15 Hormonal Health Markers Women Should Track Throughout Their Lifetime
Understanding and monitoring hormonal health markers represents one of the most empowering steps a woman can take in managing her overall well-being throughout her lifetime. The intricate dance of hormones in the female body orchestrates everything from reproductive cycles and bone density to mood regulation and metabolic function. Unlike men, whose hormonal patterns remain relatively stable, women experience dramatic hormonal fluctuations during puberty, menstrual cycles, pregnancy, postpartum recovery, perimenopause, and menopause. These natural transitions create unique health considerations that require proactive monitoring and understanding. Research consistently demonstrates that women who actively track their hormonal markers experience better health outcomes, earlier detection of potential issues, and more effective treatment interventions. The fifteen key hormonal health markers we'll explore encompass reproductive hormones, stress indicators, metabolic regulators, and thyroid function markers that collectively paint a comprehensive picture of a woman's hormonal landscape. By developing literacy around these markers and establishing baseline measurements early in life, women can work collaboratively with healthcare providers to optimize their hormonal health, prevent disease, and maintain vitality across all life stages.
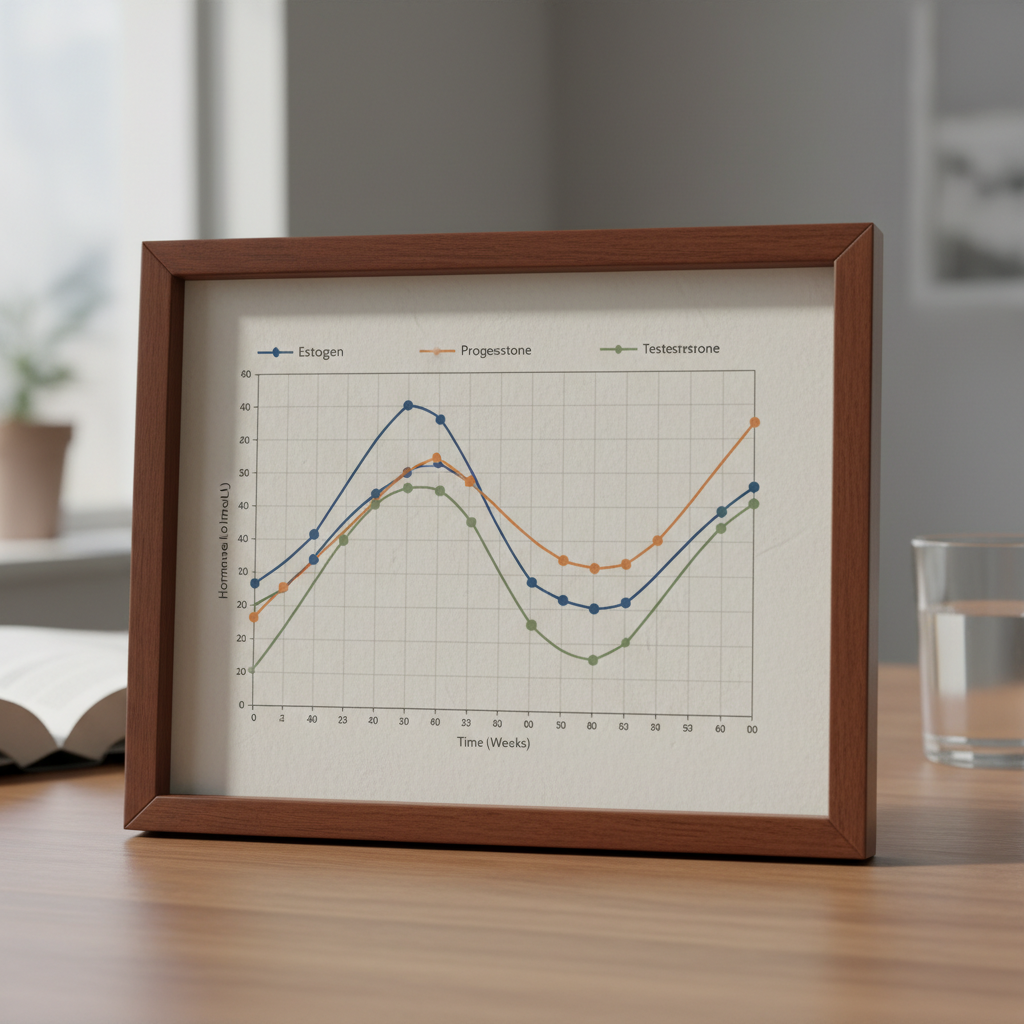
1. Estrogen - The Master Regulator of Female Reproductive Health

Estrogen stands as perhaps the most recognized and influential hormone in women's health, serving as the primary female sex hormone responsible for the development and regulation of the female reproductive system. This powerful hormone exists in three main forms: estradiol (the most potent during reproductive years), estrone (predominant after menopause), and estriol (elevated during pregnancy). Throughout a woman's lifetime, estrogen levels fluctuate dramatically, beginning with the surge during puberty that triggers breast development, hip widening, and the onset of menstruation. During reproductive years, estrogen levels rise and fall cyclically with each menstrual cycle, reaching peak levels just before ovulation to prepare the body for potential pregnancy. Beyond reproduction, estrogen plays crucial roles in maintaining bone density, supporting cardiovascular health, regulating cholesterol levels, and influencing mood and cognitive function. Research has shown that optimal estrogen levels are associated with improved memory, better skin elasticity, and enhanced overall vitality. However, both excessive and insufficient estrogen levels can lead to significant health complications, including increased risks of breast cancer, osteoporosis, cardiovascular disease, and mood disorders. Tracking estrogen levels through regular blood tests allows women to identify patterns, predict reproductive changes, and work with healthcare providers to address imbalances through lifestyle modifications, nutritional interventions, or hormone replacement therapy when appropriate.
2. Progesterone - The Pregnancy Hormone and Mood Stabilizer

