference points for future health assessments. Physical activity during these formative years plays a crucial role in establishing healthy heart rate patterns, with active children often displaying lower resting rates and better cardiovascular recovery times. Sleep quality and duration significantly influence heart rate measurements in preschoolers, as inadequate rest can elevate baseline rates and mask underlying health issues that might otherwise be apparent through routine monitoring.
4. School Age Children (6-12 Years) - Building Cardiovascular Foundation
School-age children typically maintain resting heart rates between 75 and 115 beats per minute, reflecting continued cardiovascular development and the establishment of more adult-like heart rate patterns. This period represents a critical window for cardiovascular health education and the development of lifelong fitness habits that will significantly influence future heart health outcomes. Studies published in Pediatric Exercise Science demonstrate that children who engage in regular physical activity during these formative years develop more efficient cardiovascular systems, often displaying resting heart rates at the lower end of the normal range. The increased structure of school schedules, organized sports participation, and growing awareness of health concepts make this an ideal time for teaching children about heart rate monitoring and cardiovascular wellness. Nutritional factors become increasingly important during this age range, as dietary habits established in childhood directly influence cardiovascular health and can impact resting heart rate measurements. Healthcare providers emphasize that establishing baseline heart rate measurements during routine school physicals creates valuable reference points for detecting future changes that might indicate developing health issues or the need for lifestyle modifications.
5. Teenagers (13-18 Years) - Navigating Hormonal Influences

Adolescents experience resting heart rates typically ranging from 60 to 100 beats per minute, though hormonal fluctuations during puberty can create temporary variations that challenge standard interpretation guidelines. The dramatic physical and hormonal changes occurring during teenage years significantly impact cardiovascular function, with growth spurts, hormonal surges, and lifestyle changes all contributing to heart rate variability. Research from the Journal of Adolescent Health reveals that teenagers who participate in regular cardiovascular exercise often develop resting heart rates similar to trained adults, sometimes dropping below 60 beats per minute without indicating underlying health problems. Sleep patterns during adolescence, often characterized by later bedtimes and insufficient total sleep duration, can artificially elevate resting heart rates and mask the true cardiovascular fitness level. Stress factors unique to teenage years, including academic pressure, social dynamics, and identity formation challenges, can chronically elevate heart rates and establish patterns that persist into adulthood. Mental health considerations become particularly important during this age range, as anxiety and depression can significantly influence heart rate patterns and require specialized interpretation by healthcare providers familiar with adolescent development.
6. Young Adults (19-30 Years) - Peak Performance Potential

