12 Vision Changes That Warrant an Eye Exam
Your eyes serve as the primary gateway through which you experience the world, processing an estimated 80% of all sensory information that reaches your brain. Yet despite their fundamental importance, many people take their vision for granted until noticeable changes occur. The human visual system is remarkably complex, involving not just the eyes themselves but intricate neural pathways that can be affected by numerous factors ranging from age-related changes to serious underlying health conditions. Recognizing when vision changes warrant professional attention is crucial for maintaining optimal eye health and preventing potentially irreversible damage. While some visual fluctuations may seem minor or temporary, they can often signal the early stages of conditions that, if left untreated, could lead to significant vision loss or even blindness. This comprehensive examination of twelve critical vision changes will empower you to make informed decisions about when to seek professional eye care, potentially saving your sight and improving your quality of life for years to come.
1. Sudden Vision Loss - When Every Second Counts
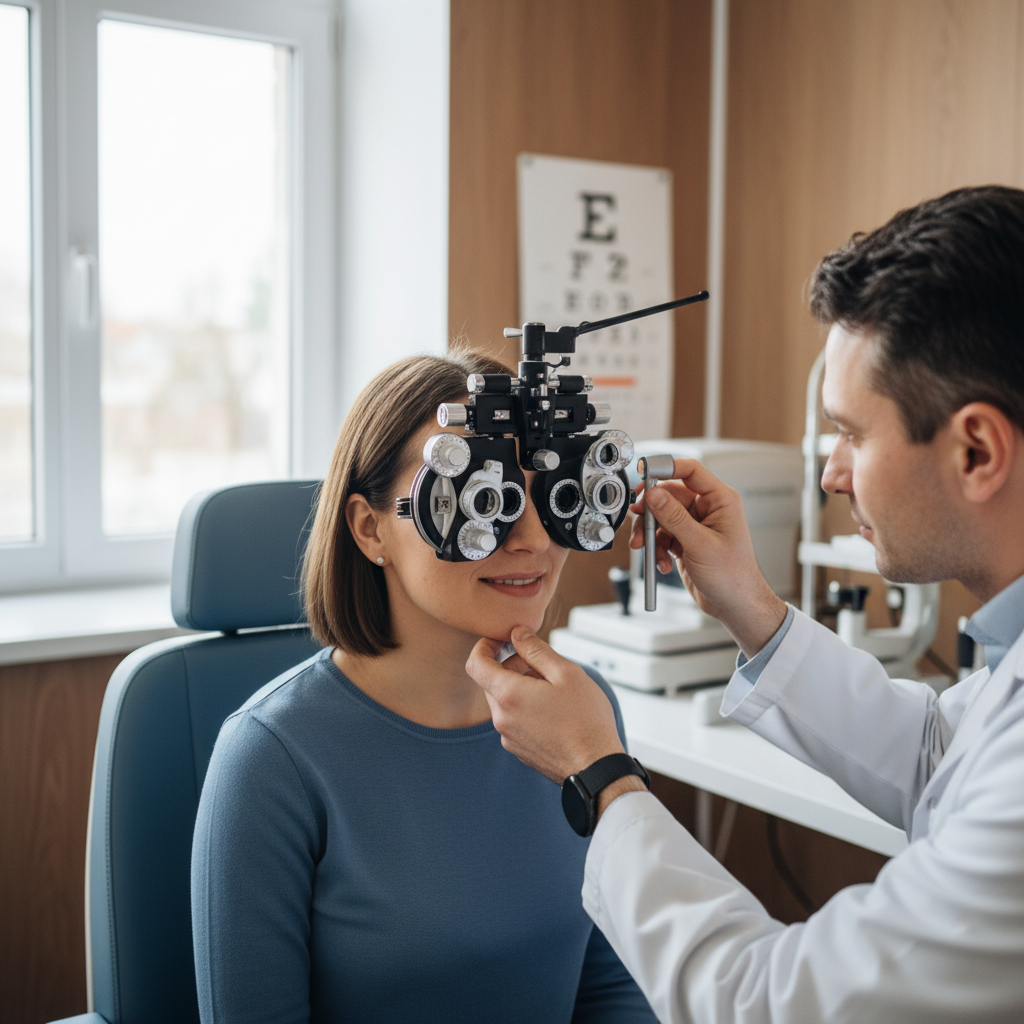
Sudden vision loss represents one of the most urgent eye-related emergencies, demanding immediate medical attention regardless of whether it affects one or both eyes. This dramatic change can manifest as complete blackness, severe blurriness that doesn't improve with blinking, or the sensation of a curtain falling across your field of vision. The underlying causes range from retinal detachment and stroke to severe glaucoma attacks and arterial blockages in the eye. Retinal detachment, for instance, occurs when the light-sensitive tissue at the back of the eye separates from its supporting layer, cutting off the blood supply and potentially causing permanent vision loss if not treated within hours. Similarly, a stroke affecting the visual cortex can cause sudden vision loss that may be accompanied by other neurological symptoms. Central retinal artery occlusion, often called an "eye stroke," blocks blood flow to the retina and requires emergency intervention to prevent irreversible damage. The key factor in all these conditions is time – the sooner treatment begins, the better the chances of preserving vision. Never adopt a "wait and see" approach with sudden vision loss; instead, seek emergency medical care immediately, as this symptom often indicates conditions where every minute of delay can mean the difference between sight and blindness.
2. Persistent Blurry Vision - Beyond Simple Refractive Errors