Progesterone, often called the "pregnancy hormone," plays an equally vital role in women's hormonal health as estrogen's complementary partner. Produced primarily by the ovaries after ovulation and by the placenta during pregnancy, progesterone serves multiple critical functions beyond supporting pregnancy. This hormone prepares the uterine lining for potential implantation, maintains pregnancy by preventing uterine contractions, and supports breast tissue development. During the menstrual cycle, progesterone levels rise significantly after ovulation, creating the characteristic temperature increase that fertility awareness methods utilize for tracking. Beyond reproductive functions, progesterone acts as a natural mood stabilizer, promoting feelings of calm and well-being while supporting healthy sleep patterns through its interaction with GABA receptors in the brain. Research indicates that adequate progesterone levels are essential for maintaining emotional balance, particularly during the luteal phase of the menstrual cycle when many women experience premenstrual symptoms. Low progesterone levels can contribute to irregular menstrual cycles, difficulty conceiving, increased miscarriage risk, mood swings, anxiety, insomnia, and weight gain. Conversely, optimal progesterone levels support regular ovulation, healthy pregnancy outcomes, improved sleep quality, and emotional stability. Women can track progesterone through blood tests, saliva tests, or by monitoring basal body temperature patterns, with testing typically recommended during the luteal phase (approximately 7 days after ovulation) for the most accurate assessment of production levels.
3. Testosterone - The Underestimated Female Hormone
While testosterone is commonly associated with male physiology, it plays surprisingly important roles in women's health and should be monitored throughout a woman's lifetime. Women produce testosterone in smaller quantities than men, with production occurring in the ovaries, adrenal glands, and peripheral tissues. This hormone significantly influences libido, energy levels, muscle mass maintenance, bone density, and overall vitality in women. During reproductive years, testosterone levels naturally fluctuate with the menstrual cycle, typically peaking around ovulation to support increased sexual desire during the most fertile period. Research demonstrates that adequate testosterone levels in women contribute to improved sexual satisfaction, enhanced mood, increased motivation, better cognitive function, and maintained lean muscle mass. However, testosterone levels naturally decline with age, particularly after menopause when ovarian production decreases significantly. This decline can lead to reduced libido, decreased energy, muscle weakness, bone loss, and diminished overall quality of life. Conversely, excessive testosterone levels in women can indicate conditions such as polycystic ovary syndrome (PCOS), leading to symptoms including irregular periods, acne, excess hair growth, and difficulty maintaining healthy weight. Monitoring testosterone levels through blood tests helps women understand their individual patterns and work with healthcare providers to address imbalances. Treatment options may include lifestyle modifications, nutritional support, stress management, or in some cases, carefully monitored hormone replacement therapy to restore optimal levels and improve overall well-being.