Young adults typically exhibit resting heart rates between 60 and 100 beats per minute, representing the age group with the greatest potential for achieving optimal cardiovascular fitness and the lowest sustainable heart rates. This life stage offers unique opportunities for establishing excellent cardiovascular health habits, as the heart muscle retains maximum adaptability and responsiveness to training stimuli. Exercise physiologists note that well-trained young adults can achieve resting heart rates in the 40-60 beat per minute range, indicating exceptional cardiovascular efficiency and reduced long-term health risks. The lifestyle choices made during young adulthood, including exercise habits, dietary patterns, stress management techniques, and substance use decisions, create lasting impacts on cardiovascular health that extend far beyond this age period. Career establishment, relationship formation, and educational pursuits during these years often introduce new stress patterns that can influence heart rate measurements and require careful monitoring to prevent the development of chronic cardiovascular issues. Sleep quality and consistency become increasingly important as young adults navigate changing schedules and responsibilities, with poor sleep hygiene often manifesting as elevated resting heart rates that can persist until healthy patterns are reestablished.
7. Early Middle Age (31-40 Years) - Maintaining Momentum
Adults in their thirties typically maintain resting heart rates between 60 and 100 beats per minute, though this decade often marks the beginning of gradual cardiovascular changes that require increased attention to heart health maintenance. Research from the Framingham Heart Study indicates that this age group represents a critical period for preventing the onset of cardiovascular disease, with heart rate patterns serving as early indicators of developing risk factors. The responsibilities of career advancement, family formation, and financial obligations during this life stage often challenge the maintenance of optimal fitness levels, potentially leading to gradual increases in resting heart rate over time. Hormonal changes, particularly in women approaching perimenopause, can begin influencing heart rate patterns and require adjusted interpretation guidelines to distinguish between normal physiological changes and concerning health developments. Stress management becomes increasingly crucial during this decade, as chronic work and family pressures can establish elevated heart rate patterns that increase long-term cardiovascular risk. Healthcare providers emphasize that establishing regular monitoring routines during the thirties creates valuable baseline data for detecting future changes and implementing preventive interventions before significant health issues develop.
8. Midlife Transition (41-50 Years) - Adapting to Change
The fifth decade of life typically sees resting heart rates ranging from 60 to 100 beats per minute, though individual variations become more pronounced as the cumulative effects of lifestyle choices and genetic factors become increasingly apparent. This age group often experiences the first significant signs of cardiovascular aging, including slight increases in resting heart rate, reduced heart rate variability, and decreased maximum heart rate capacity during exercise. Hormonal changes, particularly menopause in women and gradual testosterone decline in men, can significantly influence heart rate patterns and require specialized interpretation by healthcare providers familiar with midlife physiology. The prevalence of risk factors such as hypertension, elevated cholesterol, and insulin resistance increases substantially during this decade, often manifesting as subtle changes in heart rate patterns before more obvious symptoms develop. Work-related stress often peaks during the forties as individuals navigate senior career responsibilities, eldercare obligations, and teenage children, creating chronic stress patterns that can persistently elevate resting heart rates. Research published in Circulation demonstrates that individuals who maintain regular exercise routines and stress management practices during this decade can preserve heart rate patterns similar to younger adults, highlighting the continued importance of lifestyle interventions.
9. Pre-Retirement Years (51-60 Years) - Recognizing Early Warning Signs
Adults in their fifties typically display resting heart rates between 60 and 100 beats per minute, though this decade often reveals the first clear signs of age-related cardiovascular changes that require increased monitoring and potential medical intervention. The natural aging process begins affecting the heart's electrical conduction system, sometimes resulting in slight increases in resting heart rate or the development of occasional irregular rhythms that warrant professional evaluation. This age group experiences the highest incidence of newly diagnosed cardiovascular conditions, including hypertension, coronary artery disease, and arrhythmias, making heart rate monitoring an essential component of preventive healthcare strategies. Medication effects become increasingly relevant during this decade, as many individuals begin taking prescription drugs for various health conditions that can significantly influence heart rate measurements and require careful monitoring by healthcare providers. The approach of retirement often brings both stress relief and anxiety about financial security and life changes, creating emotional factors that can impact heart rate patterns and require consideration during health assessments. Sleep disorders, including sleep apnea and insomnia, become more prevalent during the fifties and can significantly influence resting heart rate measurements, sometimes masking underlying cardiovascular issues or creating false alarms about heart health.
10. Early Senior Years (61-70 Years) - Embracing Healthy Aging
Individuals in their sixties typically maintain resting heart rates between 60 and 100 beats per minute, though age-related changes in cardiovascular function become more pronounced and require careful interpretation within the context of overall health status. The natural aging process affects heart muscle efficiency, electrical conduction pathways, and blood vessel flexibility, sometimes resulting in slightly elevated resting heart rates even in the absence of disease. Research from the Journal of the American Geriatrics Society indicates that seniors who maintain regular physical activity can preserve heart rate patterns similar to much younger individuals, demonstrating the continued benefits of exercise throughout the aging process. Medication management becomes increasingly complex during this decade, as many seniors take multiple prescription drugs that can interact to influence heart rate in unexpected ways, requiring careful coordination between healthcare providers and regular monitoring. The retirement transition often brings significant lifestyle changes that can positively or negatively impact heart rate patterns, depending on how individuals adapt to increased leisure time and potentially reduced physical activity levels. Chronic health conditions become more prevalent during the sixties, with conditions such as diabetes, arthritis, and cognitive changes potentially influencing heart rate measurements and requiring specialized interpretation by geriatric healthcare specialists.
11. Active Aging (71-80 Years) - Maintaining Vitality
Seniors in their seventies typically exhibit resting heart rates between 60 and 100 beats per minute, though individual variations become more significant as the cumulative effects of genetics, lifestyle choices, and medical history create diverse cardiovascular profiles within this age group. The concept of "successful aging" emphasizes that chronological age alone does not determine heart rate patterns, with many active seniors maintaining cardiovascular function comparable to individuals decades younger. Age-related changes in the autonomic nervous system can affect heart rate variability and recovery patterns, making it important for healthcare providers to consider these factors when evaluating cardiovascular health in older adults. Polypharmacy, or the use of multiple medications, becomes increasingly common during this decade and can significantly influence heart rate measurements through direct cardiac effects, drug interactions, and side effects that impact overall cardiovascular function. Social factors, including social isolation, loss of loved ones, and changes in living situations, can significantly impact heart rate patterns through stress-related mechanisms that require consideration during health assessments. Research published in Age and Ageing demonstrates that seniors who maintain strong social connections and engage in regular physical activity often display more favorable heart rate patterns and better overall cardiovascular health outcomes.
12. Advanced Years (81+ Years) - Wisdom in Monitoring
Individuals over eighty typically maintain resting heart rates between 60 and 100 beats per minute, though the interpretation of these measurements requires specialized knowledge of age-related physiological changes and the complex interplay of multiple health conditions common in this population. The aging heart undergoes structural and functional changes that can influence heart rate patterns, including increased stiffness of heart muscle, changes in electrical conduction, and reduced responsiveness to nervous system regulation. Healthcare providers emphasize that heart rate monitoring in this age group should focus on detecting significant changes from individual baseline measurements rather than strict adherence to population-based normal ranges. The prevalence of atrial fibrillation and other cardiac arrhythmias increases substantially after age eighty, making regular heart rate monitoring essential for early detection and appropriate management of these potentially serious conditions. Quality of life considerations become paramount during this life stage, with heart rate monitoring serving as one tool for optimizing comfort, function, and independence rather than solely focusing on disease prevention. Palliative care principles often guide heart rate interpretation in this population, emphasizing symptom management and comfort over aggressive interventions, while still maintaining vigilance for treatable conditions that could improve quality of life.
13. Taking Action - What Your Heart Rate Is Telling You

Understanding your personal heart rate patterns within the context of your age group provides valuable insights that can guide important health decisions and lifestyle modifications to optimize your cardiovascular wellness. Consistently elevated resting heart rates may indicate underlying health issues such as hyperthyroidism, anemia, dehydration, or cardiovascular disease, warranting professional medical evaluation and potential intervention strategies. Conversely, unusually low heart rates, particularly when accompanied by symptoms such as fatigue, dizziness, or shortness of breath, may signal problems with the heart's electrical system or medication effects that require immediate medical attention. The trend of your heart rate measurements over time often provides more valuable information than isolated readings, making regular monitoring and record-keeping essential components of proactive health management. Lifestyle factors including regular exercise, stress management, adequate sleep, proper nutrition, and avoiding tobacco and excessive alcohol can significantly improve heart rate patterns and overall cardiovascular health across all age groups. Modern technology, including fitness trackers and smartphone applications, has made heart rate monitoring more accessible than ever, empowering individuals to take an active role in cardiovascular health management while working collaboratively with healthcare providers to interpret results and implement appropriate interventions when necessary.