While occasional blurry vision might result from fatigue, dry eyes, or the need for updated prescription glasses, persistent blurriness that doesn't resolve with rest or blinking warrants thorough investigation. This symptom can indicate various underlying conditions, from developing cataracts and diabetic retinopathy to more serious neurological issues. Cataracts, characterized by the clouding of the eye's natural lens, typically develop gradually and may initially cause only slight blurriness that worsens over time. Diabetic retinopathy, a complication of diabetes affecting the blood vessels in the retina, can cause fluctuating vision that becomes progressively worse without proper management. Additionally, persistent blurry vision might signal the onset of age-related macular degeneration, particularly when it affects central vision and makes reading or recognizing faces difficult. Refractive errors such as myopia, hyperopia, or astigmatism can also worsen over time, requiring prescription updates. However, when blurriness persists despite corrective lenses or appears suddenly in someone with previously stable vision, it may indicate more serious conditions requiring immediate attention. The brain's visual processing centers can also be affected by conditions such as multiple sclerosis or brain tumors, manifesting as persistent visual disturbances that don't respond to conventional treatments.
3. Flashing Lights and Floaters - Distinguishing Normal from Alarming

The appearance of flashing lights (photopsia) and floaters in your visual field can range from benign age-related changes to serious retinal emergencies requiring immediate intervention. Floaters, those small specks, threads, or cobweb-like shapes that drift across your vision, are often caused by tiny clumps of gel or cells inside the vitreous humor, the clear gel-like substance filling the eye. While most floaters are harmless and become less noticeable over time, a sudden increase in their number, especially when accompanied by flashing lights, can indicate a retinal tear or detachment. Flashing lights typically appear as brief streaks or arcs of light in your peripheral vision and occur when the vitreous gel pulls on the retina. This tugging sensation can sometimes cause the retina to tear, leading to retinal detachment if left untreated. The classic warning signs include a sudden shower of floaters, persistent flashing lights, and the appearance of a shadow or curtain in your peripheral vision. Posterior vitreous detachment, while often benign, can sometimes lead to retinal complications and should be evaluated promptly. Age-related changes in the vitreous are common after age 50, but any sudden onset of these symptoms, regardless of age, requires urgent ophthalmologic evaluation to rule out sight-threatening conditions.