4. Follicle Stimulating Hormone (FSH) - The Ovarian Function Indicator
Follicle Stimulating Hormone (FSH) serves as a crucial messenger between the brain and ovaries, making it an invaluable marker for assessing reproductive health and predicting life stage transitions. Produced by the anterior pituitary gland, FSH stimulates the growth and development of ovarian follicles, which contain the eggs released during ovulation. Throughout the menstrual cycle, FSH levels fluctuate in a carefully orchestrated pattern, rising during the early follicular phase to stimulate follicle development, then decreasing as estrogen levels rise in response to follicular growth. This hormone provides critical insights into ovarian reserve and function, making it particularly valuable for women planning pregnancies or experiencing fertility concerns. As women age, FSH levels gradually increase as the ovaries become less responsive to hormonal signals, requiring higher levels of stimulation to produce the same response. This natural aging process accelerates during perimenopause, when FSH levels can fluctuate wildly before ultimately remaining elevated after menopause when ovarian function ceases. Elevated FSH levels may indicate diminished ovarian reserve, approaching menopause, or other reproductive health concerns, while abnormally low levels might suggest pituitary dysfunction or hypothalamic suppression. Regular monitoring of FSH levels helps women understand their reproductive timeline, make informed decisions about family planning, and prepare for menopausal transitions. Healthcare providers often use FSH measurements in conjunction with other hormonal markers to assess fertility potential, diagnose reproductive disorders, and determine appropriate treatment strategies for various life stages.
5. Luteinizing Hormone (LH) - The Ovulation Trigger
Luteinizing Hormone (LH) works in concert with FSH to regulate the menstrual cycle and plays the starring role in triggering ovulation, making it an essential marker for women tracking their reproductive health. Like FSH, LH is produced by the anterior pituitary gland and follows a predictable pattern throughout the menstrual cycle. The most significant event in LH's monthly cycle is the dramatic surge that occurs approximately 24-36 hours before ovulation, when LH levels can increase by 3-10 times their baseline levels. This LH surge triggers the release of the mature egg from the dominant follicle and stimulates the formation of the corpus luteum, which subsequently produces progesterone. Understanding and tracking LH patterns is particularly valuable for women trying to conceive, as the LH surge represents the most fertile period of the cycle. Many home ovulation prediction kits detect this LH surge in urine, providing women with advance notice of their most fertile days. Beyond fertility tracking, LH levels provide important information about overall reproductive health and can help diagnose various conditions. Elevated baseline LH levels may indicate polycystic ovary syndrome (PCOS), particularly when combined with elevated testosterone levels. During perimenopause and menopause, LH levels increase significantly as the body attempts to stimulate increasingly unresponsive ovaries. Abnormally low LH levels might suggest pituitary dysfunction, hypothalamic suppression from stress or excessive exercise, or eating disorders. Regular monitoring of LH patterns helps women optimize their fertility timing, understand their reproductive health status, and identify potential hormonal imbalances that may require medical attention.
6. Thyroid Stimulating Hormone (TSH) - The Metabolic Master Switch
Thyroid Stimulating Hormone (TSH) serves as the primary regulator of thyroid function and represents one of the most important hormonal markers for women to monitor throughout their lifetime. Produced by the pituitary gland, TSH stimulates the thyroid gland to produce thyroid hormones T3 and T4, which control virtually every aspect of metabolism, energy production, and cellular function. Women are significantly more likely than men to develop thyroid disorders, with research indicating that up to 20% of women will experience thyroid dysfunction during their lifetime. The intricate relationship between TSH and thyroid hormones operates on a negative feedback loop: when thyroid hormone levels are low, TSH increases to stimulate more production, and when thyroid hormones are adequate, TSH decreases accordingly. This makes TSH an extremely sensitive marker for detecting thyroid dysfunction, often showing changes before symptoms become apparent. Elevated TSH levels typically indicate hypothyroidism (underactive thyroid), which can cause symptoms including fatigue, weight gain, depression, hair loss, cold intolerance, and irregular menstrual periods. Conversely, suppressed TSH levels may indicate hyperthyroidism (overactive thyroid), leading to symptoms such as anxiety, rapid heartbeat, weight loss, heat intolerance, and sleep disturbances. Thyroid dysfunction can significantly impact reproductive health, affecting menstrual regularity, fertility, and pregnancy outcomes. Additionally, thyroid disorders often develop or worsen during periods of hormonal change, such as postpartum or menopause, making regular monitoring particularly important during these transitions. Optimal TSH levels support healthy metabolism, stable energy levels, regular menstrual cycles, and overall well-being, making this marker essential for comprehensive women's health assessment.
7. Free T3 and T4 - The Active Thyroid Hormones

While TSH provides valuable information about thyroid function, measuring the actual thyroid hormones T3 (triiodothyronine) and T4 (thyroxine) offers deeper insights into thyroid health and metabolic function. T4 is the primary hormone produced by the thyroid gland, but it must be converted to T3, the more active form, to exert its metabolic effects on cells throughout the body. Free T3 and free T4 measurements are particularly important because they represent the unbound, biologically active portions of these hormones that are available for cellular uptake and utilization. Many women experience symptoms of thyroid dysfunction despite having normal TSH levels, making free T3 and T4 measurements crucial for comprehensive thyroid assessment. T4 serves as a prohormone, requiring conversion to T3 primarily in the liver, kidneys, and other peripheral tissues through the action of deiodinase enzymes. This conversion process can be impaired by various factors including stress, illness, certain medications, nutritional deficiencies (particularly selenium and zinc), and genetic variations. When conversion is compromised, women may have adequate T4 levels but insufficient T3, leading to persistent hypothyroid symptoms despite normal standard thyroid tests. Free T3 is considered the most metabolically active thyroid hormone, directly influencing cellular energy production, protein synthesis, and metabolic rate. Optimal free T3 levels support healthy weight management, stable energy throughout the day, normal body temperature regulation, and proper cognitive function. Low free T3 levels can contribute to fatigue, brain fog, depression, cold intolerance, and difficulty losing weight, even when TSH and T4 levels appear normal. Monitoring both free T3 and T4 alongside TSH provides a comprehensive picture of thyroid function and helps identify conversion issues that might otherwise go undetected.
8. Cortisol - The Stress Response Hormone
Cortisol, often called the "stress hormone," plays a fundamental role in women's health and represents a critical marker for assessing adrenal function and stress response throughout life. Produced by the adrenal glands in response to stress and following a natural circadian rhythm, cortisol affects virtually every system in the body, influencing metabolism, immune function, blood pressure regulation, and inflammatory responses. Under normal circumstances, cortisol levels follow a predictable daily pattern, rising sharply upon waking (cortisol awakening response), peaking within the first hour after awakening, then gradually declining throughout the day to reach their lowest levels in the evening. This natural rhythm supports healthy energy patterns, with morning cortisol providing the energy needed to start the day and evening decline allowing for restful sleep. However, chronic stress, poor sleep, irregular eating patterns, excessive exercise, or underlying health conditions can disrupt this delicate balance, leading to either chronically elevated cortisol (hypercortisolism) or depleted cortisol production (hypocortisolism or adrenal fatigue). Elevated cortisol levels can contribute to weight gain (particularly around the midsection), insulin resistance, high blood pressure, mood disorders, suppressed immune function, and disrupted reproductive hormones. Women with chronically high cortisol often experience irregular menstrual cycles, reduced fertility, and accelerated aging. Conversely, insufficient cortisol production can lead to extreme fatigue, low blood pressure, salt cravings, difficulty handling stress, and compromised immune function. The relationship between cortisol and other hormones is particularly important for women, as elevated cortisol can suppress reproductive hormone production and interfere with thyroid function. Monitoring cortisol through saliva tests (which measure free, active cortisol) or 24-hour urine tests provides valuable insights into stress response patterns and helps guide interventions to restore healthy adrenal function.