4. Double Vision - Unraveling Complex Neurological and Ocular Causes

Double vision, or diplopia, presents a particularly concerning symptom that can stem from various causes ranging from simple muscle imbalances to serious neurological conditions. When you see two images of a single object, either side by side (horizontal diplopia) or one above the other (vertical diplopia), it indicates a disruption in the normal coordination between your eyes or the brain's processing of visual information. Monocular diplopia, where double vision persists even when one eye is covered, often results from problems within the eye itself, such as cataracts, corneal irregularities, or lens dislocation. However, binocular diplopia, which disappears when either eye is covered, typically indicates issues with eye muscle control or nerve function. Conditions such as myasthenia gravis, an autoimmune disorder affecting muscle function, can cause fluctuating double vision that worsens with fatigue. Thyroid eye disease can inflame and restrict eye muscles, leading to persistent diplopia. More seriously, double vision can signal neurological conditions including stroke, brain tumors, or aneurysms affecting the cranial nerves that control eye movement. Multiple sclerosis frequently presents with diplopia as an early symptom. Given the wide range of potential causes, from relatively benign to life-threatening, any persistent double vision requires prompt medical evaluation to determine the underlying cause and initiate appropriate treatment.
5. Severe Eye Pain - Recognizing Emergency Conditions

Intense eye pain, particularly when accompanied by other symptoms such as nausea, vomiting, or vision changes, can indicate serious conditions requiring immediate medical attention. Acute angle-closure glaucoma represents one of the most urgent causes of severe eye pain, occurring when the drainage angle of the eye becomes suddenly blocked, causing rapid increases in intraocular pressure. This condition typically presents with excruciating pain, often described as feeling like the eye is being pushed out of its socket, along with nausea, vomiting, halos around lights, and rapid vision loss. Without immediate treatment to reduce eye pressure, permanent vision loss can occur within hours. Corneal abrasions, while less sight-threatening, can cause significant pain and discomfort, particularly when the protective surface layer of the cornea is scratched or damaged. Foreign bodies embedded in the eye, chemical burns, or severe infections can also produce intense pain requiring urgent care. Optic neuritis, inflammation of the optic nerve often associated with multiple sclerosis, typically causes deep, aching pain that worsens with eye movement. Cluster headaches, while not originating in the eye itself, can cause severe pain around and behind the eye. The key distinction lies in recognizing when eye pain accompanies other concerning symptoms such as vision loss, light sensitivity, or neurological signs, as these combinations often indicate conditions where delayed treatment can result in permanent complications.
6. Light Sensitivity - From Mild Discomfort to Serious Underlying Conditions
Photophobia, or abnormal sensitivity to light, can range from mild discomfort in bright environments to severe pain that makes normal daily activities impossible. While some degree of light sensitivity is normal, particularly when transitioning from dark to bright environments, persistent or severe photophobia often indicates underlying eye or neurological conditions. Corneal problems, including abrasions, infections, or dystrophies, frequently cause significant light sensitivity as the damaged corneal surface becomes hypersensitive to stimulation. Uveitis, inflammation of the eye's middle layer, commonly presents with photophobia along with eye pain, redness, and blurred vision. This condition can be associated with autoimmune disorders, infections, or trauma and requires prompt treatment to prevent complications such as cataracts, glaucoma, or vision loss. Migraine headaches often include photophobia as a prominent symptom, with sufferers seeking dark, quiet environments during episodes. More seriously, meningitis and other central nervous system infections can cause severe photophobia as an early warning sign. Certain medications, including some antibiotics and anti-inflammatory drugs, can increase light sensitivity as a side effect. Albinism and other genetic conditions affecting pigmentation can cause lifelong photophobia due to reduced melanin in the eyes. When light sensitivity interferes with daily activities, persists despite avoiding bright lights, or accompanies other symptoms such as eye pain or vision changes, professional evaluation is essential to identify and treat the underlying cause.