9. DHEA-S - The Youth and Vitality Hormone

Dehydroepiandrosterone sulfate (DHEA-S) represents one of the most abundant hormones in the human body and serves as a crucial precursor to both male and female sex hormones, making it an important marker for assessing overall hormonal health and aging. Produced primarily by the adrenal glands, DHEA-S levels peak during a woman's twenties and then gradually decline with age, decreasing by approximately 10% per decade. This natural decline is so consistent that DHEA-S levels are often considered a biomarker of biological aging. Unlike many other hormones that fluctuate throughout the menstrual cycle, DHEA-S levels remain relatively stable, making it easier to track and interpret. This hormone serves multiple important functions in women's health, including supporting immune function, maintaining bone density, promoting healthy skin and hair, enhancing mood and cognitive function, and serving as a buffer against the negative effects of cortisol. Research indicates that optimal DHEA-S levels are associated with increased energy, improved stress resilience, better mood stability, enhanced libido, and overall feelings of vitality and well-being. The relationship between DHEA-S and cortisol is particularly significant, as these hormones often work in opposition to each other. While cortisol rises in response to stress and can have catabolic (tissue-breaking-down) effects, DHEA-S provides anabolic (tissue-building) support and helps counterbalance cortisol's potentially harmful effects. Low DHEA-S levels may contribute to increased susceptibility to stress, reduced immune function, accelerated aging, decreased bone density, mood disorders, and reduced overall vitality. Some women may benefit from DHEA supplementation under medical supervision, particularly those with significantly low levels or those experiencing symptoms of premature aging or chronic fatigue. However, it's important to monitor levels carefully, as excessive DHEA can convert to androgens and cause unwanted side effects such as acne or excess hair growth.
10. Insulin - The Blood Sugar and Weight Management Hormone
Insulin, while not traditionally considered a reproductive hormone, plays an increasingly recognized role in women's hormonal health and represents a crucial marker for metabolic wellness throughout life. Produced by the pancreas in response to rising blood glucose levels, insulin's primary function is to facilitate the uptake of glucose into cells for energy production and storage. However, insulin's influence extends far beyond blood sugar regulation, significantly impacting reproductive hormones, weight management, and overall metabolic health. Women are particularly susceptible to insulin resistance, a condition where cells become less responsive to insulin's signals, requiring higher levels of the hormone to maintain normal blood glucose. This resistance can develop due to various factors including genetics, sedentary lifestyle, poor diet, chronic stress, hormonal changes during menopause, and certain medical conditions. Insulin resistance is strongly linked to polycystic ovary syndrome (PCOS), affecting up to 70% of women with this condition and contributing to irregular menstrual cycles, elevated androgen levels, and difficulty conceiving. The relationship between insulin and reproductive hormones is bidirectional: insulin resistance can disrupt normal ovarian function and hormone production, while hormonal changes (such as those occurring during menopause) can increase insulin resistance. Elevated insulin levels promote fat storage, particularly in the abdominal area, and can make weight loss extremely challenging. Additionally, chronically high insulin levels contribute to inflammation, increase the risk of type 2 diabetes and cardiovascular disease, and can accelerate cellular aging. Monitoring insulin levels through fasting insulin tests or glucose tolerance tests with insulin measurements provides valuable insights into metabolic health and can help identify insulin resistance before it progresses to diabetes. Women with optimal insulin sensitivity typically experience more stable energy levels, easier weight management, regular menstrual cycles, and reduced risk of metabolic disorders.