7. Night Vision Problems - Understanding Diminished Low-Light Vision

Difficulty seeing in low-light conditions, known as nyctalopia or night blindness, can significantly impact quality of life and safety, particularly when driving after dark or navigating dimly lit environments. This condition can result from various factors, ranging from nutritional deficiencies to serious retinal diseases. Vitamin A deficiency, while rare in developed countries, remains a leading cause of night blindness worldwide and can progress to complete blindness if left untreated. More commonly, cataracts can cause increasing difficulty with night vision as the clouded lens scatters light and reduces the amount reaching the retina. Retinitis pigmentosa, a group of inherited disorders affecting the retina's rod cells responsible for low-light vision, typically begins with night blindness and peripheral vision loss before progressing to more severe visual impairment. Diabetic retinopathy can also affect night vision as damage to retinal blood vessels compromises the eye's ability to function in low-light conditions. Age-related changes in the eye, including reduced pupil size and decreased retinal sensitivity, naturally diminish night vision capabilities over time. Certain medications, particularly those used to treat malaria or some psychiatric conditions, can cause temporary night vision problems. Additionally, uncorrected refractive errors may become more noticeable in low-light conditions when the pupils dilate and optical aberrations become more prominent. When night vision problems develop suddenly, worsen rapidly, or significantly impact daily activities, comprehensive eye examination is crucial to identify treatable causes and prevent further deterioration.
8. Peripheral Vision Loss - Detecting Silent Vision Thieves

Loss of peripheral or side vision often develops gradually and may go unnoticed until it becomes severe, earning conditions like glaucoma the nickname "silent thief of sight." The peripheral visual field encompasses everything you can see while looking straight ahead, and its loss can significantly impact mobility, driving safety, and overall quality of life. Glaucoma, a group of eye diseases characterized by damage to the optic nerve, typically begins by affecting peripheral vision while leaving central vision intact until advanced stages. This pattern makes early detection challenging, as people may not notice the gradual loss until significant damage has occurred. Open-angle glaucoma, the most common form, progresses slowly and painlessly, while angle-closure glaucoma can cause rapid peripheral vision loss accompanied by severe symptoms. Retinal detachment can cause peripheral vision loss that may progress toward central vision if not treated promptly. Brain tumors, strokes, or other neurological conditions affecting the visual cortex can cause specific patterns of peripheral vision loss called visual field defects. Retinitis pigmentosa typically begins with night blindness and progresses to tunnel vision as peripheral retinal cells deteriorate. Even seemingly unrelated conditions such as severe high blood pressure or diabetes can cause peripheral vision changes through their effects on retinal blood vessels. Regular comprehensive eye exams including visual field testing are essential for detecting peripheral vision loss early, particularly for individuals with risk factors such as family history of glaucoma, diabetes, or high eye pressure.
9. Color Vision Changes - Beyond Congenital Color Blindness

While most people associate color vision problems with congenital color blindness, acquired changes in color perception can indicate serious underlying eye or neurological conditions requiring prompt attention. Acquired color vision defects differ from inherited forms in that they typically affect one eye more than the other, may worsen over time, and often accompany other visual symptoms. Optic neuritis, inflammation of the optic nerve commonly associated with multiple sclerosis, frequently causes reduced color saturation and difficulty distinguishing between colors, particularly reds. Patients often describe colors as appearing "washed out" or less vibrant than normal. Diabetic retinopathy can affect color vision as damage to retinal blood vessels compromises the function of color-sensitive cone cells. Age-related macular degeneration may cause difficulty distinguishing between similar colors, particularly in the central visual field where cone cells are most densely packed. Cataracts can cause a yellowing effect that makes it difficult to distinguish between blues and purples or causes all colors to appear less vibrant. Certain medications, including some used to treat heart conditions, malaria, or tuberculosis, can cause temporary or permanent color vision changes. Retinal detachment may cause color vision abnormalities in the affected area of vision. Toxic exposures to substances such as carbon monoxide or certain industrial chemicals can damage the retina and optic nerve, resulting in color vision defects. When color vision changes develop in adulthood, particularly if accompanied by other visual symptoms, comprehensive evaluation is essential to identify and treat potentially serious underlying conditions.
10. Halos Around Lights - Optical Phenomena and Underlying Pathology
The appearance of halos or rings of light around bright objects, particularly at night, can indicate various eye conditions ranging from minor refractive issues to serious diseases requiring immediate treatment. While small halos around lights may be normal, especially in low-light conditions or when pupils are dilated, prominent or persistent halos often signal underlying problems. Acute angle-closure glaucoma classically presents with rainbow-colored halos around lights, accompanied by severe eye pain, nausea, and rapid vision loss. This represents a true medical emergency requiring immediate intervention to prevent permanent blindness. Cataracts commonly cause halos around lights as the clouded lens scatters incoming light, creating a ring-like appearance around bright objects. This symptom often worsens at night when pupils dilate, allowing more scattered light to enter the eye. Corneal edema, or swelling of the cornea, can cause halos by disrupting the cornea's normally smooth surface and creating optical irregularities. This condition can result from various causes, including eye trauma, infections, or complications from eye surgery. Fuchs' dystrophy, a progressive condition affecting the cornea's inner layer, often begins with morning halos that improve throughout the day as corneal swelling decreases. Certain types of contact lenses or refractive surgery complications can also cause halos around lights. Additionally, some medications that affect pupil size or corneal hydration may contribute to halo formation. When halos around lights develop suddenly, are accompanied by pain or vision loss, or significantly interfere with night driving or daily activities, prompt ophthalmologic evaluation is essential to determine the cause and initiate appropriate treatment.
11. Frequent Headaches with Visual Symptoms - The Eye-Brain Connection
The relationship between vision problems and headaches is complex, with eye strain, refractive errors, and serious ocular conditions all capable of triggering head pain. However, when headaches consistently accompany visual symptoms such as blurred vision, light sensitivity, or visual disturbances, they may indicate conditions requiring specialized attention. Eye strain headaches, often called asthenopic headaches, typically result from prolonged visual tasks, uncorrected refractive errors, or muscle imbalances that force the eyes to work harder than normal. These headaches usually occur after extended periods of reading, computer work, or other close visual tasks and may be accompanied by eye fatigue, burning, or tearing. Migraine headaches frequently include visual components such as aura, photophobia, or temporary vision changes, and may be triggered by specific visual stimuli such as flickering lights or patterns. Cluster headaches, while less common, cause severe pain around one eye and may be accompanied by eye redness, tearing, and temporary vision changes. More concerning are headaches associated with increased intracranial pressure, which can result from brain tumors, aneurysms, or other neurological conditions and may present with vision changes, double vision, or visual field defects. Temporal arteritis, an inflammatory condition affecting blood vessels in the head and neck, can cause severe headaches along with vision loss and requires immediate treatment to prevent blindness. Acute angle-closure glaucoma often presents with severe headache and eye pain accompanied by nausea and vision changes. When headaches consistently occur with visual symptoms, worsen over time, or are accompanied by neurological signs, comprehensive evaluation by both eye care professionals and neurologists may be necessary.
12. Difficulty Focusing or Eye Strain - Modern Visual Demands and Underlying Conditions

In our increasingly digital world, complaints of difficulty focusing and eye strain have become more common, but distinguishing between normal visual fatigue and underlying conditions requiring treatment is crucial for maintaining long-term eye health. Computer Vision Syndrome, also known as Digital Eye Strain, affects millions of people who spend extended periods using digital devices and typically presents with symptoms including difficulty focusing, eye fatigue, dry eyes, and headaches. However, persistent focusing difficulties that occur even during non-digital activities may indicate more serious underlying conditions. Presbyopia, the age-related decline in near focusing ability, typically begins in the mid-40s and progressively worsens, making it difficult to focus on close objects without reading glasses or bifocals. Accommodative insufficiency, a condition where the eye's focusing muscles don't work properly, can affect people of any age and may cause difficulty switching focus between near and